Multiple cerebral hydatid cysts
Images
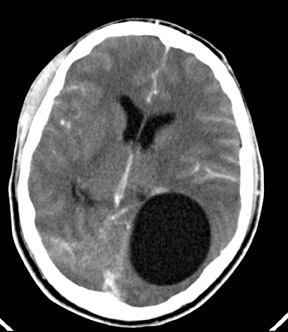
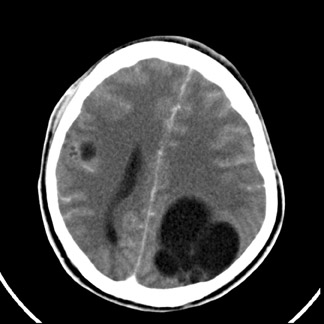

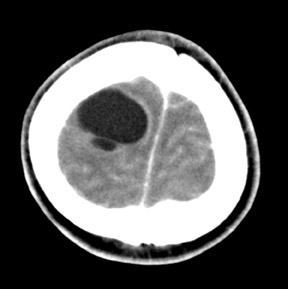
Multiple cerebral hydatid cysts
Findings
Contrast enhanced CT (Figures 1 to 4) showed multiple well-defined bilateral, rounded, cystic lesions in the supratentorial neuroparenchyma. One of the lesions showed daughter cysts (Figure 2). There was no perilesional edema. On injection of contrast, the lesions did not show significant enhancement. In addition to these lesions, there was cerebral edema. With these findings, a diagnosis of multiple cerebral hydatid cysts was suggested. Abdominal sonography did not reveal any cysts in other organs. The patient did not improve with conservative management and surgery was performed. The accessible cystic masses were removed and were confirmed to be hydatid cysts upon histologic examination. The patient improved with added drug treatment.
Discussion
Human echinococcosis, also known as hydatid disease is caused by Echinococcus granulosus. The larval stage is known as the hydatidcyst (HC). The disorder is caused by ingestion of dog feces that contain tapeworm ova. Intermediate hosts infected by larval hydatid cysts are usually sheep and cattle. Ingested ova hatch in the GI tract and liberated embryos can spread to organs via the portal or systemic circulation and develop into cystic larvae.
Hydatid cysts (HC) occur most frequently in the liver (65%) and lung (20%). Skeletal involvement is less common; the skull and vertebrae are common sites. Cerebral hydatids are rare and are seen in 1% to 3% of cases.1 They account for 1% to 5% of all intracranial masses in endemic areas and 0.2% to 2% in general. The human brain can be involved primarily via the hematogenous route or by metastatic spread when a cystruptures in the heart or lung.1,2 The majority of HC in the brain are singular. About 50% to 75% of intracranial hydatid cysts are seen in children. This high incidence in children is probably related to patent ductus arteriosus. These lesions can occur anywhere within the brain, but the middle cerebral artery distribution is most frequently involved, especially the parietal lobe. Most cysts are supratentorial. Infratentorial HC is very rare. Less common sites are skull, cavernous sinus, eyeball, pons, extradural, cerebellum and ventricles. As many as 80% of cerebral HC are associated with hepatic HC, but lack of evidence of HC in other parts of the body does not exclude HC within the brain.2, 3
The imaging findings are characteristic. A single, thin-walled spherical cerebrospinal fluid (CSF) density cyst in the parietal area is typical. Multilocular or multiple lesions occur but are rare (as in our case). CT shows a well-defined round or oval cystic structure of CSF density. Rim enhancement is infrequent, but intravascular contrast material may minimally increase the attenuation value of cyst fluid. There is no surrounding edema, but there is considerable mass effect and hydrocephalus may be present.3,4 Multivesical cysts are infrequent. Calcification occurs in <1% of the brain hydatid cysts. Magnetic resonance imaging (MRI) is superior to CT for evaluation of cerebral HC. The MRI usually shows an intra-axial fluid-containing structure without edema or enhancement, unless the cyst has ruptured and leakage has occurred and induced an inflammatory reaction. A diagnostic feature of cerebral hydatid disease is low signal intensity of the cyst wall in T2- weighted images.2,3,4
Conclusion
Though rare, hydatid cyst is an important differential diagnosis of cystic, intracranial-space–occupying lesions and is potentially curable.
- Diren HB, Ozcanli H, Boluk M, Kilic C. Unilocular orbital, cerebral and intraventricular cyst: CT diagnosis. Neuroradiology. 1993;35:149–150.
- Chang KH, Cho SY, Hesselink JR et al. Parasitic diseases of the central nervous system. Neuroimaging Clin North Am. 1991;1:159–178.
- Beggs I. The radiology of hydatid disease.AJR Am J Roentgenol. 1985;145: 639–648.
- Sierra J, Oviedo J, Berthier M, Leiguarda R. Growth rate of secondary hydatid cysts of the brain. Case report. J Neurosurg. 1985; 62;781–782.