Breast Cancer Metastasis to the Endometrium
Images


CASE SUMMARY
A 47-year-old G2P2002 presented to the oncologist with a history of Stage IIIB estrogen receptor (ER), progesterone receptor (PR), and human epidermal receptor 2 (HER2) positive ductal carcinoma managed with right mastectomy, radiation therapy, chemotherapy, and tamoxifen. The patient had had a 7-year disease-free interval, but on presentation, recurrences were found in her bones, brain, and lymph nodes. Shortly after disease recurrence, she experienced new-onset vaginal bleeding. The patient underwent positron emission tomography-computed tomography (PET-CT) and subsequently underwent total abdominal hysterectomy with bilateral salpingo-oophorectomy and lymph node dissection.
IMAGING FINDINGS
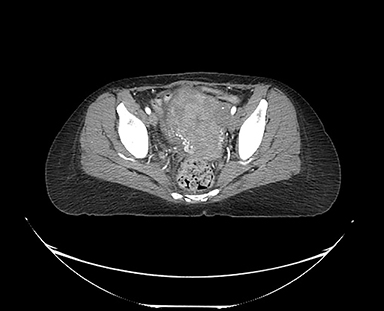
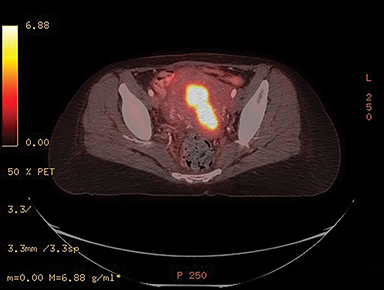
PET-CT demonstrates a lobular appearance of the uterus with a thickened endometrium. There was increased avidity in the uterus with a standard uptake value of 15.4, concerning for malignancy (Figure 1).
DIAGNOSIS
Breast cancer metastasis to the endometrium
DISCUSSION
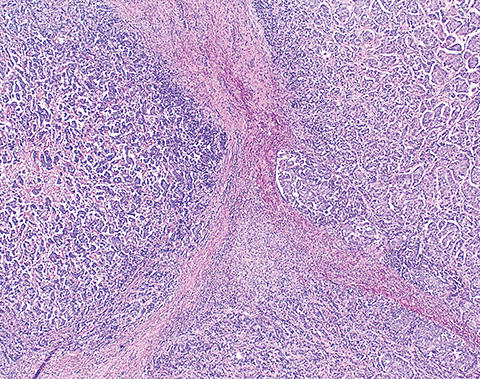
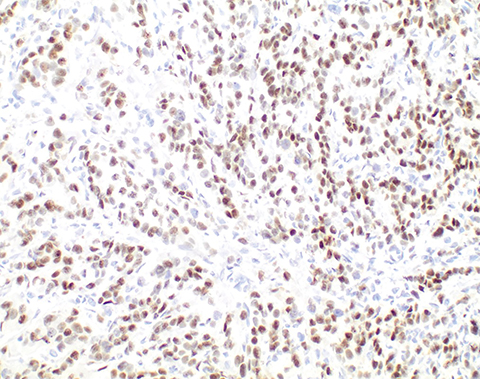
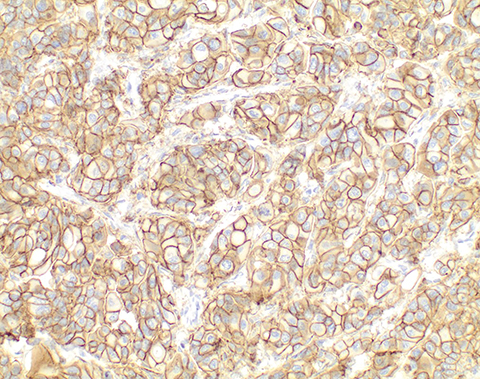
On gross examination, the endometrial cavity was filled by a tan-pink nodular mass measuring 6.1 × 3.8 × 2.2 cm (Figure 2). Microscopic examination demonstrated a poorly differentiated metastatic carcinoma in the uterus consistent with breast primary, with involvement of the uterine endometrium, myometrium, lower uterine segment, cervical mucosa, and stroma (Figure 3). The lesional cells stained strongly positive for ER and HER2 immunohistochemistry (Figure 3). This immunoprofile was consistent with the prior lumpectomy specimen. Mammoglobin, an IHC stain useful for detecting metastatic breast cancer, was also positive (Figure 3).
Breast cancer most commonly metastasizes to the bone. The lungs, liver, and brain are also common sites of metastatic disease.1 The most common gynecologic site of metastatic breast cancer is the ovary, followed by the vagina.2 In contrast, the endometrium is a rare site for primary breast cancer metastasis. Few case reports describe metastatic disease to the uterus, which is most commonly discovered at autopsy.3 The most common presenting symptom, as in this case, is abnormal vaginal bleeding. Endometrial metastases from breast cancer are most frequently described in cases of invasive lobular carcinoma.3
Given the rarity of metastasis to the endometrium, primary endometrial cancer is an additional diagnostic consideration in a breast cancer patient with new onset vaginal bleeding. This is of particular concern in breast cancer patients with hormone receptor positive breast cancer managed with tamoxifen. The agonist effect of tamoxifen on the endometrium increases the risk of primary endometrial cancer two to three times the typical risk of postmenopausal women.4
The incidence of endometrial cancer among breast cancer patients treated with tamoxifen is 0.388%, which is presumably more common than metastatic disease to the uterus.5 Differentiating primary endometrial cancer from breast cancer metastatic to the endometrium has important clinical implications. Primary endometrial cancer may be curable with surgery, whereas metastatic disease to the uterus has only systemic treatment options with an overall poor prognosis.
CONCLUSION
We report a case of ductal carcinoma metastasizing to the uterus, presenting with abnormal vaginal bleeding. The endometrium is an unusual location for breast cancer metastasis, with more common involvement seen at other gynecologic sites. Breast cancer metastasis to the endometrium, while rare, must be distinguished from primary endometrial cancer due to significant clinical implications of the diagnosis.
REFERENCES
- Lee YT. Breast carcinoma: pattern of metastasis at autopsy. J Surg Oncol. 1983 Jul;23(3):175-80. doi 10.1002/jso.2930230311
- Mazur MT, Hsueh S, Gersell DJ. Metastases to the female genital tract: Analysis of 325 cases. Cancer. 1984 May 1;53(9):1978-84. Doi: 10.1002/1097-0142(19840501)53:9<1978::aid-cncr2820530929>3.0.co;2-1
- Hara F, Kiyoto S, Takabatake D, et al. Endometrial Metastasis from Breast Cancer during Adjuvant Endocrine Therapy. Case Reports in Oncology. 2010;3(2):137-141. doi 10.1159/000313921
- Lhommé C, Pautier P, Zagamé L, et al. Endometrial surveillance of women on Tamoxifen. Gynecol Obstet Fertil. 2003 Jul-Aug;31(7-8):647-56. doi 0.1016/s1297-9589(03)00195-4
- Chen JY, Kuo SJ, Liaw YP, et al. Endometrial cancer incidence in breast cancer patients correlating with age and duration of tamoxifen use: a population based study. J Can. 2014;5(2):151–155. doi 10.7150/jca.8412.
Citation
A F, D R, V S, K N. Breast Cancer Metastasis to the Endometrium. Appl Radiol. 2020;(6):52-53.
November 6, 2020