Imaging body composition may benefit treatment of cancer patients
The use of CT and MRI examinations for tumor staging of cancer patients, surveillance, and response assessment provides an excellent opportunity for radiologists to integrate body composition assessment into patient care. Body composition assessment can also identify risk factors that may have a negative impact on the treatment and overall health of a patient such as obesity, sarcopenia, and sacropenic obesity.
Imaging quantification of body composition such as lean muscle mass and fat distribution is potentially a valuable tool for clinicians treating cancer patients, according to Professor Vicky Goh, M.D., chair in clinical cancer imaging of the Division of Imaging Sciences and Biomedical Imaging at Kings College London, and a co-author of an article on the subject published online June 13, 2015 in Insights into Imaging. This could be most beneficial in high risk patients with gastrointestinal cancers or pre-existing gastrointestinal disease. Additionally, an objective assessment of body composition using cross-section imaging techniques has the potential to complement both clinical and nutritional evaluation of patients’ fitness and treatment tolerability.
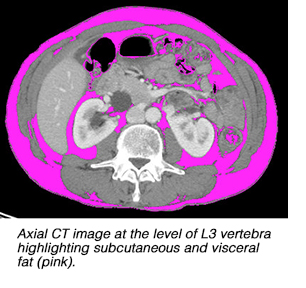 Body mass index (BMI) is most commonly used to define obesity. Visceral obesity refers to the excessive accumulation of visceral fat in the abdominal cavity. Visceral obesity is associated with adverse outcomes in cancer patients, attributed in part to increased insulin resistance and its levels of endocrine hormonal secretion. The latter has been associated with cancer progression.
Body mass index (BMI) is most commonly used to define obesity. Visceral obesity refers to the excessive accumulation of visceral fat in the abdominal cavity. Visceral obesity is associated with adverse outcomes in cancer patients, attributed in part to increased insulin resistance and its levels of endocrine hormonal secretion. The latter has been associated with cancer progression.
Body composition may affect an individual’s tolerance to chemotherapy and may be predictive of treatment toxicity. The risk of toxicity is higher in women, as they tend to have a lower lean body mass in comparison to their body surface area. A lean body mass of both men and women may be a better measure to determine the dose of chemotherapy drugs on an individual patient basis.
Scarcopenia is defined as appendicular skeletal muscle mass less than two standard deviations below the mean of a young healthy adult group as determined by dual-energy X-ray absorptiometry (DEXA), although the condition should ideally be diagnosed based on the presence of impaired muscular function and low muscle mass. The condition may be age-related or associated with reduced activity, malnutrition, endocrine disease, neurodegenerative disorders, or cancer cachexia (a complex metabolic syndrome in chronically ill patients associated with loss of muscle mass, with or without loss of fatty tissue). Physicians should be aware that sarcopenia may be present even in the absence of weight loss.
The authors report that sarcopenic cancer patients have higher rates of both morbidity and mortality. Clinical studies have shown that sarcopenic cancer patients who undergo primary colorectal surgery may have twice as high a risk of post-operative infection and may have an increased length of inpatient hospital stay.
When scaropenia and obesity are combined, the resulting condition is sarcopenic obesity. This condition is a significant negative prognostic factor in patients with gastrointestinal and respiratory tract cancer. Patients with sarcopenic obesity tend to have poorer functional status and a worse overall survival outcome.
CT and MRI scans can provide estimates of lean muscle mass adipose tissue and fat infiltration within the skeletal muscles. CT has been shown to be superior to DEXA, and lean body mass, subcutaneous, and visceral mass can be delineated for a given volume on CT images. The major advantage of MRI over CT in body composition analysis is that no ionizing radiation is used. In addition, MRI has better soft tissue definition compared to CT, which may improve image segmentation of adipose tissues and skeletal muscle.
The authors discuss specific techniques in their article, which may be accessed free of charge here.
REFERENCE
- Yip C, Dinkel C, Mahajan A et al. Imaging body composition in cancer patients: visceral obesity, sarcopenia and sarcopenic obesity may impact on clinical outcome. Insights Imaging. Published online June 13, 2015.