Lipomyelocele in newborn
Images


CASE SUMMARY
Patient is a 1-day-old male who was found to have a small cutaneous hemangioma overlying the lumbosacral region. Birth history and physical examination are otherwise unremarkable.
IMAGING FINDINGS
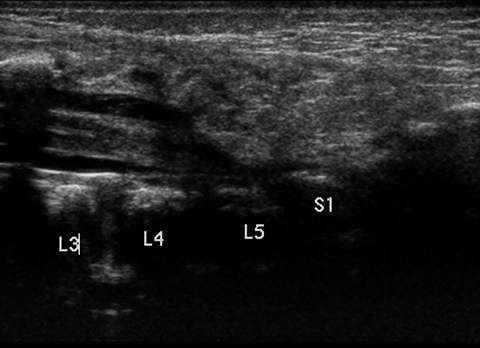
Ultrasound images demonstrate a tethered spinal cord, extending to the L5-S1 level. There is also a subcutaneous echogenic mass, which has an intrathecal component that appears contiguous with the cord (Figure 1).
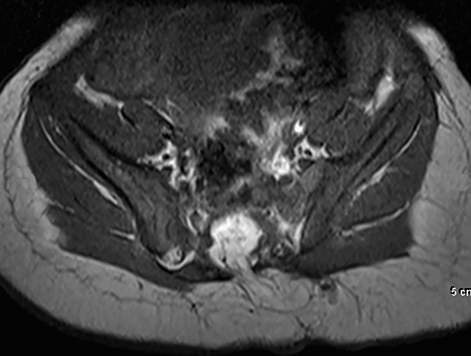
Noncontrast lumbar spine MRI shows a focal fatty mass (high T1, T2 signal) in the sacrococcygeal region with an intrathecal component. This mass causes tethering of the spinal cord. The fatty mass extends through a defect in the posterior elements of the sacrum and is contiguous with the subcutaneous fatty tissues (Figures 2, 3 and 4).
DIAGNOSIS
Lipomyelocele
DISCUSSION
Occult spinal dysraphisms (skin- covered lesions with no exposed neural tissue) include lipomyelocele, lipomyelomeningocele, dorsal dermal sinus, and diastematomyelia, and are the most common indication for spinal imaging in children.1 Spinal dysraphism prevalence has been estimated at 3.1 cases per 10,000 people between ages 0-19.2
Lipomyelocele and lipomyelomenigocele both involve lipomas with a dural defect, and are differentiated by the extension of the neural placode-lipoma interface outside of the spinal canal with the latter. Both of these abnormalities result from a defect during primary neurulation, with mesenchymal tissue entering the neural tube and forming lipomatous tissue.3,4
Occult dysraphisms demonstrate a broad spectrum of clinical findings, including skin stigmata such as dimples, sinus tract, hair patch or hemangioma. Approximately 50-80% of occult spinal dysraphic cases exhibit a dermal lesion. Motor, bladder, or bowel dysfunction may also be present.1
Ultrasound will demonstrate a low-lying spinal cord tethered by a lipoma. The lipoma will be contiguous with subcutaneous tissues of the back and extend through a posterior bone defect to insert on the cord. Sonographic findings that suggest a tethered cord include low positioning of the conus (normally ends between T12 and L2-3) and decreased/absent “to-and-fro” motion of the cord during real-time imaging.
MR will confirm the presence of a lipoma (high signal on T1, T2), which is contiguous with the subcutaneous tissues, extending through a posterior spinal canal defect and causing cord tethering. Insertion of the lipoma on the cord tends to be asymmetric; if a meningocele is present, it tends to extend to the side opposite of the lipoma insertion.5
Lipomyelocele and other occult spinal dysraphic disorders may result in issues including upper urinary tract deterioration, infection, and permanent neurological damage. Spinal neuroimaging thus has a critical role in allowing early detection and prompt neurosurgical intervention.1
CONCLUSION
Occult spinal dysraphic disorders such as lipomyelocele are an uncommon but clinically important diagnosis in the pediatric patient population due to the high risk of significant neurologic impairment. These disorders are often initially detected on ultrasound after the discovery of lumbosacral skin stigmata on physical examination. MRI is useful for confirmation and further characterization of ultrasound findings.
REFERENCES
- Medina LS, Crone K, Kuntz KM. Newborns with suspected occult spinal dysraphism: A cost-effectiveness analysis of diagnostic strategies. Pediatrics. 2001;108(6):e101.
- Shin M, Besser LM, Siffel C, et al. Prevalence of Spina Bifida among children and adolescents in 10 regions in the United States. Pediatrics. July 2010;126:274-279.
- Rufener SL, Ibrahim M, Raybaud CA, Parmar HA. Congenital spine and spinal cord malformations - Pictorial review. AJR. March 2010;194:26-37.
- Muthukumar N. Congenital spinal lipomatous malformations. Acta Neurochirurgica. 2009(151):179-188.
- Korsvik HS, Keller MS. Sonography of occult dysraphism in neonates and infants with MR imaging correlation. RadioGraphics. 1992(12):297-306.
Citation
AM V, JE S, G H, MA W. Lipomyelocele in newborn. Appl Radiol. 2016;(11):53-54.
November 2, 2016