Radiological Case: Arteriovenous malformation of the pancreas
Images




CASE SUMMARY
A 37-year-old man who had been alcoholic for 15 years presented to our hospital with complaints of abdominal pain in epigastric region for 3 months and melena for 2 days. The pain was of moderate intensity, radiating to the back, aggravated by food and relieved by vomiting. There was no past history of epistaxis, diabetes, hypertension, blood transfusion or any surgery. No family history of similar pain, gastrointestinal bleeding, mucocutaneous telangiectasia or epistaxis was noted. On physical examination, the patient had epigastric tenderness but no hepato-splenomegaly, ascites, jaundice or mucocutaneous telangiectasia. His laboratory investigations revealed haemoglobin level of 4.2gm%, serum amylase-299 and serum lipase-132.
IMAGING FINDINGS
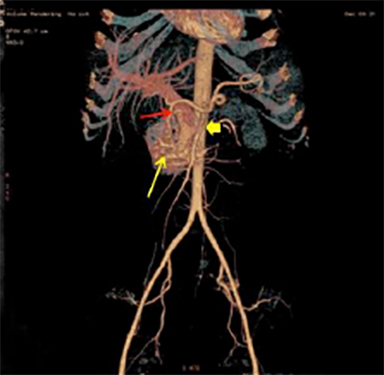
Upper-gastrointestinal endoscopy was normal. Computed tomography (CT) of the abdomen revealed multiple vessels in and around the head and uncinate process of the pancreas with feeding arteries from gastroduodenal artery (GDA) and superior mesenteric artery (SMA),early filling of superior mesenteric and portal veins and dense pancreatic stain in arterial phase (Figure 1). CT also revealed partial thrombus in the portal vein (Figure 2). CT findings were suggestive of arteriovenous malformation (AVM) of the pancreas.
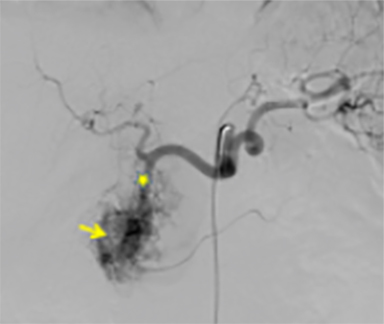
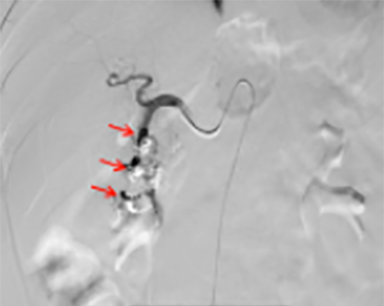
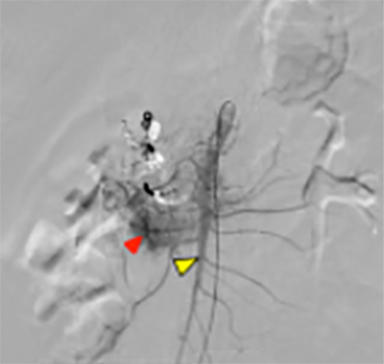
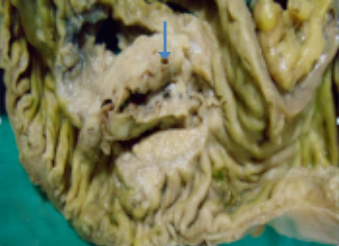
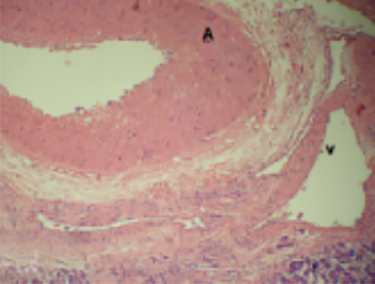
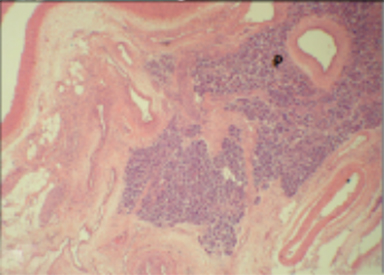
The celiac axis angiogram revealed dilated tortuous arteries, dense stain in the pancreatic head region and early filling of the veins (Figure 3A). Arterial feeders from GDA were embolized with gelfoam and coils. Post-embolization angiography showed neither a dense stainin the pancreas nor early filling of the veins (Figure 3B). Thereafter an SMA angiogram showed dilated tortuous feeding arteries and dense stain in the same region which could not be embolized (Figure 3C). The patient continued to have abdominal pain and bleeding that required multiple blood transfusions. The patient was taken for a laparotomy, which revealed bulky head of pancreas and multiple vessels around the head and uncinate process of pancreas. A Whipple’s pancreaticoduodenectomy was performed. The histopathological findings were suggestive of arteriovenous malformation of head and uncinate process of pancreas (Figure 4A-C).
DIAGNOSIS
Arteriovenous malformation of pancreas
DISCUSSION
Arteriovenous malformation (AVM) of the pancreas is a very rare disorder, first reported by Halpern et al in 1968 in a patient with Osler-Weber-Rendu disease and described as tumorous formation or vascular anomaly formed by aberrant communication between arterial and venous systems.1 It can be either congenital or acquired in origin. Congenital pancreatic AVM can be an isolated finding or it can be associated with Osler-Weber-Rendu disease, an autosomal dominant syndrome, in 10-30% of patients.2 Acquired pancreatic AVM is less common and may be secondary to inflammation, tumor, trauma or complications of pancreatic transplantation.3 The most common location of pancreatic AVMs is in the head of the pancreas. Takemoto et al in 2007 reviewed 90 cases of pancreatic AVM and reported that these were congenital in 49 (54%) and acquired in 5 (6%) patients. In 36 (40%) patients the etiology was not known. Takemoto et al also found that the location of pancreatic AVM was in the head in 37 (41%) patients, head and body in 9 (10%) patients, body in 9 (10%) patients, body and tail in 15 (17%) patients, tail in 7 (8%) patients and in the entire pancreas in 13 (14%) patients.4
The most common symptoms of pancreatic AVM are gastrointestinal bleeding, abdominal pain and jaundice. Gastrointestinal bleeding can occur by rupture of the AVM into pancreatic duct or into the submucosal layer of gastrointestinal tract, or through esophageal and/or gastric variceal bleeding due to portal hypertension caused by pancreatic AVM.5
Takemoto et al, in their review of 90 cases of pancreatic AVM, found the mean age of patients to be 52.5 years, with a range from 7 month to73 years, with a M:F ratio of 73:17. They also found that, of these 90 patients, 48 (54%) presented with gastrointestinal bleeding, 27 (30%) with abdominal pain, 4 (4%) with jaundice, 2 (2%) with abdominal discomfort and 14 (14%) asymptomatic.4
Pancreatic arteriovenous malformation may be associated with portal hypertension, portal vein thrombosis and pancreatitis. The predisposing factors for portal vein thrombosis are hepatic diseases, abdominal inflammation, hypercoagulability, abdominal interventions, malignancies and myeloproliferative syndrome.6 However, the cause is not known in nearly half of patients, as in our case.7 The etiology of pancreatitis in these patients may be bleeding into the pancreatic duct, or pancreatic arteriovenous malformation with vascular steal causing ischemia or pancreatic duct compression.5
Abdominal ultrasonography is an initial non-invasive imaging modality and demonstrates hypoechoic linear and nodular structures in and around the pancreas with mosaic flow pattern and pulastile waveform in the portal vein on Doppler sonography.8 CT and MRI provide more detailed information of the pancreatic arteriovenous malformation. CT is now used as the primary imaging modality in pancreatic AVM to demonstrate the network of multiple intrapancreatic and peripancreatic vessels with early enhancement of the portal vein in the arterial phase. Postprocessing techniques such as maximum intensity projection (MIP), multiplanar reformation (MPR) and volume rendering (VR)are very useful in evaluating the anomaly in detail and demonstrating the arterial feeders and draining veins.9 On MRI, pancreatic AVM is seen as a heterogeneous area of signal void structures. Angiography is an invasive method and demonstrates dilated tortuous feeding arteries, a racemose intrapancreatic vascular network producing transient, dense staining of pancreas, and early filling of veins, such as the portal vein in arterial phase, followed by early clearance of the pancreatic stain.10
The differential diagnoses for pancreatic arteriovenous malformation are neuroendocrine tumors, hypervascular metastases, and intrapancreatic accessory spleen.
The radical treatment for pancreatic arteriovenous malformation is complete or partial resection of pancreas. The other treatment options for pancreatic AVM are transarterial embolization (TAE), transjugular intrahepatic portosystemic shunt (TIPS), vascular ligation and radiation therapy.2
CONCLUSION
The pancreatic arteriovenous malformation is a rare cause of gastrointestinal bleeding or abdominal pain and may lead to complications like portal hypertension, portal vein thrombosis and pancreatitis. CT is the primary imaging modality used to confirm the diagnosis and to help in treatment planning. Surgery is the only definitive treatment of pancreatic AVM.
REFERENCES
- Halpern M, Turner AF, Citron BP. Hereditary hemorrhagic telangiectasia. An angiographic study of abdominal visceral angiodysplasias associated with gastrointestinal hemorrhage. Radiology. 1968;90:1143-1149.
- Nishiyama R, Kawanishi Y, Mitsuhashi H, et al. Management of pancreatic arteriovenous malformation. J Hepatobiliary Pancreat Surg. 2000;7:438–442.
- Butte JM, San Francisco IF, Pacheco F, Solar A, Crovari FJ, Jarufe NP. Arteriovenous malformation of the pancreas: Report of a case. Surg Today. 2007;37:604–607.
- Takemoto I, Tsuda M, Yano Y, et al. Pancreatic arteriovenous malformation combined with portal thrombosis. Intern Med. 2007;46:233-236.
- Kanno A, Satoh K, Kimura K, et al. Acute pancreatitis due to pancreatic arteriovenous malformation: 2 case reports and review of the literature. Pancreas. 2006;32:422-425.
- Jenssen HL, Wijnhoud A, Haagsma EB, et al. Extrahepatic portal vein thrombosi: Aetiology and determinants of survival. Gut. 2001;49:720-724.
- Bayraktar Y, Harmanci O. Etiology and consequences of thrombosis in abdominal vessels. World J Gastroenterol. 2006;12: 1165-1174.
- Koito K, Namieno T, Nagakawa T, Ichimura T, Hirokawa N, Mukaiya M, et al. Congenital arteriovenous malformation of the pancreas: its diagnostic features on images. Pancreas. 2001; 22: 267-273.
- Endo K, Sata N, Shimura K, Yasuda Y. Pancreatic arteriovenous malformation: A case report of hemodynamic and three dimensional morphological analysis using multi-detector row computed tomography and post-processing methods. J Pancreas.2009;10:59-63.
- Chuang VP, Pulmano CM, Walter JF, Cho KJ: Angiography of pancreatic arteriovenous malformation. Am J Roentgenol. 1977; 129:1015-1018.