Ferromagnetic detection systems: a safety net after MRI patient pre-screening
The highest safety standards of operating a MRI imaging suite can potentially be compromised if a patient has an implant which he or she may not know about and for which medical records are not available. Or, if a patient fails to disclose metal body piercing jewelry and/or it is concealed in an intimate location. Or if, as in a recent near miss at a Fort Myers, FL imaging center, a radiologic technologist violates protocol and tells a patient that it is not necessary not to remove her shoes, which happened to contain numerous metal nails.
 Ferromagnetic detection systems can provide an additional safeguard. But how well do they work? Laura Orchard, the superintendent manager of MRI at Princess Elizabeth Hospital in St. Martins, Guernsey, United Kingdom, decided to assess the effectiveness of a system that had recently been installed in the patient changing room.
Ferromagnetic detection systems can provide an additional safeguard. But how well do they work? Laura Orchard, the superintendent manager of MRI at Princess Elizabeth Hospital in St. Martins, Guernsey, United Kingdom, decided to assess the effectiveness of a system that had recently been installed in the patient changing room.
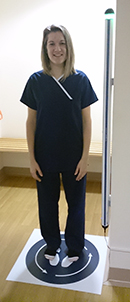
The system (Ferroguard® Screener, Metrasens, Malvern, Worcestershire, UK) worked by pushing a button, after which a patient slowly rotates in a complete circle while standing on a fixed floor mat.The system is not affected by the static magnetic field, as it is designed to detect moving ferromagnetic objects only. The sensitivity of the system had been adjusted at the time of installation to allow for the local environment so that extraneous magnetic field interference was minimized. If a light on the sensor turned yellow or red, further questioning and investigation was performed.
A total of 1,000 consecutive patients were recruited, with 23 dismissed due to the inability to rotate in a circle unaided. Alerts were triggered for 76 patients. Eighteen patients were identified as having removable objects on them and 16 patients had non-removable objects or implants. There were a total of 21 false positives, or 2% of the total. The time to assess “green light” patients was less than one minute. The time to question and rescreen patients who triggered an alert took five to 10 additional minutes. If a question remained, a radiologist was consulted.
The causes for generating accurate alerts included:
- Pre-disclosed implants, including coronary stents and sternal wires, pacemakers, orthopedic and other surgical implants.
- Failure of patients to remove metal objects on their bodies.
- Items such as keys and safety pins in pockets of clothing (including hospital issued gowns or robes).
Sensitivity was 100% and specificity was 98%.
This study published online in Radiography was limited to evaluation of a single ferromagnetic detection system. It supports an earlier study conducted in 2013 by Dr. Frank G. Shellock of the University of California Keck School of Medicine and the Institute for MRI Safety, Education and Research in Los Angeles of the same manufacturer’s system. Dr. Shellock and colleagues’ study evaluated 67 implants and other objects, including items made from materials that had relatively low magnetic susceptibility, by attaching the items to a volunteer who then rotated in a circle. The system’s sensitivity was 92% and its specificity was 100%.
Orchard told Applied Radiology that the system has added another level of safety to prevent harm to a patient, and is an excellent supplement to the existing prescreening protocols. “it gives us an additional level of confidence that we have done everything possible to protect a patient,” she said.
REFERENCES
- Orchard LJ. Implementation of a ferromagnetic detection system in a clinical MRI setting. Radiography Published online January 3, 2015.
- Shellock FG. Detection of implants and other objects using a ferromagnetic detection system: Implications for patient screening before MRI. 2013 AJR 201:4;720-725.
Citation
. Ferromagnetic detection systems: a safety net after MRI patient pre-screening. Appl Radiol.
March 19, 2015