Pediatric interventional radiology: Intervening gently
Images
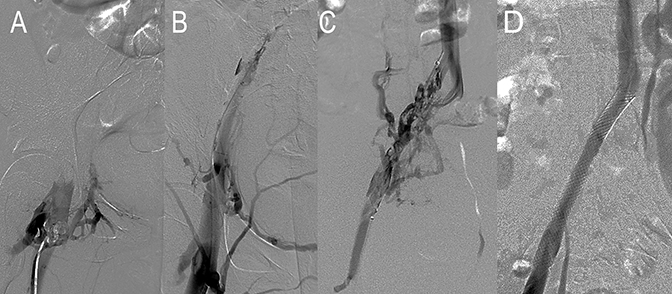
Interventional radiology (IR) is important to the delivery of safe, cost-effective pediatric care. Minimally invasive, image-guided vascular applications include venous access and interventions for congenital and acquired disease (Figure 1). Diagnostic catheter-directed angiography is used selectively in current algorithms, as ultrasound, magnetic resonance imaging and angiography, and computed tomographic angiography are now the principle noninvasive diagnostic vascular imaging modalities. Nonvascular pediatric IR procedures include enteric access (eg, feeding and percutaneous gastrostomy tube placements), biopsies, diagnostic and therapeutic drainages, percutaneous transhepatic cholangiography and biliary drainage, percutaneous cholecystostomy, and percutaneous nephrostomy.
Radiation exposure is a primary clinical risk in the performance of pediatric interventional procedures. This is directly related to the fact that radiation-dependent fluoroscopy and computed tomography (CT) are principal modalities for image guidance. Nonradiation-dependent ultrasound and MRI (in select centers) can also be utilized, depending upon the disease process, interventional window and supportive equipment and technology. Fluoroscopic guidance may be combined with ultrasound to improve technical guidance and potentially decrease radiation exposure. Hybrid CT-fluoroscopy and MRI-fluoroscopy technologies are also available and can be applied to minimize procedural time and radiation exposure.
When considering radiation risk, it is important to keep in mind that while organs have variable susceptibility and exposure during an IR procedure, radiation exposure is cumulative. Each time a pediatric patient undergoes a procedure with a radiation-dependent modality, the effective radiation dose is added to the total effective exposure. The total effective radiation dose is then measured against natural environmental background exposure. Natural radiation exposure averages approximately 2.5mSv per year.1
Mitigating radiation risk from medical imaging and restricting radiation exposure to not more than 2.5mSv per year requires adherence to the principles of ALARA—As Low As Reasonably Achievable. Paramount to achieving ALARA is limiting the use and volume of a radiation-dependent modality. For pediatric IR, this mandates primary consideration of a nonradiation modality (eg, ultrasound) or solution (eg, surgical procedure). The interventional team should always confirm appropriate clinical indications, a high pre-procedural probability for technical success, and moderate to high expected clinical impact. In accordance with these practice guidelines, repeat interventions with a radiation dependent modality should be performed only when the benefits of the procedure will outweigh the risks of additional effective radiation exposure. 2
General technical ALARA strategies to reduce exposure include: 1) weight-based protocols for radiation parameters (eg, kilovoltage, kV; milliamperage, mAs); and, 2) body and selective organ protective shielding.
Specific fluoroscopy radiation reduction strategies include: 1) using intermittent, pulsed X-ray beams of narrow width and low rates; 2) capturing images with “last image hold” and “fluoroscopic-save” options; 3) using X-ray beam and field of view filters; and, 4) selecting appropriate larger field of views.2
Radiation exposure during interventional procedures will depend upon procedure complexity, extent of disease, comorbid risk factors and the operator’s technique. While it is possible to perform a fluoroscopic or CT-guided procedure at the lowest possible kV and mAs, the penalty may be suboptimal quality. Suboptimal image guidance may also result from inadequate patient positioning, patient motion and overlying support devices. The consequences in these scenarios are longer procedure times and increased risk for iatrogenic injury. Furthermore, the longer procedure times, combined with the possible need to compensate with increased radiation parameters, may excessively increase exposure. At the extreme end of the spectrum, avoidance of radiation-dependent image-guidance and reliance solely upon ultrasound, MRI, or a surgical intervention could adversely impact resource utilization, patient safety, and clinical management.
Quality control measures are critically important to balancing the appropriate use of radiation modalities, adherence to ALARA, and dose optimization. Pathology-based interventional protocols with modality algorithms are primary control steps. Technical guidelines on radiation exposure parameters (eg, kV, mAs), patient positioning, and body shielding are the next level of control. These are specific to the patient and the procedure, in accordance with the modality, disease process, and region of intervention. Eliminating potential indirect sources of poor image quality is a third layer of control. Nonessential support devices should be excluded from the field of view. To control motion, conscious sedation protocols should be established in collaboration with pediatric anesthesiologists.
Continuous quality reviews are fundamental to ensuring appropriate modality utilization and compliance with control measures. They are necessary to ensure that radiation-dependent image-guided procedures are of appropriate and sufficient diagnostic quality. Reviews should assess determinants which may impact exam quality, including, but not limited to, radiation exposure settings, positioning, support devices, and motion. Three-hundred-sixty-degree input and feedback from the interventional team is essential to evaluating the quality of the pediatric interventional program, identifying areas for improvement, and implementing changes that will yield the highest success in pediatric clinical care and safety.
References
- International Commission on Radiological Protection (ICRP). Radiation and your patient: a guide for medical practitioners. A web module produced by Committee 3 of the ICRP. http://www.icrp.org/docs/Rad_for_GP_for_web.pdf
- Khong PL, Ringertz H, Donoghue V, Frush D, et al. ICRP publication 121: Radiological protection in paediatric diagnostic and interventional radiology. Ann ICRP. 2013; 42(2):1-13.