Bariatric embolization: Does it carry any weight?
Images
Obesity has become an epidemic not only in the United States, but throughout the world. More than 1/3 of Americans are now considered obese based on a BMI >30. Recently it was discovered that 1/3 of the world population is either obese or overweight. Obesity is associated with a host of diseases and conditions, including diabetes, heart disease, hypertension, cancer, sleep apnea, venous stasis disease and osteoarthritis. Collectively, obesity-related diseases constitute the fifth-leading cause of death in the United States. Life expectancy is predicted to decrease in the future as a result of the obesity epidemic.
Ghrelin is the only known orexigenic, or appetite-stimulating, hormone. Its existence was first reported in 1996; 90% of the hormone is produced in the fundus of the stomach. Ghrelin production increases prior to food intake and decreases after eating. It also increases as a result of chronically reduced food intake, such as dieting.
The first animal experiments designed to reduce ghrelin production and cause reduced appetite were first reported in 2007 and 2008 by Arvind Arepally, MD, at Johns Hopkins University. Dr. Arepally found that embolizing the arteries supplying the fundus of the stomach with sodium morhulate, a sclerosant, resulted in blunted weight gain and decreased ghrelin levels in otherwise rapidly growing juvenile swine.1,2 A follow-up study in 2012 by Paxton and Arepally using 40-micron particles demonstrated similar results, but with significant complications (ulcers, gastritis, and distal esophageal stricture).3
Bawudun et al (2012) described a technique of left gastric embolization using a mixture of bleomycin and lipiodol versus polyvinyl alcohol 500- to 700-micron particles to create weight loss in a canine model without gastric ulceration at 8 weeks. In addition, these researchers demonstrated significant reduction in subcutaneous fat and plasma ghrelin.
Left gastric-artery embolization has been performed since the early 1970’s for the treatment of life-threatening gastric hemorrhage. In 2013, a retrospective study of patients who underwent left gastric artery embolization demonstrated 8% body weight loss at 3 months compared to controls.4 The first human experience was reported in 2013 by Dr. Nicholas Kipshidze in the Georgian Republic.5 Dr. Kipshidze demonstrated an average loss of 49 lbs (16% of total body weight) at 24 months in 5 morbidly obese (BMI>40) patients with no complications.6
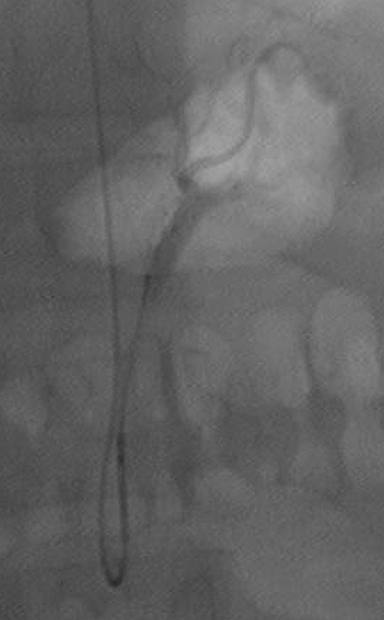
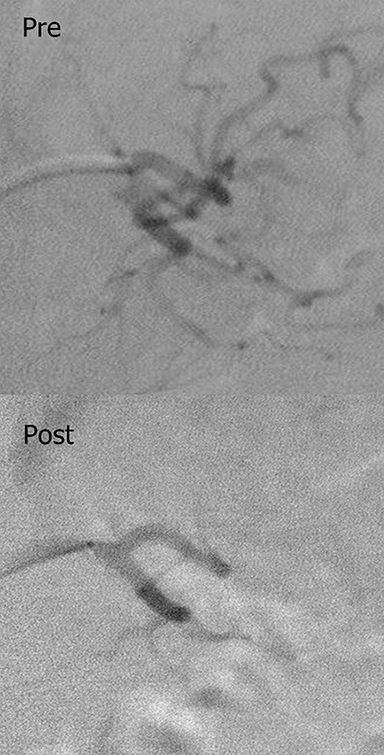
The first bariatric embolization in the western hemisphere was performed in 2014 by Mubin Syed, MD. A total of 4 embolizations using 300- to 500-micron Beadblock (BTG group) have since been performed in the GET LEAN study (Gastric Artery Embolization Trial for the Lessening of Appetite Nonsurgically). Average weight loss at 3 months was 7% with an excess body weight (EBW) loss of 14%. Average weight loss at 6 months was 8.5% with an EBW loss of 17.2%. The one-year result for the first patient was 48 lbs of weight loss, representing 49% of EBW for this patient and a loss that is equivalent to bariatric surgery. There was only mild weight loss of 6 and 9 lbs in the 2nd and 3rd patients, respectively at 6 months, due to prior history of depression requiring antidepressant therapy. The 4th patient lost 26 lbs in 3 months, or 17% of excess body weight. She also was the first diabetic patient to undergo the procedure and had near normalization of her Hgb A1C levels at 3 months. This series also included the first radial artery approach for the procedure, which has safety implications in the morbidly obese who may have “hostile groins.”7
Led by Clifford Weiss, MD, Johns Hopkins University has performed the procedure in 5 patients with an average weight loss of 6.7% and an EBW loss of 7.9% at 3 months (BEAT OBESITY study) using 300- to 500-micron Embospheres (Merit Medical). They also reported a 29% decrease in ghrelin levels at 3 months.8
No human trial so far has reported any major adverse events. Minor adverse events have included superficial gastric ulcerations in the GET LEAN study that have all healed by 30 days. In BEAT OBESITY, 2 patients had minor adverse events, including 1 with transient pancreatitis and 1 with a superficial gastric ulceration that healed by 90 days. Human trials in the United States are part of FDA-supervised IDE studies. All studies require a CT angiogram, a baseline endoscopy and a gastric-emptying study. Once normal studies are obtained, the procedure is performed using standard left gastric artery catheterization techniques with microcatheter sub-selection for the actual embolization. Close follow-up exams are then performed for at least 1 year.
Future directions include the study of larger patient groups, as well as a randomized controlled trial. The optimal technique in terms of particle size will, hopefully, also be determined by further study. In conclusion, bariatric embolization shows great promise as a potential weapon against obesity.
References
- Arepally A, Barnett BP, Patel TH, Howland V, Boston RC, Kraitchman DL, Malayeri AA. Catheter-directed gastric artery chemical embolization suppresses systemic ghrelin levels in porcine model. Radiology. 2008 Oct;249(1):127-33.
- Arepally A, Barnett BP, Montgomery E, Patel TH. Catheter-directed gastric artery chemical embolization for modulation of systemic ghrelin levels in a porcine model: initial experience. Radiology. 2007;244:138-143.
- Paxton BE, Kim CY, Alley CL, Crow JH, Balmadrid B, Keith CG, Kankotia RJ, Stinnett S, Arepally A. Bariatric embolization for suppression of the hunger hormone ghrelin in a porcine model. Radiology. 2013 Feb;266(2):471-9
- Oklu, R, Gunn, AJ, Hamilton, EJ. A catheter to curb your appetite? A novel observation of weight loss following left gastric artery embolization in humans. Radiological Society of North America Annual Meeting 2013; Dec 1, Session SSA23, Code: SSA23-01.
- Kipshidze, N, Archvadze, A, Kantaria, M, Konstantine, M, First In-Man study of left gastric artery embolization for weight loss. American College of Cardiology Annual Meeting, 2013, Mar 10, Presentation Number: 1209M-159.
- Kipshidze, N, Archvadze, A, Kantaria, M, Konstantine, M. Endovascular bariatric embolization: 2 Year follow-up from first in-Man study. American College of Cardiology Annual Meeting, 2015; Mar 15, Presentation Number: 908-06.
- Syed, MI, et al. Bariatric embolization for morbid obesity, first western hemisphere experience: Gastric artery embolization trial for lessening appetite nonsurgically (GET LEAN). Radiological Society of North America Annual Meeting 2015, De. 1, Session RC314.
- Weiss, CR, Paudel, K, Cheskin, LJ, Holly, KH, Fischman, A, Patel, R, Shin, EJ, Steele, K, Moran, DL, Kraitchman, Arepally, A. Bariatric embolization of arteries for the treatment of obesity (BEAT Obesity): Early clinical results. Cardiovascular and Interventional Radiological Society of Europe Annual Meeting, 2015. Session 1406.2.
Citation
MI S, K M, A S. Bariatric embolization: Does it carry any weight?. Appl Radiol. 2016;(3):30-32.
March 2, 2016