Intrapulmonary bronchogenic cyst
Images

CASE SUMMARY
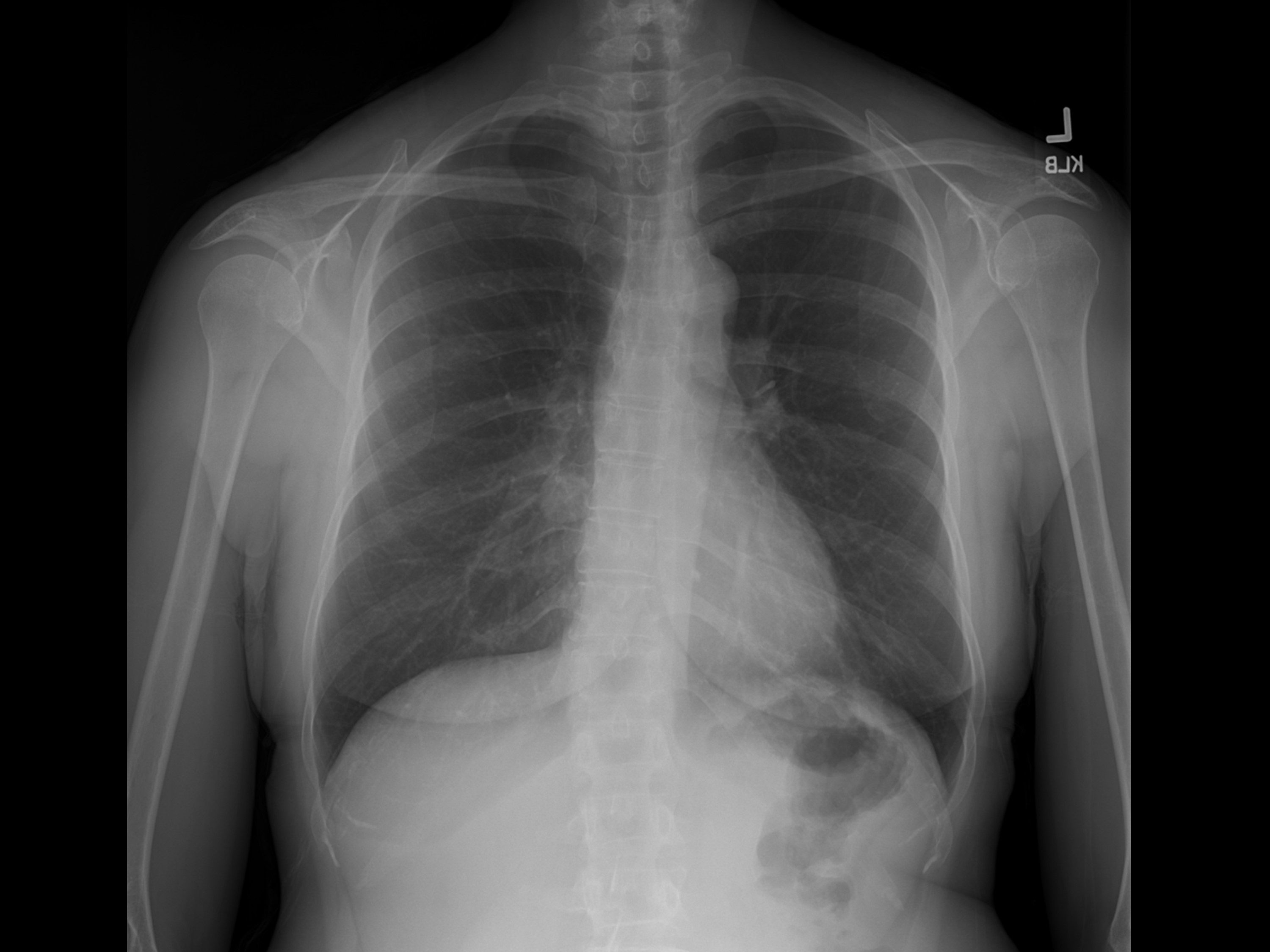
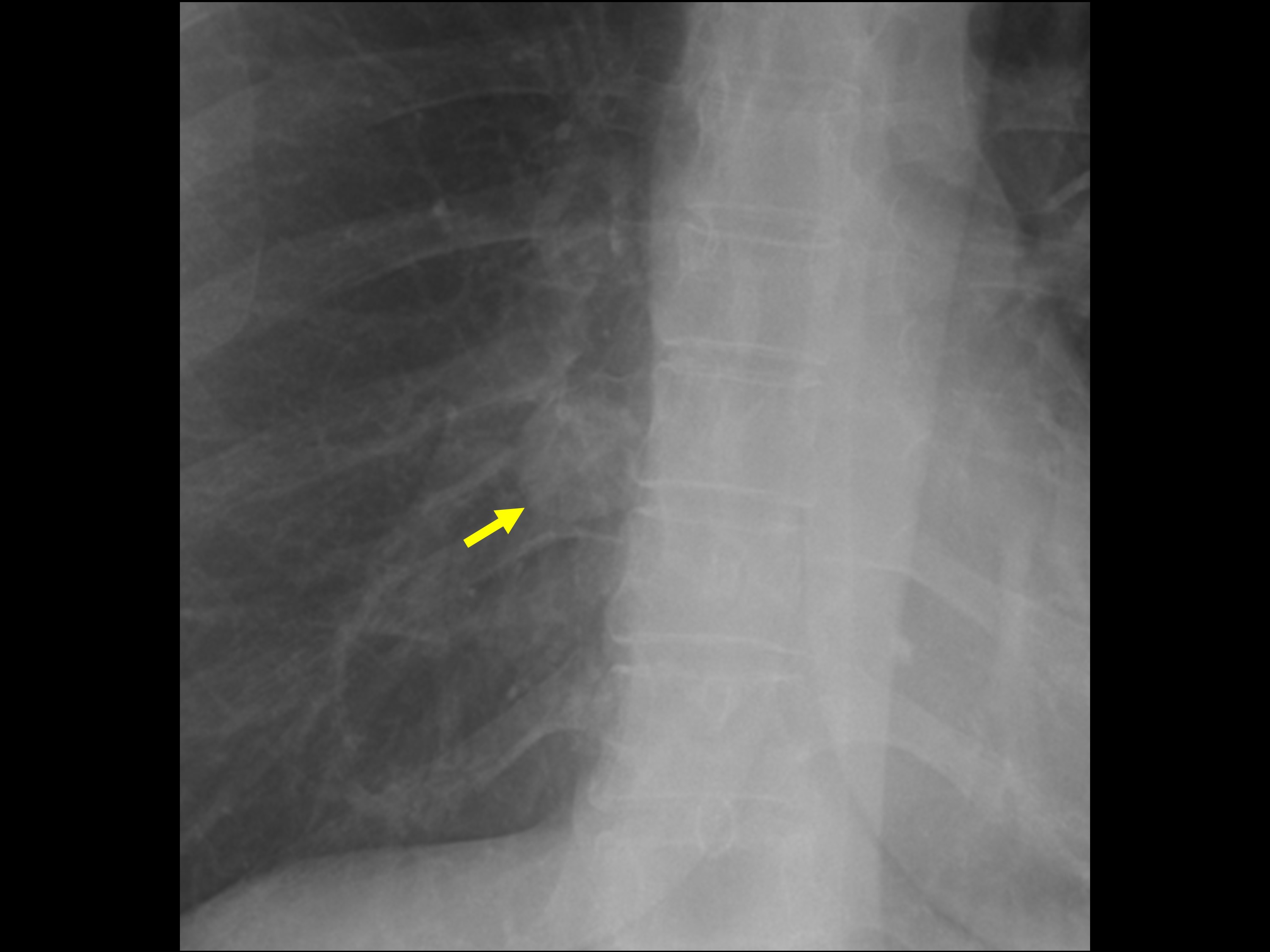
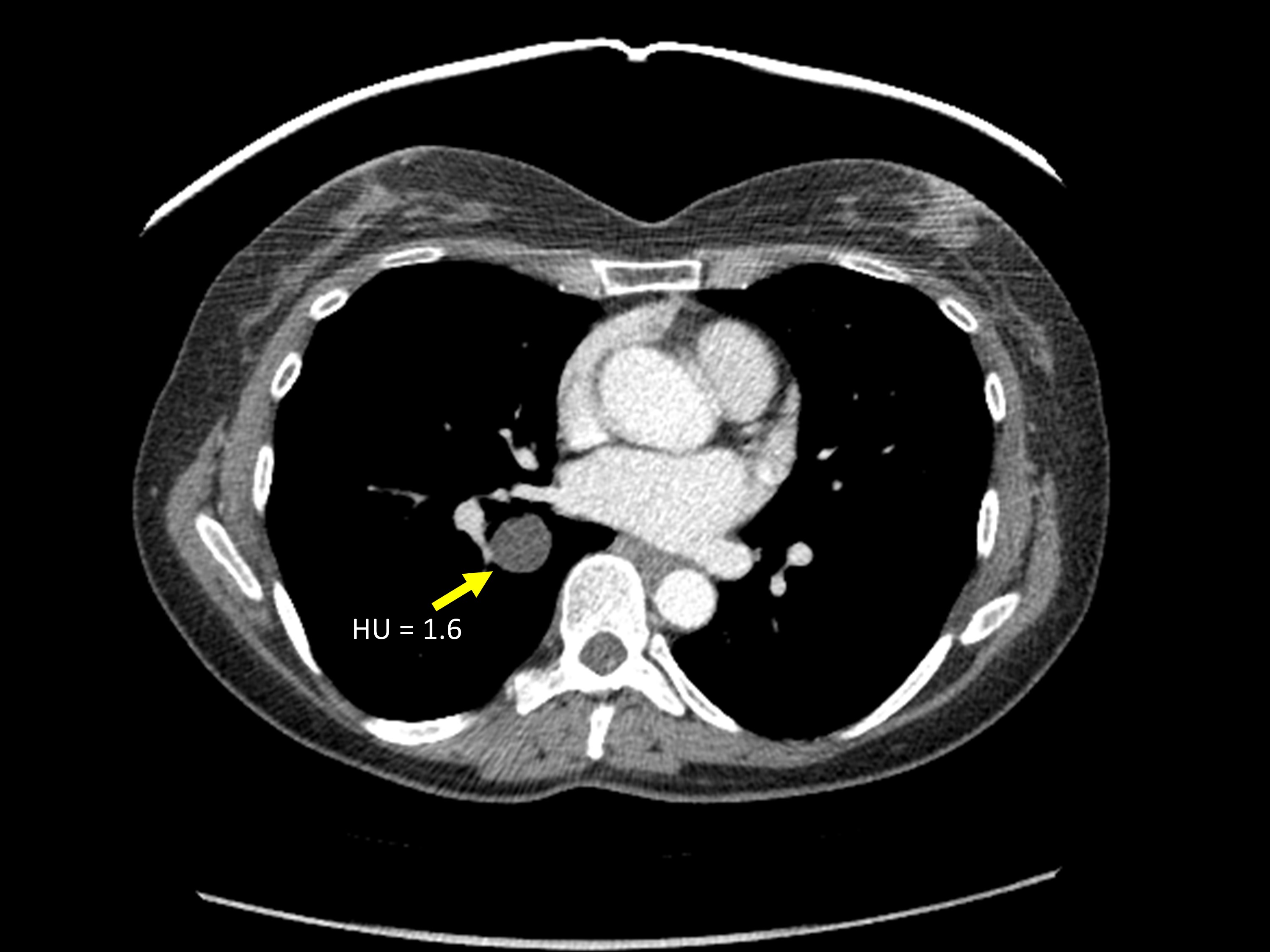
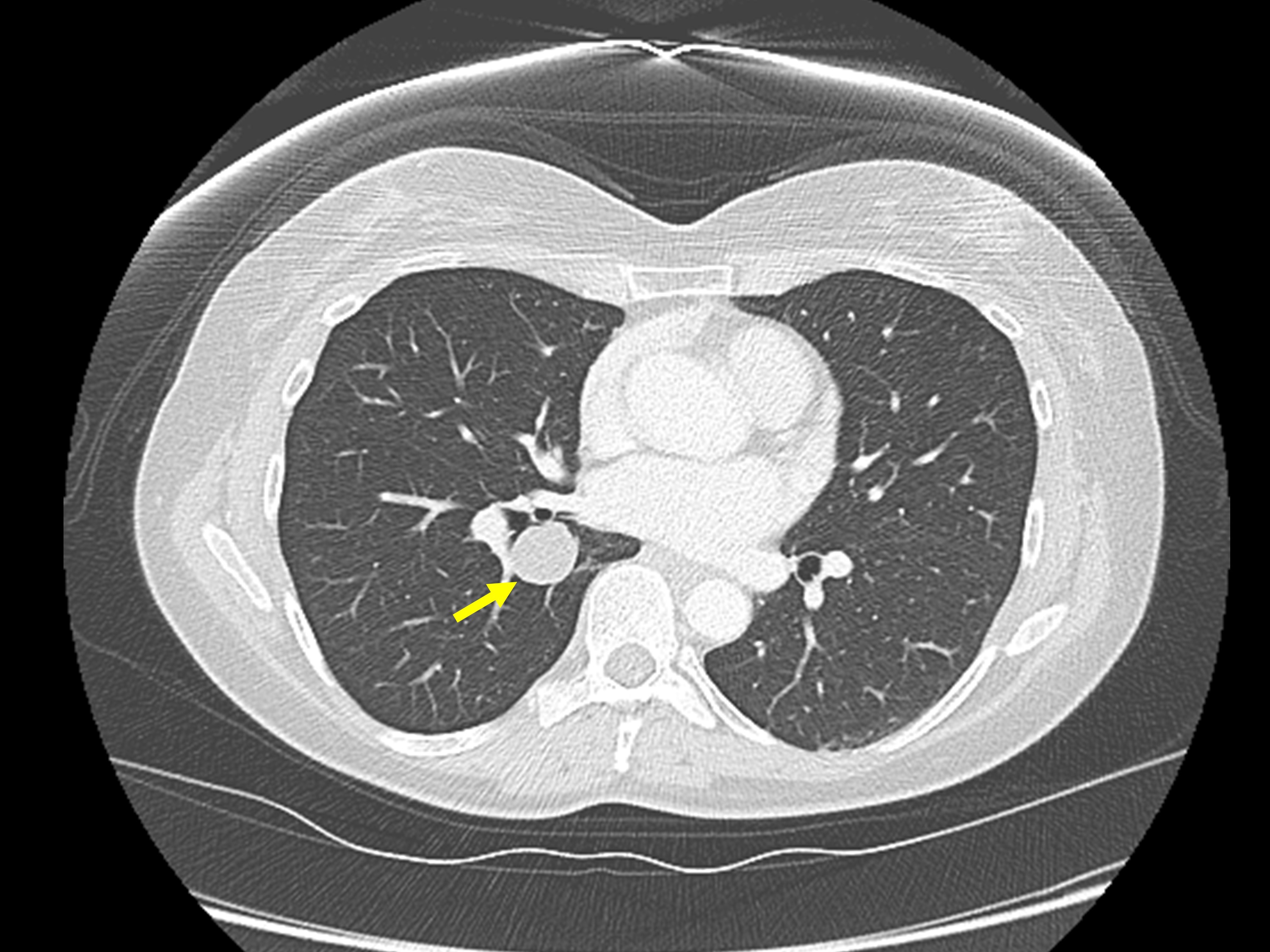
A 52-year-old female presented to the emergency department with left-sided chest pain. The patient was afebrile and had a normal white blood cell count. A chest radiograph was obtained for evaluation of the chest pain (Figure 1). Based on the chest radiograph findings, a contrast-enhanced chest CT was also obtained (Figure 2).
IMAGING FINDINGS
The chest radiograph demonstrated a well-circumscribed nodule in the medial right lower lobe (Figure 1). Subsequent contrastenhanced CT demonstrated a homogeneous, nonenhancing, thin-walled cyst in the right lower lobe (Figure 2). Hounsfield units measured 1.6. This cyst correlates with the nodule identified on radiography.
DIAGNOSIS
Intrapulmonary bronchogenic cyst
DISCUSSION
During embryologic development, a ventral foregut diverticulum gives rise to the respiratory system. Abnormal budding of the resultant bronchial tree results in a bronchogenic cyst. Bronchogenic cysts that form early in respiratory system development localize to the mediastinum, whereas bronchogenic cysts that form later in respiratory system development localize to the lung parenchyma (ie, intraparenchymal bronchogenic cyst).1 Histologically, bronchogenic cysts consist of ciliated columnar epithelium cells surrounded by bronchial cartilage, smooth muscle, connective tissue, and bronchial glands.2 The majority of bronchogenic cysts localize to the mediastinum, 15-25% localize to the lung parenchyma, and a small number of bronchogenic cysts localize to the diaphragm or pleura.1,3 In general, most bronchogenic cysts are asymptomatic. When symptomatic, clinical presentations include chest pain, dyspnea, wheezing, and cough.3
On chest radiographs, intrapulmonary bronchogenic cysts are smoothly marginated, round or oval masses.4 CT typically shows a homogeneous, non-enhancing, oval or round lung mass with thin walls, and a lower lobe predominance.4 CT attenuation values may clearly confirm that these lesions are cysts, as in our case. However, if the cyst fluid is hemorrhagic, proteinaceous, or contains calcium, the attenuation values may be higher than expected for simple fluid. In some cases, intraparenchymal bronchogenic cysts may communicate with the bronchial tree, resulting in air-filled cysts or an air-fluid level.4 Differential diagnosis of an intrapulmonary bronchogenic cyst includes a pulmonary lymphangioma, though these are extremely rare. If the cyst contains air, abscess or infected bulla should be included in the differential. If abutting the mediastinum, other medistinal congenital cysts, pericardial cysts, or cysts from spinal origin could be considered. Furthermore, when the cyst fluid is hyperdense, distinction between an intraparenchymal bronchogenic cyst and a solid lung nodule may be challenging. Bronchogenic cysts typically do not enhance, which helps to distinguish them from solid nodules on contrast-enhanced cross-sectional imaging.4 On MRI, a hyperdense bronchogenic cyst should follow proteinaceous fluid signal (i.e., high signal on both T1 and T2-weighted sequences).3,4
Treatment of bronchogenic cysts is somewhat controversial. Some advocate surgical excision due to the risk of infection and a small (0.7 percent) risk of malignant degeneration.5 An alternative option is close imaging surveillance to ensure temporal stability.5
CONCLUSION
Bronchogenic cysts may occasionally arise within the lung parenchyma rather than the more common mediastinal location. On imaging, these intraparenchymal bronchogenic cysts are typically well circumscribed oval or round masses. When the attenuation is clearly fluid, the diagnosis of a bronchogenic cyst is fairly straightforward. However, when the fluid is dense (hemorrhagic/proteinaceous), distinction of a cyst versus a solid lung nodule may prove challenging. Treatment is controversial and ranges from surgical excision to imaging surveillance.
REFERENCES
- Shields TW, LoCicero J, Reed CE, Feins RH. General Thoracic Surgery. Lippincott Williams & Wilkins. 2011.
- Aktogu, S, Yuncu G, Halilcolar H, Ermete S, Buduneli T. Bronchogenic cysts: clinicopathologic presentation and treatment. Eur Respir J. 1996; 9: 2017-2021.
- McAdams HP, Kirejczyk WM, Rosado-de-Christenson ML, et al. Bronchogenic cyst: Imaging features with clinical and histopathologic correlation. Radiology. 2000;217:441-446.
- Yoon YC, Lee KS, Kim TS, et al. Intrapulmonary bronchogenic cyst: CT and pathologic findings in five adult patients. Am J Roentgenol. 2002;179:167-170.
- Kirmani B, Kirmani B, Sogliani F. Should asymptomatic bronchogenic cysts in adults be treated conservatively or with surgery? Interact Cardiovasc Thorac Surg. 2010;11:649-659.
Citation
VA L. Intrapulmonary bronchogenic cyst. Appl Radiol. 2016;(1):38-39.
January 7, 2016