A simplified approach to the spaces of the suprahyoid neck
Images














The spaces of the suprahyoid neck were originally described by anatomists and surgeons in the 19th century as they dissected the layers of the deep cervical fascia, attempting to better understand the extension of infections of the extracranial head and neck to other areas in the neck, chest, and abdomen.1 This led to detailed categorization and descriptions of the cervical fascia and numerous soft tissue spaces that have been used by anatomists and otolaryngologists. However, due to the complexity and confusing array of terminology used to describe the deep cervical fascia, radiologists did not commonly use it.1,2
The advent of CT and MRI allowed radiologists to better visualize the complex anatomy and pathology of the suprahyoid neck. Then in the late 1980s and early 1990s, the spaces concept in the neck was reintroduced from a radiologic perspective, which enabled the radiologists to better understand the spaces of the neck and their components (Table 1).2 - 8 This article will present a discussion of each of the various spaces of the suprahyoid neck, along with a list of differential diagnoses pertinent to that space based on its anatomical contents.
Spaces of the suprahyoid head, neck and fascia
The two main fascial layers of the suprahyoid neck are the superficial cervical fascia and the deep cervical fascia (DCF). The superficial cervical fascia consists of the subcutaneous tissues of the head and neck. The DCF consists of the superficial, middle and deep layer. The middle layer (visceral or pharyngomucosal) encloses the pharynx, which includes the oropharynx and the nasopharynx. The deep layer (prevertebral) is posterior to the visceral fascia and defines the contents of the prevertebral space (PVS).9
Visceral space
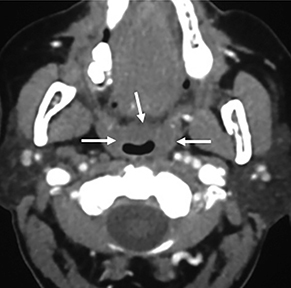
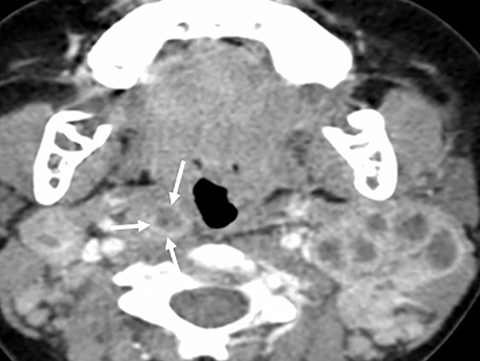
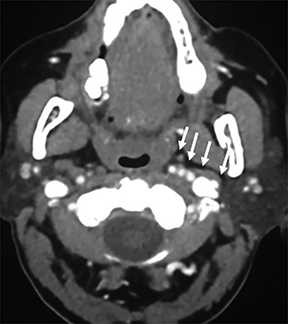
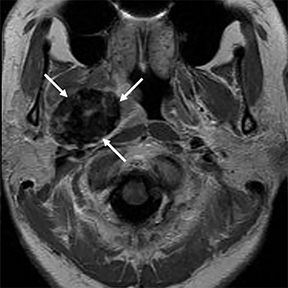
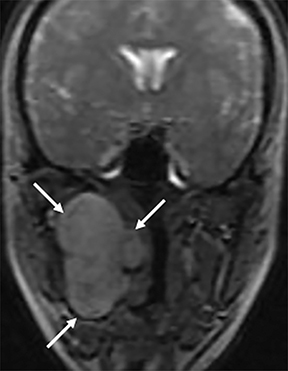
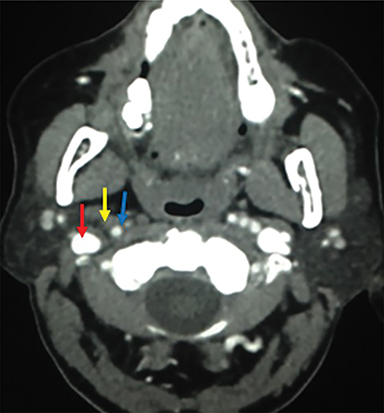
In the suprahyoid neck, the contents of the visceral space are the naso- and oropharynx, which have an epithelial lining (Figure 1A). In the infrahyoid neck, the fascia encircles the hypopharynx, larynx, and thyroid. Some of the important contents of the suprahyoid neck are the mucosa, lymphoid tissue of Waldeyer’s ring (adenoids, tonsils), and minor salivary glands.2
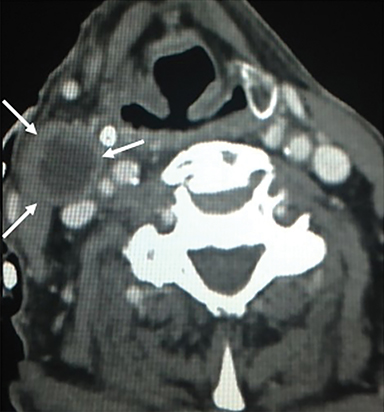
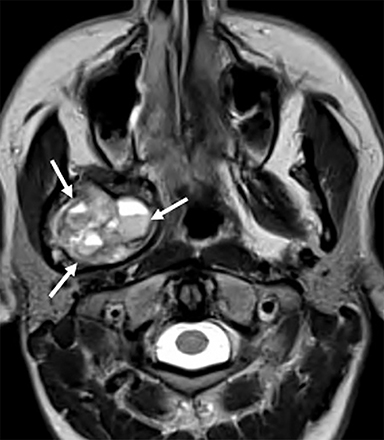
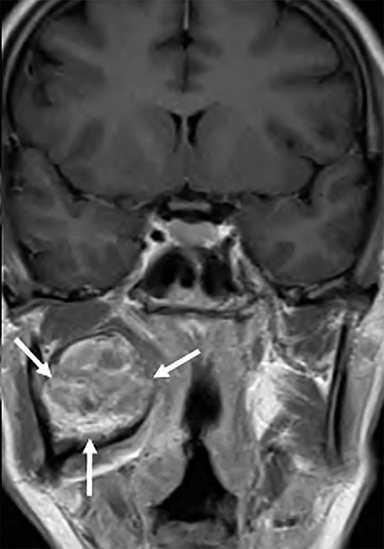
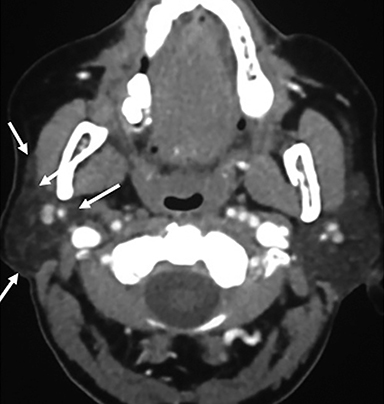
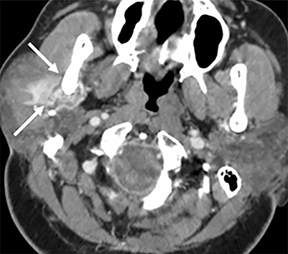
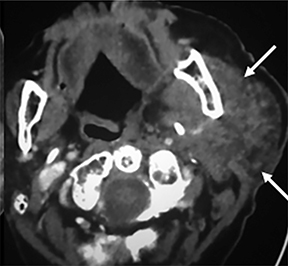
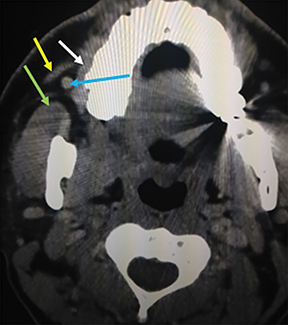
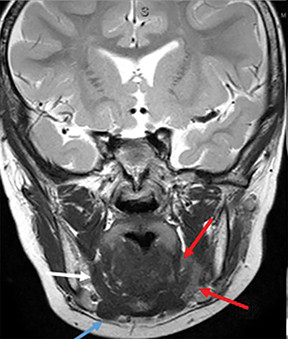
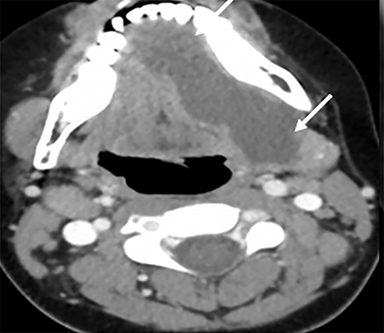
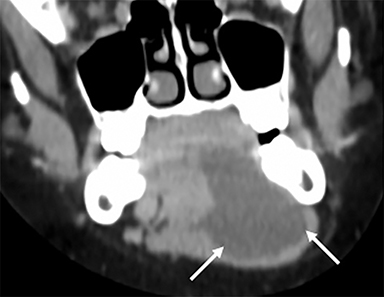
Some of the pathological processes that can occur within this space include malignant tumors, inflammatory lesions, infectious causes (tonsillar or peritonsillar abscess) and musculoskeletal tumors (Figures 1B, 2). With the epithelial lining, the most common malignancy in the visceral space is squamous cell carcinoma (SCC).2, 5, 10, 11 The lymphatic tissue in the Waldeyer’s ring can give rise to non-Hodgkin’s lymphoma, the second-most common malignancy in the PMS.2 The minor salivary glands can also give rise to both benign and malignant tumors.
Retropharyngeal space
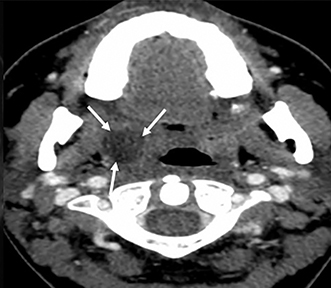
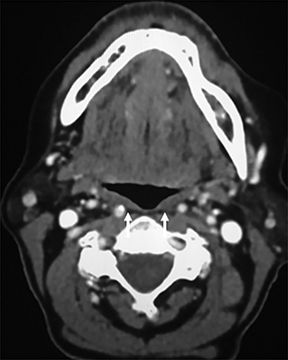
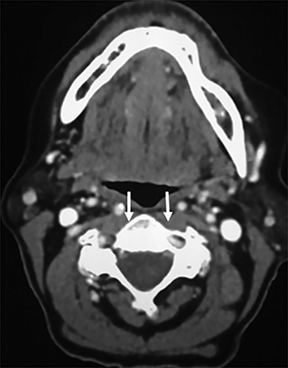
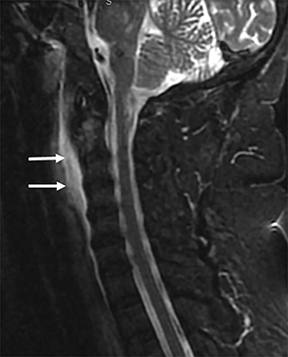
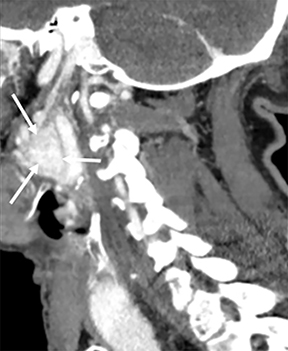
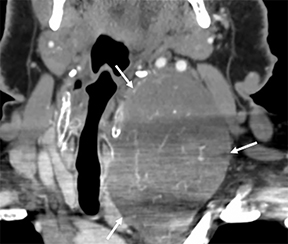
The retropharyngeal space (RPS) is bordered anteriorly by the visceral fascia and posteriorly by the prevertebral fascia and is commonly referred to as the “danger space.”1 A thin fascial layer (alar fascia) divides the RPS into anterior and posterior compartments. The anterior compartment extends from the skull base inferiorly to where the alar fascia fuses with the visceral fascia and the posterior compartment, the “danger space” that extends from the skull base to the diaphragm.1, 2, 4, 9 The contents of the RPS are fat and retropharyngeal lymph nodes (RPLN), sometimes referred to as the nodes of Rouviere (Figure 3A).
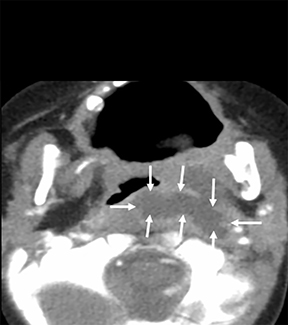
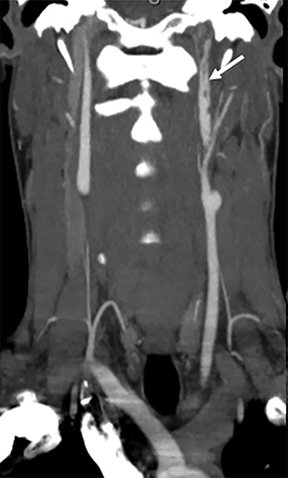
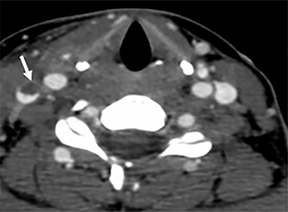
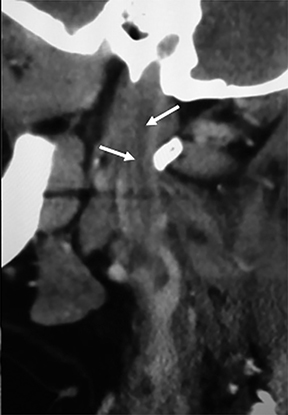
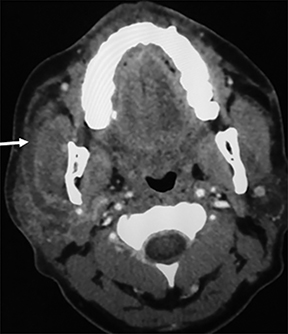
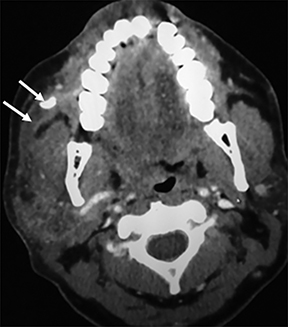
The differential diagnoses for primary retropharyngeal processes include edema, cellulitis and abscess (Figures 3B and 3C). Differential diagnoses for secondary extension into the RPS include direct extension from squamous cell carcinoma, tortuous carotid artery, lipoma, hemangioma, diskitis and osteomyelitis from the prevertebral space. For the lymph nodes, differential diagnoses include reactive adenopathy, suppurative adenitis, metastatic adenopathy, and lymphoma (Figure 4).1
Prevertebral space
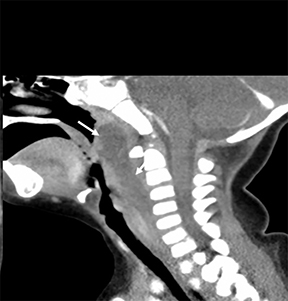
The prevertebral space (PVS) is posterior to the retropharyngeal space and is enclosed by the prevertebral fascia.1 The anatomic components of the PVS in the suprahyoid neck include the following: Prevertebral muscles (longus colli capitus), vertebral body, cervical disk, spinal canal, vertebral artery and phrenic nerve (Figure 5A). Some of the main pathologic processes arising from or involving the PVS contents include: benign and malignant mesenchymal tumors, calcific tendinitis, osteophytes, osteomyelitis, primary bone tumors, metastases, diskitis, anterior disk herniation, aneurysm, lymphoma, and direct extension of carcinoma of the nasopharynx (Figures 5B and 5C).2, 5 The most common PVS malignancy in children is a rhabdomyosarcoma. This tumor can be difficult to differentiate from a neuroblastoma that arises from the sympathetic chain, located in the adjacent carotid space.
Parapharyngeal space
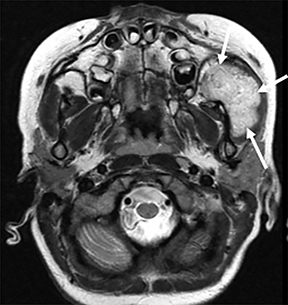
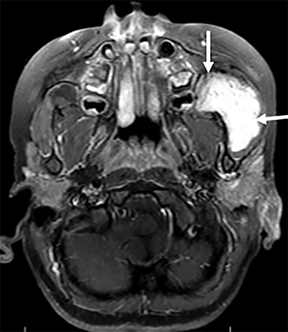
The parapharyngeal space (PPS), also known as the prestyloid PPS, is next to the pharynx and extends from the skull base to the hyoid bone.1 - 4, 12 The contents of the PPS includes fat, vascular structures, small branches of the fifth cranial nerve, lymph nodes and ectopic rests of minor salivary gland tissue1 (Figure 6A). The primary PPS masses usually displace the lateral wall of the visceral space medially, the deep lobe of the parotid gland laterally, and the contents of the CS posteriorly. It is also important to differentiate a primary PPS mass from a mass arising from the deep lobe of the parotid because nonvascular masses localized to the PPS may be resected via a submandibular cervical approach while a deep parotid lobe mass might require a total parotidectomy.1
Some of the primary PPS masses include minor salivary gland tumors arising from ectopic salivary gland tissue rests, atypical type II first branchial cleft anomaly, and lipomas. Secondary PPS masses include deep spread of malignant tumor from adjacent spaces, SCC from the visceral space, sarcoma from the MS (masticator space), minor salivary gland tumor from PS or PPS abscess (odontogenic infection from the MS, or tonsil infection).1 Primary PPS masses are unusual and the most common primary lesion of the PPS is a minor salivary gland tumor (Figure 6B and 6C). The most common lesions in the PPS result from secondary extension of pathologic processes arising from the adjacent spaces and the most pathology is deep extension of SCC arising in the tonsillar region.1
Carotid space
The carotid space, also known as the post styloid PPS or the carotid sheath, is located posterior to the styloid process and lateral to the RPS and PVS.2, 3, 9, 13 Its sheath extends superiorly to the jugular foramen and inferiorly to the aortic arch and is bordered anteriorly by the styloid process and PPS, laterally by the anterior belly of the digastric muscle and the PS and medially by the lateral margin of the RPS. It contains the internal carotid artery, internal jugular vein, sympathetic chain, cranial nerves IX to XII and lymph nodes (Figure 7A).1 Most of the pathology involving the carotid sheath are those that originate from the carotid space (Figures 8 and 9) . Enlarged lymph nodes are the most common pathology of the carotid sheath (Table 2). In children the most common primary malignancy of the carotid sheath is a neuroblastoma.1
Masticator space
The masticator space (MS) contains muscles of mastication (medial and lateral pterygoid, masseter, and temporalis), ramus of the mandible and the third division of the cranial nerve V (Figure 10A).1 - 4, 14, 15 It extends inferiorly to the attachment of the medial pterygoid and masseter muscles to the mandible and the superomedial margin of the MS at the skull base. The superomedial margin of the masticator space includes soft tissues inferior to the foramen ovale so any malignancy involving the MS has potential to extend to the cavernous sinus via retrograde perineural spread along cranial nerve V3.1 The anatomically-based differential diagnosis is referenced in Table 3.
Parotid space
The parotid space (PS) contains the parotid gland and is divided into superficial and deep lobes by the facial nerve which is located just lateral to the retromandibular vein (Figure 12).2 - 4, 9,16 The contents include gland parenchyma, facial nerve, retromandibular vein, external carotid artery, and intra parotid lymph nodes. The anatomically based differential diagnosis is shown in Table 4.
Buccal space
The buccal space (BS) does not have complete fascial coverings and is bordered medially by the buccinators muscle, MS posteriorly, PS laterally and anteriorly. It is separated from the subcutaneous tissues of the face by the plane formed by the superficial muscle of facial expression and the investing fascia1 (Figure 14A). The contents of the BS are adipose tissue, minor salivary gland tissue, parotid duct, lymph nodes, fascial vein, facial and buccal artery, buccal branch of the cranial nerve VII, buccal division of the mandibular division of cranial nerve V. The differential diagnosis for the contents are as follows: SCC (direct extension or nodal metastases), lymphoma, minor salivary gland tumors, lipoma, hemangioma, sarcoma, sebaceous cyst, fibromatosis, obstructed duct, accessory parotid tissue, cellulitis and abscess (Figures 14B and 14C).1
Sublingual space
The sublingual space (SLS), referred to as the floor of mouth, is the space located below the tongue and confined by the mylohyoid muscle and hyoid bone (Figure 15A). The contents of the SLS include muscles, the hypoglossal nerve, the lingual nerve, lingual artery and vein, sublingual gland and ducts, the deep portion of the submandibular gland and duct and lymph nodes.1 The differential diagnoses for the contents are as follows: SCC from the epithelial lining, minor salivary gland tumors, ranula, obstructed submandibular duct, abscess, ludwig’s angina, neurogenic tumor, lingual thyroid, thyroglossal duct cyst, hemangioma, lymphangioma, dermoid/epidermoid (Figures 15B and C).1
Submandibular space
The submandibular space (SMS) is located below the mandible, inferior to the mylohyoid muscle and the inferior margin is the hyoid bone (Figure 15A). The posterior portion of the SMS is in direct communication with posterior aspect of the SLS. The contents of the SMS are: anterior belly of the digastric muscle, superficial portion of the submandibular gland, submandibular and submental lymph nodes, facial artery and vein, fat, and the inferior loop of the hypoglossal nerve.1 The differential diagnoses for the contents are as follows: metastatic disease, lymphoma, adenitis, obstructed submandibular duct, salivary gland tumors, abscess, Ludwig’s angina, thyroglossal duct cyst, hemangioma, lymphangioma, dermoid/epidermoid, diving ranula (complex), second branchial cleft cyst (more common in children) (Figure 16).1
Conclusion
Contrary to popular belief, the spaces of the head and neck were not created to torture residents studying for their boards. Rather, a proper understanding of the anatomical spaces of the neck can aid considerably in formulating a differential diagnosis of pathologic processes involving the contents of that space and providing better care for our patients.
References
- Mukherji SK, Castillo M. A simplified approach to the spaces of the suprahyoid neck. Radiol Clin North Am. 1998; 36(5):761-780.
- Harnsberger HR. Handbook of Head and Neck Imaging. 2nd ed. St.Louis, MO: Mosby; 1995:3-28.
- Davis WL, Smoker WR, Hamsberger HR. The normal and diseased retropharyngeal and prevertebral spaces. Semin Ultrasound CT MR. 1990; 11(6):520-523.
- Davis WL, Smoker WR, Hamsberger HR The normal and diseased infrahyoid retropharyngeal, danger, and prevertebral spaces. Semin Ultrasound CT MR. 1991; 12(3):241-256.
- Harnsberger HR. Head and Neck Imaging. Littleton, MA: Year Book Medical Publishers; 1990.
- Harnsberger HR, Osbom AG. Differential diagnosis of head and neck lesions based on their space of origin. 1. The suprahyoid part of the neck. AJR Am J Roentgenol. 1991; 157(1):147-154.
- Smoker WR, Hamsberger H R. Differential diagnosis of head and neck lesions based on their space of origin. 2. The infrahyoid portion of the neck. AJR Am J Roentgenol. 1991; 157(1):155-159.
- Velpeau A. A Treatise on Surgical Anatomy or the Anatomy of the Regions, vol one. New York: Samuel Wood and Sons; 1830
- Grodinsky M, Holyoke EA. The fasciae and fascial spaces of the head, neck and adjacent regions. Am J Anat. 1938; 63(3):367-408.
- Parker GD, Hamsberger HR, Jacobs JM. The pharyngeal mucosal space. Semin Ultrasound CT MR. 1990; 11(6):460-475.
- Vogelzang P, Hamsberger HR, Smoker WR. Multi-spatial and transpatial diseases of the extracranial head and neck. Semin Ultrasound CT MR. 1991; 12(3)274-287.
- Babbel RW, Harnsberger HR. The paraphyaryngeal space: the key to unlocking the suprahyoid neck. Semin Ultrasound CT MR. 1990;11(6):444-459.
- Fruin ME, Smoker WR, Harnsberger HR. The carotid space in the suprahyoid neck. Semin Ultrasound CT MR. 1990; 11(6):504-519.
- Braun IF, Hoffman JC. Computed tomography of the buccomasseteric region. AJNR Am J Neuroradiol. 1984; 5(5):605-610.
- Tryhus MR, Smoker WR, Harnsberger HR. The normal and diseased masticator space. Semin Ultrasound CT MR. 1990; 11(6):476-485.
- Pollei SR, Harnsberger H. The radiologic evaluation of the parotid space. Semin Ultrasound CT MR. 1990; 11(6):486-503.
Citation
IR M, SK M. A simplified approach to the spaces of the suprahyoid neck. Appl Radiol. 2017;(4):6-14.
April 3, 2017