The Dawn of Training Programs in Africa
Images
A key driver of global radiology disparities is the lack of trained professionals and a lack of formal training programs, despite the increasing availability of previously cost-prohibitive radiology equipment.1
In Africa, limited access to radiology training programs is severe at both the diagnostic radiology (DR) residency and radiology subspecialty (RS) fellowship levels. Of 54 African sovereign countries (excluding disputed territories), only 18 have well-established DR residency programs, and only 8 report any subspecialty programs, with details readily available for only 5 of those 8 countries: Egypt, Ethiopia, Kenya, South Africa, and Tanzania.2
The earliest one-year RS programs, for interventional radiology (IR) and pediatric radiology, were established in South Africa in 2002 and 2009, respectively; both bestow postgraduate diplomas.2 Interventional Radiology (IR) training in Egypt consists of institution-based clinical apprenticeships, with an optional subsequent pathway for certification by the Egyptian Board of Interventional Radiology following written and oral examinations.3
Four two-year radiology fellowship training programs in Ethiopia, Kenya, and Tanzania have been established within the past ten years. We will describe initiation of IR and Neuroradiology fellowship programs in Tanzania, with comparisons to Pediatric Radiology in Ethiopia (2015) and IR in Kenya (2020).4,5 These four fellowship programs offer lessons on how to accelerate the development of RS training programs in Africa.
Tanzania
Interventional Radiology Fellowship
In 2017, an IR Readiness Assessment at Muhimbili National Hospital (MNH) in Dar es Salaam revealed a complete lack of trained IR personnel and disposable equipment as their two main obstacles to initiating IR service.6,7
Beginning in October 2018, through close collaboration among MNH, Muhimbili University of Health and Allied Sciences (MUHAS), and multiple US institutions including Yale and Emory Universities under the Road2IR consortium, rotating teams of IR faculty, nurses, and technologists were deployed to MNH for hands-on teaching.
A two-year Master of Science (MSc) Interventional Radiology curriculum was approved by MUHAS in 2019 and the first three IR trainees were enrolled.7 To date, 48 faculty have traveled to Tanzania, most accompanied by nurses, technologists, medical students, and/or residents, once a month, on average.
The first three IR fellows graduated in 2021, with the next class of seven expected to graduate in August 2022. In addition, three Tanzanian IR nurses and three technologists have completed training, with additional nurses and technologists joining the program this year, helping to expand IR services to other hospitals in Tanzania.
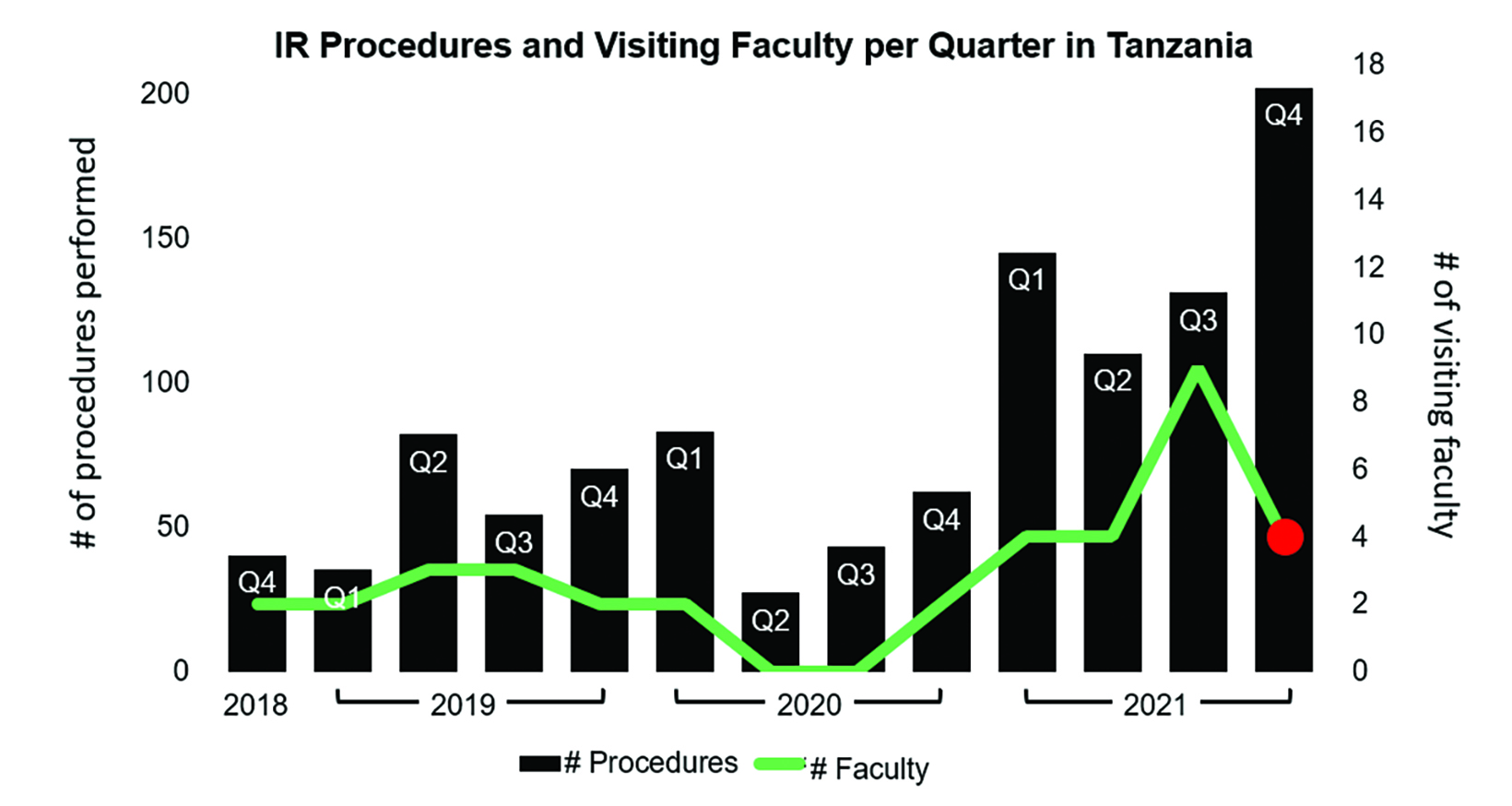
MNH now offers nearly a full spectrum of IR procedures, ranging from core needle biopsies and abscess drainages to transarterial chemoembolization (TACE) and transjugular intrahepatic portosystemic shunts (TIPS).8,9 Most of these procedures are provided year-round and are no longer limited by availability of visiting faculty, which confirms the feasibility and success of this training model utilizing rotating IR teaching teams (Figure).
Neuroradiology Fellowship
The success of the IR program created demand for additional subspecialty programs at MNH/MUHAS. The highest demand was for neuroradiology, given the complexity of cases seen at MNH, a tertiary referral center with a busy neurosurgery and neurology clinical services.
The MUHAS approved a two-year MSc Neuroradiology curriculum supported by rotating visiting faculty, enrolling two inaugural fellows in 2020. During the first year, the fellows were mentored by two faculty from the Radiological Society of North America (RSNA) Global Learning Center (GLC) program. The MSc Neuroradiology training consists of daily clinical practice, virtual case review sessions, weekly didactic lecture sessions, and assessment examinations each semester.
In addition, the fellows are embedded in daily clinical practice at MNH and supervised by local attendings. During their first year, the fellows logged more than 1,000 clinical cases and participated in more than 50 virtual, one-hour case review sessions, which discussed more than 250 of their most challenging clinical cases. The fellows prepared weekly didactic lectures and presented at multi-disciplinary clinical meetings with neurosurgery, neurology, and pathology colleagues. On-site visits by the faculty mentors were limited by COVID-19 pandemic travel restrictions. This first class will graduate in late 2022.
The second class of two neuroradiology fellows enrolled in 2021. The RSNA GLC program has expanded the volunteer faculty mentors from two to twelve, offering regular virtual case-review sessions three times per week. The neuroradiology fellowship provides both in-country subspecialty training and regular virtual consultation for challenging neuroradiology cases, to the immediate benefit of both MNH trainees and patients.
Ethiopia and Kenya
The pediatric fellowship program in Ethiopia was accredited in 2015 by Addis Ababa University in partnership with Children’s Hospital of Philadelphia and other collaborating institutions. Two inaugural fellows graduated in 2017, and a second cohort began training in 2019.4
The Kenyan IR fellowship was accredited by the University of Nairobi in 2019 in partnership with University of North Carolina and RAD-AID International and enrolled its first two trainees in 2020.5,10 This fellowship is supported by three in-country attendings and an established IR service, compared to the Tanzanian program, which had neither attendings nor IR service at its inception.
RAD-AID International supplements the Kenyan attendings with volunteer faculty, nurses, and technologists who are deployed two to four times per year.10
Ingredients for Program Success
All four recently established fellowship programs in Ethiopia, Kenya, and Tanzania have demonstrated the feasibility of sub-specialty programs, even without local subspecialists. The programs share three key characteristics that have contributed to their success:
- Each program underwent a rigorous accreditation process by a local university;
- The primary training site for each is located in the host country;
- Each leveraged strong collaboration with an international institution or organization to help mobilize and coordinate volunteer faculty and staff.
The two-year fellowship programs provide ample time and structure for trainees to gain the necessary competencies in their subspecialties, compared to unstructured clinical apprenticeships or short-term observer-based models.3,11
Providing in-country training opportunities is a critical step toward addressing the severe radiology disparities in Africa. Adapted to local conditions, these three key ingredients of the programs could help to accelerate subspecialty programs in Africa.
References
- Mollura DJ, Lungren MP, eds. Radiology in Global Health: Strategies, Implementation, and Applications. New York, NY: Springer, 2014. http://link.springer. com/10.1007/978-1-4614-0604-4. Accessed May 23, 2022.
- Iyawe EP, Idowu BM, Omoleye OJ. Radiology subspecialisation in Africa: A review of the current status. S Afr J Rad. 2021;25(1):2168.
- El Tawab KA, Wahab SM. The status of interventional radiology training: The Egyptian experience. Arab J Intervent Radiol. 2020;4:3.
- Zember J, Reid J, Gorfu Y, Solomon DZ, Darge K. Pediatric radiology fellowship creation as an international education outreach effort in Ethiopia. J Grad Med Educ. 2020 Feb;12(1):98-103.
- >Brown B, Culp M, Olabu BO, et al. Meeting the need for IR training in Kenya. J Vasc Interv Radiol. 2020;31(11):1929-1932.e1.
- Kline AD, Dixon RG, Brown MK, et al. Interventional radiology readiness assessment tool for global health. J Global Radiol. 2017; 3.
- Laage Gaupp FM, Solomon N, Rukundo I, et al. Tanzania IR initiative: training the first generation of interventional radiologists. J Vasc Interv Radiol.2019;30(12):2036-2040.
- Mbuguje EM, Alswang JM, Rukundo I, et al. Safety and effectiveness of transthoracic core needle biopsy in a newly established interventional radiology program in Tanzania. Arab J Intervent Radiol 2021;5:82-87.
- Rukundo I, Mbuguje E, Naif A, et al. Establishment of a percutaneous nephrostomy service to treat obstructive uropathy secondary to cervical cancer in Tanzania. Arab J Intervent Radiol 2022; DOI: 10.1055/s-0042-1744507
- McKenney AS, Garg T, Kim E, Kesselman A. Addressing global radiology disparities: increasing access to interventional radiology education. Radiographics. 2021 Sep-Oct;41(5):E142-E144.
- Sharma S, Ganga K. Establishing IR in emerging countries: a skill development initiative. J Vasc Interv Radiol 2019;30(6):956-960.
References
Citation
FJ M, MC M, FML G. The Dawn of Training Programs in Africa. Appl Radiol. 2022;(4):34-41.
July 14, 2022