Spontaneous retroclival subdural hematoma associated with anticoagulation
Images
CASE SUMMARY
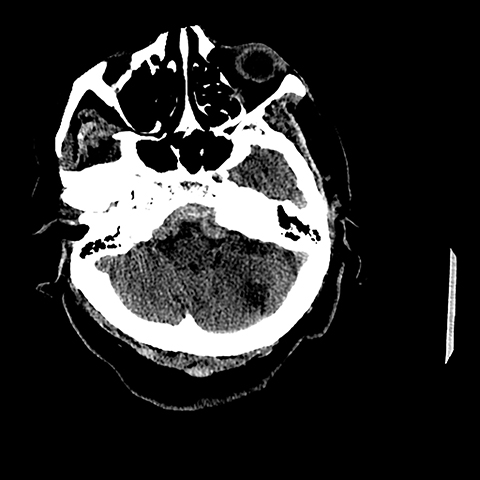
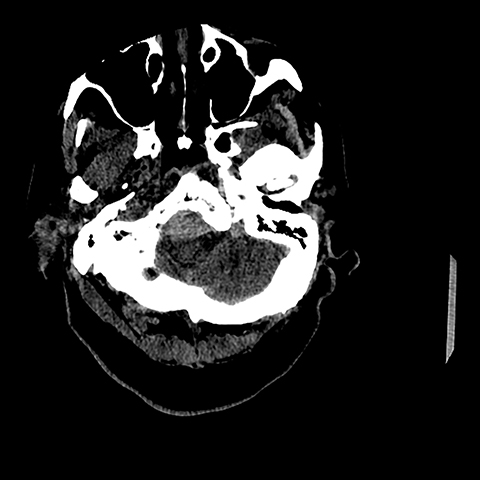
A 72-year-old female with a past history of a right frontoparietal stroke and residual left hemiparesis presented to the ER with a one-day history of headache and confusion. One month previously she had been diagnosed with a deep venous thrombosis in her leg and had been started on lovenox and Coumadin. There was no reported history of antecedent trauma. Physical exam, other than the residual deficits from her previous infarct, was noncontributory. Laboratory values were within normal limits given patient’s current anticoagulation status. A noncontrast head CT was subsequently performed and demonstrated an area of extra-axial hyperdensity marginating the clivus and extending from the most inferiorly visualized aspect of the anterior foramen magnum cephalad towards the left and right cerebellopontine angle cisterns (Figures 1,2). A spontaneous retroclival subdural hematoma was suspected. Less likely considerations included an extra-axial hypercellular mass such as meningioma, lymphoma or plasmacytoma.
IMAGING FINDINGS
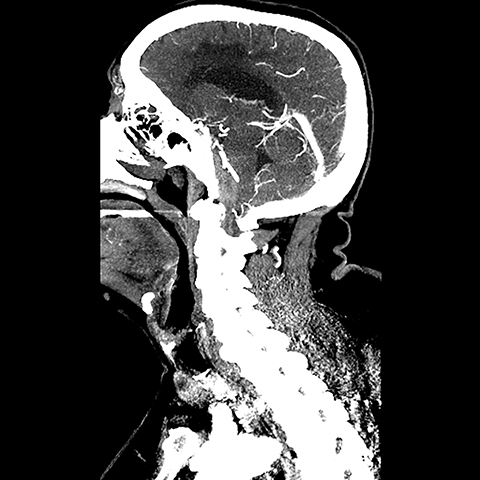
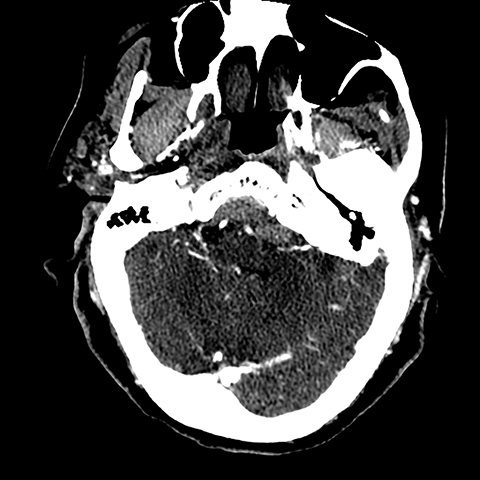
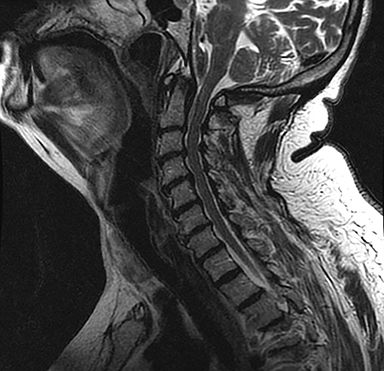
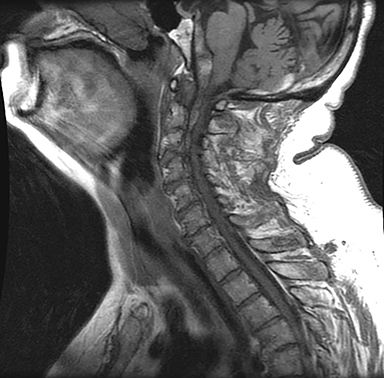
A CT angiogram of the head and neck was performed next to exclude any regional vascular anomalies, such as an occult arteriovenous malformation or dissection, as well as to assess for any abnormal regional enhancement. There was no evidence of an underlying enhancing mass or regional aberrant vessels (Figures 2,3). Elevation and dorsal displacement of the distal V4 vertebral artery segments and the basilar artery was observed (Figure 4). Anticoagulation was reversed in the ER with fresh frozen plasma and vitamin K was begun; the patient was subsequently admitted for supportive care and observation. At that time, an MRI of the brain and cervical spine, ordered to ensure a bland nature of the hemorrhage and to completely exclude any underlying mass, demonstrated the hematoma to have predominantly low signal on T2 FSE images and high signal on T1, consistent with intracellular methemoglobin. There was dissection from the superior aspect of the clivus distally through the anterior foramen magnum into the ventral spinal canal. The hematoma was noted to overlay an intact, otherwise unremarkable tectorial membrane and to extend distal to the membrane attachment at the dorsal mid C2 vertebral body, consistent with a subdural location (Figures 5,6). As a final step in the workup, a four vessel cerebral angiogram, not shown, was done to exclude any small contributory distal vertebral aneurysms and proved negative in this regard. After an uneventful 10-day hospital course during which temporal evolution and progressive resolution of the hemorrhage was observed on a follow-up CT exam, the patient was discharged back to a skilled nursing care facility. DVT prophylaxis was reinitiated with subcutaneous heparin and a return appointment as an outpatient with the neurosurgery clinic was scheduled.
DIAGNOSIS
Extra-axial hemorrhage isolated to the posterior fossa retroclival region is a rare imaging finding. Perimesencephalic spontaneous venous bleeding in the subarachnoid space is perhaps the most familiar entity, posing a diagnostic conundrum for the interpreting radiologist and necessitating a workup for ruptured aneurysm. Actual bleeding in the subdural or epidural region is even less common with most cases occurring in the epidural space in children in conjunction with blunt trauma and skull base fracture or tectorial membrane injury. A higher fulcrum of neck motion in pediatric patients, weaker neck musculature and greater ligamentous laxity predisposes this area to injury.1 The hemorrhage is typically bounded by the tectorial membrane, the cephalad continuation of the posterior longitudinal ligament, and is constrained by the ligamentous attachment at the posterior C2 vertebral body from any inferior extension. In contrast, subdural hemorrhage in the retroclival region has an adult predilection and, lacking such ligamentous constraint, can dissect both posteriorly at the foramen magnum as well as inferiorly into the spinal subdural space.2 In addition to trauma, bleeding diatheses, regional vascular anomalies, occipital surgery, and pituitary hemorrhage have all been described as inciting factors.1,3,4 Management and outcome depends on the extent of any concurrent injuries and the degree of brainstem compression. In addition to headache, cranial nerve palsies may occur transiently secondary to locoregional mass effect. The sixth nerve, due to its longer course of ascent and relative exposure, is the most frequently affected. The majority of reported patients, in the absence of significant co-morbidities, do well and are managed expectantly with clearing of the hemorrhage over one to two weeks.5,6
DISCUSSION
Retroclival hematoma is an uncommon finding, typically occurring in the epidural space in pediatric patients following significant blunt trauma. There are usually coexisting injuries to the skull base or craniocervical ligaments, most commonly the tectorial membrane.2,7 The hemorrhage may compress the brainstem resulting in altered levels of consciousness, paresis and paralysis. As with subdural hematomas at this level, cranial nerve palsies may also occur. Most commonly the sixth nerve is affected resulting in lateral rectus palsy due to its relatively longer course of exposure as it ascends from the pontomedullary junction to the petrous apex and Dorello’s canal.7 Children are more predisposed for epidural hemorrhage at this level due to their higher fulcrum of cranial cervical motion and relative ligamentous laxity. The abrupt acceleration/deceleration injury that ensues in high energy blunt trauma strips the tectorial membrane from the occipital bone at the foramen magnum and the posterior aspect of the C1 anterior arch.1 Concomitant shearing of the vessels of the basilar venous plexus and dorsal meningeal branch of the meningohypophyseal trunk results into either mixed, venous or arterial bleeding within the epidural space.2 Stretching injury to the tectorial membrane was seen in 70% of patients in one surgical series.8
As with subdural hemorrhage at this level, the typical CT finding is focal hyperdensity posterior to the clivus with variable degrees of mass effect upon the adjacent brainstem. MRI is of utility in defining the extent of the hemorrhage and in evaluating for concomitant soft tissue injury as manifest by loss of ligamentous continuity or as increased internal T2 signal in the case of an incomplete tear.2 As opposed to epidural hemorrhage, bleeding in the subdural space at this level is not constrained by ligamentous attachments and is free to diffuse into the spinal subdural space inferior to the C1-2 level as well cranially into the ventral and retrocerebellar aspects of the posterior fossa.2,6 Additionally, the tectorial membrane is typically intact and firmly attached both to the clivus and at its inferior attachment at the posterior mid axis body. The hemorrhage is thought to be due to disruption of petrosal and bridging cortical veins at the foramen magnum.2
Retroclival subdural hematomas are overall less common than epidural hemorrhage at this location and occur more often in the adult population.1,2,7 Overall they represent only 0.3% of acute subdurals.5 Though trauma may be an inciting factor, other etiologies reported have included hemophilia or iatrogenic anticoagulation, pituitary apoplexy, ruptured AVM, and decompressive craniectomy.1,3,4,9,10 The clinical presentation may mimic that of a subarachnoid hemorrhage with abrupt onset of a thunderclap headache.5 Cranial nerve palsies may ensue secondary to locoregional mass effect, typically the sixth nerve being most commonly affected. The hemorrhage, as previously stated, can diffuse into the subdural space of the spine and posterior fossa. MRI will best show typically high T1 methemoglobin extending distal to the mid-axis body, overlying the intact, uninjured tectorial membrane at the craniocervical junction. Additionally the presence of hemorrhage extending more laterally and posteriorly at the foramen magnum supports a subdural location.2,5
Given the potential association with underlying vascular malformations, it was felt prudent in our case, as had been done in other reported instances, to proceed with catheter angiography to completely exclude an underlying anomaly. In other published cases, however, CT angiography and MR imaging alone have been felt to suffice.5,10 In the absence of significant comorbidities, the overall prognosis is good. Without neurological deficits, management is conservative and expectant with most hematomas clearing by two weeks.1,2,5
CONCLUSION
In conclusion, though an uncommon entity, retroclival hematomas are an important diagnostic finding to make due to their potential for significant neural compression as well as their association with underlying osseous and ligamentous injury, especially in the pediatric population. Epidural hemorrhage, as seen in this group, will typically be constrained by an overlying attenuated tectorial membrane, partially stripped from the clivus and subjacent atlanto-axial junction. Subdural bleeding, in distinction, can diffuse freely into the posterior fossa and spinal subdural spaces and may be seen posteriorly and laterally at the level of the foramen magnum or extending below the mid axis body. Management is based on the extent of any neurological and soft tissue co-injuries. In their absence, care is expectant and conservative.
REFERENCES
- Guillaume D, Menezes A Retroclival hematoma in the pediatric population: Report of two cases and review of the literature. J. Neurosurg: Pediatrics. 2006;105:321-325.
- Koshy J, Scheurkogel M, Clough L. Neuroimaging findings of retroclival hemorrhage in children: a diagnostic conundrum. Childs Nerv Syst. 2014;30:835-839.
- Myers D, Moossy J, Ragni M. Fatal clival subdural hematoma in a hemophiliac. Annals Emerg Med. 1995;25(2):249-252.
- Goodman J, Kuzma B, Britt P. Retroclival hematoma secondary to pituitary apoplexy. Surg Neurol. 1997;47:79-80.
- Casey D, Chaudhary B, Leach P. Traumatic clival subdural hematoma in an adult. J Neurosurg. 209;110:1238-1241.
- Ahn E, Smith E. Acute clival and spinal subdural hematoma with spontaneous resolution: clinical and radiographic correlation in support of a proposed pathophysiological mechanism. J. Neurosurg: Pediatrics. 2005;103:175-179.
- Tubbs R, Griessenauer C, Hankinson T. Retroclival epidural hematomas: a clinical series. Neurosurgery. 2010;67(2) 404-406.
- Meoded A, Singhi S, Poretti A. Tectorial membrane injury: frequently overlooked in pediatric traumatic head injury. AJNR. 2011;32:1806-1811.
- Guilloton L, Godon P, Drouet A. Retroclival hematoma in a pati1ent taking oral anticoagulants. Rev Neurol. 2000;156:392-394.
- Datta N, Chan K, Kwok, J. Posterior fossa subdural hematoma due to a ruptured arteriovenous malformation. Neurosurg Focus. 2000;8(6):ecp 1.
Citation
A S, M R, P D. Spontaneous retroclival subdural hematoma associated with anticoagulation. Appl Radiol. 2017;(3):38-41.
March 4, 2017