Cross-sectional imaging essential to detecting midfoot fractures
Images
X-rays are insufficient for comprehensive detection of Chopart joint fractures and other fractures of the midfoot, according to a study from Massachusetts General Hospital (MGH) published in the October issue of Emergency Radiology. While radiographs are the initial exam, Chopart fractures were missed in one-third of the cases, and additional ankle and midfoot fractures were identified on computed tomography (CT) or magnetic resonance imaging (MRI) in more than half of the cases.

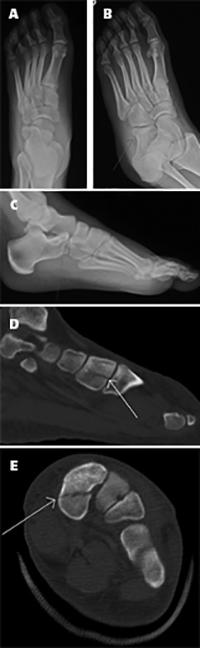
A 17-year-old male presented after a
motor vehicle accident, complaining of
left foot pain. Antero-posterior (A),
oblique (B) and lateral (C) radiographs
of the left foot show an anterior
calcaneus fracture extending to the
calcaneocuboid joint, a Chopart fracture
(arrows in B and C). Sagittal (D) and
axial (E) CT images of the left
foot show a non-displaced
additional fracture in the first
cuneiform (arrows in D and E) with
intraarticular extension (arrow in D).
The lack of sensitivity of X-ray images to identify fractures of the foot compared to CT or MRI has been well documented in published studies. However, the American College of Radiology (ACR) guidelines for midfoot fractures recommend that cross-sectional imaging be performed only if physicians suspect a fracture even though radiographs are normal. Lead author Renata R. Almeida, MD, and her colleagues at the MGH emergency department believe that a CT or MRI is essential as a part of the imaging workup of these injuries. They conducted a retrospective study of all patients diagnosed with a Chopart joint fracture over a four-year period to validate this, and also to assess the sensitivity of radiographs to detected additional fractures.
The patient cohort included 108 patients who had both X-ray and CT or MRI exams. More than half experienced high-energy traumas. The most common Chopart fracture was the calcaneocuboid joint (75% of the cases), followed by the talonavicular joint (21%). Five percent of patients had fractures in both joints. Thirty-four percent of patients who had Chopart fractures also additional fractures of the midfoot and ankle. They occurred more in patients who had experienced high-energy trauma, commonly involving fractures of the distal fibula, distal tibia, navicular, and talus.
The radiologists reported that Chopart fractures were not identified in 35 patients (32%) by radiograph. Additionally, at least one fracture was not diagnosed in 57% of cases with multiple fractures. They wrote that diagnostic sensitivity of non-weight-bearing radiographs for detecting Chopart fractures was 69% and 42% for additional fractures. CT and MR were used as the gold standard. The sensitivity of radiographs to detect additional fractures was lower in cases of low-energy trauma compared to high energy trauma, highlighting the role of cross-sectional imaging in both settings.
Although exposure to radiation dose is higher with a CT exam, the authors believe that it is merited, considering that low-radiation dose protocols have become available. “Delayed or misdiagnosis of additional midfoot fractures are associated with higher morbidity rates,” they wrote. “Without treatment, midfoot osseous fractures often lead to painful malunion or nonunion, and irreversible cartilage damage, resulting in posttraumatic arthritis, chronic pain, and deformity.”
REFERENCE
- Almeida RR, Mansouri M, Tso DK, et al. The added value of cross-sectional imaging in the detection of additional radiographically occult fractures in the setting of a Chopart fracture. Emer Radiol. 2018;25(5):513-520.