Primary hemangiopericytoma of the liver
Images
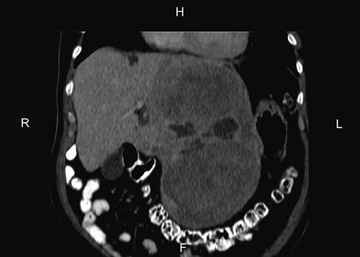
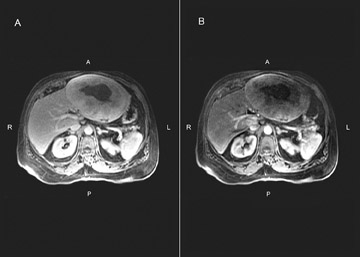
Primary hemangiopericytoma of the liver
Findings
Large heterogeneous lesions of the liver are rarely resectable for cure. However, the CT findings demonstrated no invasion of adjacent structures, no significant adenopathy and no evidence of malignancy. Additionally, the enhancement characteristics on MRI were not classic for hepatocellular carcinoma. Although the possibility of cure and the diagnosis were in doubt, the patient underwent diagnostic laparoscopy, laparotomy and left lateral segmentectomy (seg. 2 and 3). Pathology revealed a 21 cm hemangiopericytoma. Resection margins and lymph nodes were negative for tumor. The mass stained positive for CD99 and Bcl2, weakly positive for CD34 and smooth muscle actin, and negative for CD31 and EMA. This pattern is consistent with a hemangiopericytoma (solitary fibrous tumor.)
Discussion
Hemangiopericytoma, first described and named by Stout and Murray in 1942,1 is an uncommon spindle-cell tumor that pathologically displays a thin-walled vascular branching pattern. These tumors are derived from mesenchymal cells, can be benign or malignant, and occur more commonly in the lower extremities, but they have been described in the liver, pelvis and retroperitoneum. In an attempt to standardize nomenclature, some pathologists use the CD34, CD99, epithelial membrane antigen, GLC2, and smooth muscle actin stains to identify asubset of these tumors as solitary fibrous tumors.
Only 23 reported cases of primary liver hemangiopericytoma have been reported in the English literature.2 Both sexes in their sixth decade are affected equally. Clinical features include abdominal fullness and mass, weight loss, vomiting, diarrhea, fatigue and hypoglycemia.3 Information about the radiographic characteristics of hemangiopericytomas is scant. Fuksbrumer et al. described heterogenous enhancement on MRI and CT due to differential enhancement of the admixed cellular and collagenous components.4 Other anecdotal cases report areas of necrosis and calcification; these were not noted in our patient.
Conclusion
Although imaging features may suggest the diagnosis of a primary hemangiopericytoma of the liver, other benign or malignant hepatic tumors such as sarcoma, leiomyoma and inflammatory pseudotumor of the liver may have similar features.4 As resection of these tumors may result in long term survival, one should avoid the misdiagnosis and nihilism associated with hepatocellular carcinoma. Following primary excision, there is little role for radiation or chemotherapy.
- Stout AP, Murray MR. Hemangiopericytoma: A vascular tumor featuring Zimmermann’s pericytes. Ann Surg. 1942;116:26-33.
- Ji Y, Fan J, Xu Y, et al. Solitary fibrous tumor of the liver. Hepatobillary Pancreat Dis Int. 2006;5:151-153.
- Moran CA, Ishak KG, Goodman ZD. Solitary fibrous tumor of the liver; A clinicopathologic and immunohistochemical study of nine cases. Ann Diagn Pathol. 1998;2:19-24.
- Fuksbrumer MS, Klimstra D, Panicek DM. Solitary fibrous tumor of the liver: Imaging findings. AJR Am J Roentgenol. 2000;175:1683-1687.