Radiological Case of the Month: Neuroblastoma
Images


Prepared by Craig E. Barnes, MD; Ashley D. Hawkins, BA; and Michael Y. Chen, MD, Department of Radiology, Wake Forest University School of Medicine,Winston-Salem, NC.
CASE SUMMARY
A healthy 2-month-old white infant boy was found by his pediatrician to have a palpable pelvic mass at his well child check. The patient had no clinical symptoms at the time. Laboratory values were significant for an elevated urine homovanillic acid (HVA)/creatinine ratio of 361, and a normal urine vanillylmandelic acid (VMA)/creatinine ratio. Radiography (Figure 1), ultrasonography (Figure 2), computed tomography (CT) (Figure 3), and magnetic resonance (MR) imaging (Figure 4) were performed.
DIAGNOSIS
Neuroblastoma
IMAGING FINDINGS
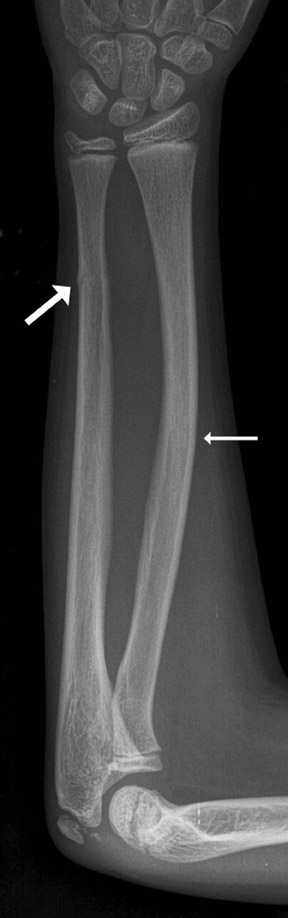
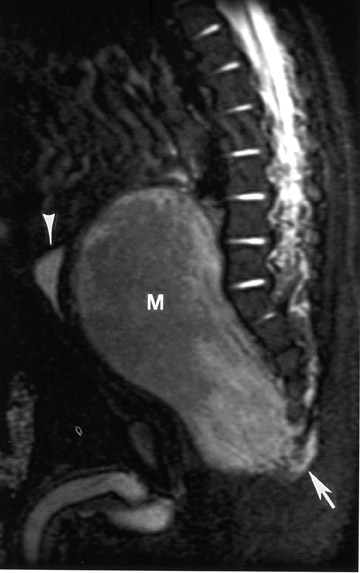
Radiography showed a pelvic soft-tissue fullness displacing the bowel loops (Figure 1). No calcifications or bone changes were noted. Ultrasonography confirmed the presence of a heterogeneous, solid, presacral pelvic mass measuring 8.1 × 3.6 × 5.3 cm that displaced the rectum and bladder anteriorly (Figure 2). The contrast-enhanced CT scan showed a large central retroperitoneal mass of the pelvis measuring 5.2 × 4.4 × 7.3 cm and extending from the lower pelvis to the umbilicus (Figure 3). There was also lateral displacement of the ureters and iliac arteries with suggestion of soft-tissue extension around the lower sacrum and coccyx. MR imaging of the lumbrosacral spine with (not shown) and without (Figure 4) contrast showed an 8.6 × 4.2 × 4.6 cm heterogeneously enhancing mass (Figure 4). The mass wrapped around the coccyx and lower sacrum into the distal-most neuroforamina on the right, which suggested a possible neural origin.
SURGICAL AND PATHOLOGICAL FINDINGS
During surgery, it was noted that the pelvic tumor had displaced many internal organs. The colon was deviated toward the left, the ureters were deviated laterally, and the rectum was shifted from behind the bladder toward the left. The excised tumor measured 7.5 × 7.0 × 3.7 cm.
A bone-marrow biopsy and postoperative bone survey were both negative. Histologic evaluation showed an undifferentiated, small round, blue-cell tumor in a fibrillar background, a pattern favoring neuroblastoma. Frozen-section pathology confirmed the diagnosis of neuroblastoma.
DISCUSSION
Neuroblastoma, which most commonly occurs in children <2 years old, often presents with a large, fixed lobular mass that extends from the flank toward the midline of the abdomen and frequently surrounds retroperitoneal structures. 1 Eighty percent of all neuroblastomas arise in the abdomen and thorax, with the most common site being the adrenal medulla. Only 5% of all primary neuroblastoma tumors arise in the pelvis. 1,2 Diagnosis and evaluation of childhood tumors usually include assays for the urinary catecholamines HVA and VMA, as they are produced by 85% to 90% of neuroblastomas. 1
The role of imaging in childhood tumors includes confirming the presence of a tumor, determining the site of origin of the tumor, helping in tumor staging, and helping in treatment planning. 3 Radiographic differential diagnoses of presacral masses in children include sacrococcygeal teratoma, anterior meningocele, neuroenteric cyst, and lymphoma. 4 Sacrococcygeal teratomas are the most common childhood tumors seen in the presacral region. Fat, calcification, and/or cystic changes within a presacral mass would make this diagnosis more like- 3,4 In myelomeningocele and neurenteric cyst an accompanying sacral defect is usually seen. 4 Lymphomas are not commonly presacral and most often are associated with retroperitoneal and mesenteric lymphadenopathy. 4
Abdominal radiography showed a soft-tissue mass in the lower pelvis, displacing the bowel superiorly. This is a nonspecific sign. In our case, ultrasonography showed a heterogeneous, solid well-demarcated presacral pelvic mass of mixed echogenicity. Areas of increased echogenicity were thought to represent fatty deposition or calcification. Doppler sonography showed prominent vessels within the tumor along its posterior-inferior margin. On CT scan, the neuroblastoma appeared as a presacral soft-tissue mass with high attenuation within it, which represented calcifications. MR imaging has been touted as a better way to evaluate cases of suspected neuroblastoma because of its ability to delineate how the tumor relates to local musculature and to assess the intraspinal involvement. 3,4 On the MR imaging study, the lack of fat or cystic change made a presacral sacrococcygeal teratoma unlikely. The presence of a solid mass with extension around the coccyx and into the distal-most right neuroforamina was seen on MR imaging. This finding is consistent with the diagnosis of neuroblastoma, which can have intraspinal extension secondary to its neural origin.
CONCLUSION
We have reported an unusual case of neuroblastoma presenting as a presacral mass in an otherwise healthy child. The lack of fat or cystic
change makes sacrococcygeal teratoma a less likely diagnosis. The presence of a solid mass in an infant having neuroforaminal extension and calcification should prompt consideration of neuroblastoma. This case of neuroblastoma stresses the importance of searching for clues to the diagnosis, such as neuroforaminal extension and calcification, as common diseases may present in uncommon sites.