Pseudoaneurysm in the renal arteries after blunt abdominal trauma
Images


Case Summary
A 22-year-old African American man with sickle cell disease was involved in a car accident and presented to the emergency department with right-sided abdominal pain. The initial workup showed multiple rib fractures, a liver laceration, and kidney lacerations. Initially he was treated conservatively and was hemodynamically stable and afebrile. On hospital day number 2, he developed fever and was treated with antibiotics. He improved and was discharged on hospital day 9 with a follow-up scheduled in 2 weeks. The patient presented to the emergency department complaining of worsening abdominal pain, and 2 episodes of emesis 4 days after discharge. No other symptoms were noted. Decreasing hematocrit and hemoglobin led to a second contrast CT scan of the abdomen and pelvis.
Imaging Findings
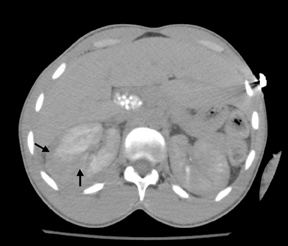
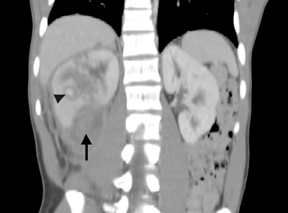
As a ligament injury was suspected to The CT scan at initial admission showed a large right perinephric hematoma with contusions and deep lacerations of the right mid-posterior kidney (Figure 1). On delayed images, no extravasations from the renal collecting system were noted. No hydronephrosis was seen. A small laceration of the liver was also noted adjacent to the right adrenal gland. Atrophy of the spleen was noted consistent with sickle cell disease. Gall stones were incidentally noted.
The CT scan on return showed again the right renal laceration with interval expansion of the perinephric hematoma and pseudoaneurysm/hemorrhage in the interpolar region of the right kidney with new distortion of the right renal cortex and suggestion of active bleeding (Figure 1).
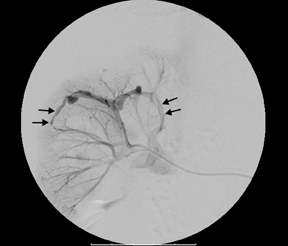
A right renal arteriogram showed 2 right renal arteries (Figure 1). The more inferior accessory renal artery was initially selected and revealed no evidence of active extravasation, pseudoaneurysm, or arteriovenous (AV) fistula. Selection of the main renal artery showed multiple areas of small pseudoaneursym formation and active extravasations with AV fistula formation in the interpolar to upper polar region of the right kidney(Figure 2). A 4 French cobra 2 catheter was advanced into a sub-segmental artery in the inter-upper polar region supplying a large pseudoaneurysm and AV fistula. These were coil embolized. Then a microcatheter was placed coaxially through the cobra catheter and subsequently smaller pseudoaneurysm and AV fistulas were coil embolized. A final arteriogram in the main renal artery showed no evidence of pseudoaneurysm, active extravasations, or AV fistula (Figure 2). About 25% of the right kidney was devascularized. No other complications were noted.
Diagnosis
Post-traumatic pseudoaneurysms and AV fistulas of the right renal artery
Discussion
Renal artery pseudoaneurysms are rare after blunt abdominal trauma. While they are common in penetrating injuries, only 20 cases after blunt trauma have been reported.1 These are caused by decelerating injuries of the renal artery after major falls or automobile accidents. In blunt trauma, strong deacceleration forces may cause the arterial injury. After the artery is completely or partially transected, hemorrhage may be contained in the surrounding tissues such as the vascular adventitia, Gerota’s fascia.2 Most patients present with hematuria, flank pain,mass, or hypertension. Delayed hemorrhage after renal trauma is a life threatening complication. Patients may be asymptomatic for many years, and a chronic pseudoaneurysm may expand and rupture before diagnosis or treatment. Treatment requires either surgical or percutaneous intervention. Surgical treatment of intraparenchymal aneurysm is usually partial nephrectomy or ligation of the parental artery which causes large amount of parenchymal loss. The angiographic approach can spare large portions of the involved kidney and preserve renal function.3
Often the diagnosis of renal artery pseudoaneurysm is made by CT, but magnetic resonance, Doppler sonography and renal perfusion imaging can be used as well. Angiography remains the gold standard to diagnose traumatic renal artery pseudoaneurysm and may reveal smaller lesions than the other techniques, as was demonstrated here.1 Moreover, with angiography concomitant therapeutic embolization can be provided.
Conclusion
Renal artery pseudoaneurysm after blunt abdominal trauma is uncommon but can be diagnosed with standard radiographic techniques. Treatment varies between open exploration and angiographic embolization. Minimally invasive therapy by super selective trans-catheter embolization provides permanent occlusion of the pseudoaneurysms that preserves maximum renal function. Our case was successfully managed with selective embolization without any medical complications.
- Mizobata Y, Yokota J, Fjuimura J, et al. Successful evaluation of pseudoaneurysm formation after blunt renal injury with dual-phase contrast-enhanced helical CT. AJR Am J Roentgenol. 2001;177:136-138.
- Lee DG, Lee SJ. Delayed hemorrhage from a pseudoaneurysm after blunt renal trauma. Intl J Urol. 2006;12: 909-911.
- Parildar M, Oran I, Memis A. Embolization of visceral pseudoaneurysms with platinum coils and N-butyl cyanoacrylate. Abdom Imag. 2003;28: 36-40.