Technology Trends: A view of the future image exchange
Images
With reimbursements plummeting, leaving financial growth at many health care practices flat, investing in more IT infrastructure seems counterintuitive.
Yet, doing so is virtually unavoidable.
Hospitals and radiology practices need to implement image-enabled electronic health records (EHR) and meet Meaningful Use Stage 2(MU2) criteria. They also face larger workloads once the federally mandated health information exchanges (HIEs) take hold. With such vastchanges unfolding, streamlining radiology workflow is more critical than ever. Fortunately, efficient and economical options exist to implement networks that support an image exchange with referring physicians and even patients.
Changing health care landscape
Several factors are pushing health care networks to consolidate their imaging data and improve workflow efficiency. The first involves reimbursement and referring physicians. The proposed 2014 Hospital Outpatient Prospective Payment System (HOPPS) rule would cut hospital outpatient payment rates for computed tomography (CT) and magnetic resonance imaging (MRI) services by 18% and 38%, respectively.1 In addition, the proposed Medicare Physician Fee Schedule (MPFS) would reduce the technical component payment rates for some CT studies by approximately 30% and some MRI studies by 16%.1
Considering each referring physician contributes about $1.5 million in annual revenue to an imaging center,2 it is in the interest of radiologists to provide an efficient and convenient system to receive orders from and deliver reports to their referring physicians. The challenge is that there are various systems and methods to choose from, and the lack of standardized workflows creates inefficiencies and opportunities for error.
One of the core mandates of MU2 is that EHRs must accommodate computerized physician order entry (CPOE) for at least 30% of radiology exam orders. Radiologists may readily comply with MU2 by choosing image-enabled EHRs to provide access to at least 10% of all images a physician accesses.2
“Data sharing technologies … promise to be game changers when it comes to working with EHRs. Not only do they make report and image exchange faster and easier for referring physicians and radiology providers, they enable providers to meet the demands of MeaningfulUse and improve patient care in the process,” said Ron Cornett, Director of Information Technology (IT), Radiology Ltd.
Image consolidation across the enterprise
The ideal image-exchange platform would include a complete, longitudinal record that goes beyond radiology, connects all clinical department imaging data to a central repository, supports zero-footprint viewers, and provides access to referring physicians as well as to patients.
The two key tools for consolidating imaging data across large hospital networks are vendor neutral archives (VNA) and PACS enterprise archive solutions. In a 2012 KLAS survey, 27% of respondents said a VNA would be central to their strategy, while 25% preferred a PACS-centric archive. Hospitals with > 500 beds selected a VNA more than other types of facilities, while facilities with < 500 beds more often opted for a PACS enterprise solution.3
The same report identified 3 tiers of providers: primary vendors that offer VNA functionality without a PACS, vendors that offer a VNA and a PACS, and a tier of specific vendors whose customers are especially interested in the PACS enterprise archive solution. Whichever approach is adopted, putting all of the pieces together is a step-by-step process.
Taking the VNA route
The need for centralized storage of standard-compliant images is driving the adoption of VNAs—particularly among large hospital networks. The 2013 global VNA market is estimated at $165.3 million and is poised to reach $335.4 million by 2018, at a CAGR of 15.2%.4 The VNA model’s appeal lies in its technology and cost-related benefits, such as supporting best-of-breed solutions. However, a lack of established VNA definitions are resulting in confusion and data insecurity (breaches)—issues that restrict market growth.4
A VNA is a comprehensive, cloud-based image storage and management solution. Images are archived on a short- and/or long-term basis, and storage is scalable. VNAs enable the consolidation of imaging data from multiple PACS, and products integrating VNAs with EHRs are a growing trend.
UCSD Health System
“The discussion for a VNA is soon going to engulf all of health care in the U.S.,” said Hamed Aryafar, MD, Assistant Professor of Vascular and Interventional Radiology, University of California San Diego (UCSD) Health Sciences, part of the UCSD Health System. “Healthcare organizations will have to find ways to consolidate their imaging data—from all sources, not just radiology—and will need to find ways to provide those to other organizations that may be taking care of the same patients. This will require an affordable solution that does not incur significant additional costs for each new interface or access point that requests this data.”
The UCSD Health System is looking at a VNA platform. The UCSD Health System is now deploying iConnect Access to the hospital,which will be used by all UCSD physicians and referring clinicians that have signed up for access to EPIC, the network’s EHR. iConnectAccess, by Merge Healthcare, is a zero-download DICOM image viewer.
“iConnect provides an easy portal for clinicians to pull up images while they are reviewing their patient charts through EPIC. This also allows them to ‘see’ the findings and diagnoses that the radiologists have elucidated in their reports,” said Dr. Aryafar. “The referring clinician can now be more empowered about the imaging that they regularly order and will be able to help their patients understand their disease process.”
A VNA can enhance service and quality of care. “If the radiologists can now review the cardiology echocardiogram, actual photographs of the disease process, the patient’s outside imaging, and even provide second opinions on such data for the referring clinicians, there is an exponential increase in the quality of care that they can provide,” Dr. Aryafar noted.
VNAs also support patient access to medical records. Patients in the UCSD Health System can already view their lab reports and communicate with their physicians, and Dr. Aryafar anticipates patients will eventually want access to their imaging reports. This will require radiologists to produce a patient’s version of the report, using terminology patients can understand. “As in mammography now, there will likely be a need for a ‘patient’ version of the report or letter that sums up the findings in clear terms,” said Dr. Aryafar. “Once the growing pains are over, this will be a resource that we won’t be able to live without.”
Cleveland Clinic
The Cleveland Clinic is also adopting the VNA model for its internal and external imaging network, which includes 35 imaging centers.“The first step was to integrate image data into the EHR. We are an enterprise, so images come from the main campus of the ClevelandClinic, family health centers and regional hospitals,” explained Cheryl Petersilge, MD, clinical professor of radiology, medical director, MyPractice Imaging, Information Technology Division, Cleveland, OH.
The process started in radiology, where clinicians were using a VNA for data storage. Once radiology image and contextual data was consolidated in the EHR, Martin Harris, MD, CIO for Cleveland Clinic, spearheaded the campaign to make images available to all stakeholders in the health system. “Our physicians are mobile,seeing patients at different geographic sites, and we needed to store the data electronically so that it is accessible from any location,” said Dr.Petersilge.
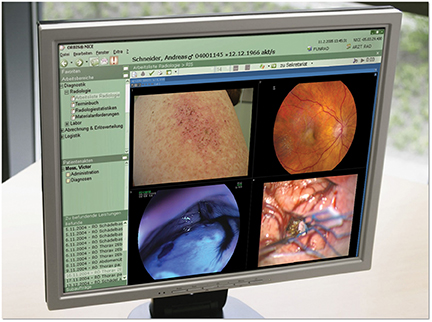
In addition to CT, MR, ultrasound, and x-ray images, the EHR accommodates endoscopy images, women’s health, and point-of-care ultrasound images from rheumatology and anesthesiology, as well as clinical photographs from the wound program and dermatology department (Figure 1). An imaging tab in the EHR lists all examinations patients have had.
“What our enterprise has done is taken the Agfa ICIS view 3.0, which is a vendor-neutral archive developed for radiology because you[can] bring in images from any different vendor system. That way, if you change vendors, you’re not going to have to roll over all of your storage. We are leveraging that to bring in nonradiology-generated images,” said Dr. Petersilge.
“As we affiliate with other hospitals … we are looking at how we can use the VNA and other associated software that helps us move images around and see images without moving them from other sites,” added Dave Piraino, MD, imaging informatics officer, Cleveland ClinicImaging Institute, Cleveland, Ohio.
VNA storage management
Reducing the required amount of storage is another advantage of a VNA.
“The image volume size is increasing, so storage is getting more costly,” said George McCulloch, Deputy CIO of the Informatics Center at the Vanderbilt University Medical Center.
Placing studies in a central location, however, eliminates storage redundancy. It also permits users to see images directly from the unified cloud-based viewer. And because the data is not sent over the Internet to different locations but viewed from one location, there is no change to the data, preserving data integrity. Vanderbilt’s network, including 3 campus buildings and 18 affiliate locations, chose to consolidate its clinical images in a VNA provided by TeraMedica. “We are preparing for the future of Meaningful Use Stage 2, which dictates the need to share images, for continuity of care, and to avoid duplicate images across our affiliates,” explained McCulloch.
Eliminating duplication is a challenge when distributing images between a PACS and an image viewer. Because the DICOM headers are proprietary to the vendor, when radiologists retrieve priors, the VNA takes the proprietary file storage and puts it back into a standard file type,essentially “unpacking” or “repacking” the data. “We have to send the image to the VNA automatically to unpack, create a jpeg, and put the datain the DICOM viewer in the database. The question is how much time it will take,” he said.
Similarly, Colorado Telehealth Network (CTN) built the CTN Colorado Imaging Exchange around a cloud-based VNA. Acuo Technologies provided VNA services and Client Outlook the diagnostic-quality medical image viewer. Today, the network enables hospitals, imaging centers, clinics, and other providers in Colorado to safely store and share medical images through a private cloud.
VNAs ease consolidation
Independent community hospitals are finding it increasingly difficult to compete, and as such, hospitals and medical practices are consolidating.5 In June 2013 alone there were 92 merger- and-acquisition transactions with a reported value of $20.6 billion, up from 68 such transactions totaling $9.4 billion in May.
The trend highlights the importance of efficient data sharing. For Intermountain Healthcare in Salt Lake City, Utah, implementing an image-sharing network accessible to over 10,000 practitioners, external referring physicians, and other occasional users was no small feat. The provider was faced with unifying multiple vendor archives and different viewers across widely dispersed facilities.
Intermountain found its solution in Siemens’ Image Sharing & Archiving (ISA) a VNA that stores images from any modality in the Siemens Healthcare Computing Center (HCC). Images are redundantly hosted in a Dell data center, and the archive is managed with Dell’s clinical data management software.
The next step for Intermountain was to connect its current archives and provide all clinicians with fast, real-time access to patient images through one consistent and easy-to-use interface. The facility selected ResolutionMD by Calgary Scientific as its enterprise viewing solution, and is working with Calgary Scientific to deliver radiology images directly to referring physicians embedded within the EHR. To date,ResolutionMD has been successfully integrated with the Intermountain’s EHR. When full deployment is completed, Intermountain will have one integrated enterprise viewer that leverages its current architecture and creates a virtual database system that eliminates the need to copy or move data across the archives.
“We wanted a solution that did not require any downloads, was fully secure, had the proper FDA clearances for diagnosis, worked with our entire IT infrastructure, and met the speed and scalability requirements that are always at the top of our user lists. ResolutionMD andSiemens delivered all of these requirements while providing mobile capability that will allow us to easily roll out better image access to our staff,” said Geoff Duke, Director, Imaging Informatics at Intermountain Healthcare.
VNA benefits for radiology practices
In a market undergoing consolidation, radiology practices need to cut costs and still find ways to grow. This is where the cost benefits of a VNA add up. In a practice with a referring base of 2,000 physicians, the cost of connecting 1,000 different EHR systems to a bidirectional HL7 feed, plus yearly maintenance, was largely unsustainable for Radiology Ltd.
The radiology practice developed a plan to implement a web-based PACS that stores and provides access to images from any web-based location, as well as a web-based radiology information system (RIS) to streamline workflow and enable referring providers to meet Meaningful Use criteria.
To do this, Radiology Ltd. implemented iConnect Access. Although the new network requires referring physicians to upgrade their ownEMR systems to a version that supports the technology, it provides this private practice an avenue to expand its referral base. “We will enable our business to potentially connect to hundreds of thousands of referring physicians without a single HL7 interface. With this system,we will not only be able to create the reports, but also be able to embed within each report a link to the corresponding patient’s images and send the entire package directly to the physician for immediate review on his/her own EHR system,” said Cornett. “This new strategy gives practices like ours a way to ride existing systems to meet Meaningful Use standards at a price that’s reasonable and sustainable over the longterm.”
Taking advantage of the best-of-breed capabilities of VNAs, earlier this year, Fujifilm Medical Systems announced that it added a VNA component into its Synapse portfolio. Synapse VNA will enable Synapse PACS, Synapse RIS, Synapse Cardiovascular, cloud services, and Fujifilm’s entire informatics platform to communicate seamlessly with all databases and storage systems throughout a healthcare facility’sIT infrastructure (Figure 2). The company also extended the continuum of care to mobile devices with its zero footprint mobile application, Synapse Mobility.
PACS enterprise-archive solutions
The role of PACS is expanding beyond radiology, as almost any PACS today can streamline connectivity to EHRs and health information exchange (HIE) platforms via local edge devices or cloud servers.6 Then add on an image viewer for shared viewing by referring physicians and radiologists. Viewers are increasingly sophisticated. A full-featured medical imaging viewer, such as NilRead by Claron Technologies, supports diagnostic viewing of all cleared DICOM imaging modalities, including PET/CT fusion.
Many hospitals are taking the PACS enterprise-archive centric approach; projections show the enterprise PACS segment is growing faster than departmental PACS and is expected to reach $510 million by 2018, at an almost double CAGR.
When the University of Miami acquired the University of Miami Hospital, the large health system implemented a single PACS across the entire network. “We wanted an enterprise solution more similar to the radiology system. If a radiologist wanted to look at a study remotely,the study needed to be loaded quickly, and to cache studies without relying on local bandwidth,” explained Dr. Gary Danton, Chief of Imaging Informatics for the Department of Radiology at University of Miami.
They chose IntelliSpace PACS 4.4 by Philips Healthcare to centralize PACS enterprise wide. IntelliSpacePACS 4.4 incorporates several enterprise imaging features, including IntelliSpace PACS Federation, which allows users to view other IntelliSpace PACS archives, gain access to disparate PACS, and to present reports and images to a clinician with a view of a patient’s imaging history. Because IntelliSpace PACS 4.4 is interoperable, the UHealth could integrate it with existing software. “We looked for a PACS with an open API and the ability to integrate other software without additional fees. We use OrthoCAD, TeraRecon, voice recognition systems, and our EHR. An open API makes that easy to do,” Dr. Danton noted.
Another important feature was the image viewer embedded in the EHR. “It allows us to give preliminary reads offsite easily and access images more quickly while doing clinic through the EHR,” said Danton. “Now patients can get imaging studies done at any hospital throughout the entire UHealth system because all of the imaging is stored in one PACS.”
Another popular PACS enterprise archive is GE Healthcare’s Centricity Clinical Archive solution. Unlike VNAs that only support departmental DICOM consolidation, Centricity Clinical Archive unifies patients’ images and documents across the care continuum. The Centricity PACS has a universal viewer for clinicians to streamline diagnosis and results turnaround time.
Internet-based image exchange
It is possible to bypass the VNA and PACS enterprise archive model altogether, and still establish an image-sharing strategy. A newly available concept, email-based medical image data sharing on a global level, has become a reality.
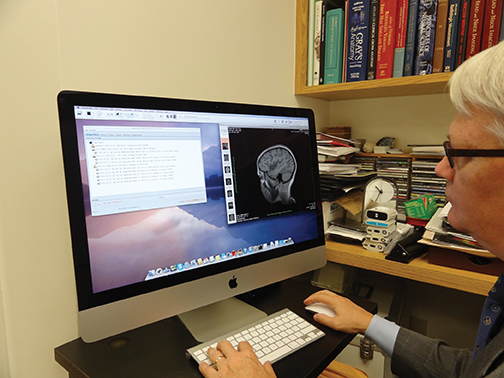
ImageInbox™ is a HIPAA-compliant, zero-footprint/zero-install application that encrypts data and securely sends medical images over anInternet connection to stakeholders (Figure 3). It provides direct image transfer between sender and receiver via email. Additionally, it manages bi-directional image workflow integration, performs MRN and accession coding, and supports CD-ROM import from outside facilities.
The first installation of ImageInbox may take place at Children’s Hospital Los Angeles (CHLA). As a primary Level 1 Trauma Center,CHLA experiences a high volume of referrals for local and international patients. One of the goals of the hospital is to make outside imaging exams available to its medical staff prior to patient arrival. CHLA is looking at several options, but believes it can accomplish this objective by connecting the referral center to its PACS via ImageInbox. “We are evaluating ImageInbox to enable referring hospitals to remotely and directly upload images into our system,” said Alberto F. Pernudi, administrative director, Department of Radiology, CHLA.
“ImageInbox is a comprehensive system that will allow transferring medical data and will integrate with the RIS and PACS workflow. It will be able to integrate with the EHR,” said Pernudi. “It is not just a radiology application – it goes beyond PACS – it touches every activity in the hospital. The faster physicians see the images, the better care we can provide to the children. I think ImageInbox will give us the ability to expand on our consultation program.”
“When transferring the data, the application recodes images for each institution and forwards those recoded images to the PACS,”indicated Stephan Erberich, director of biomedical informatics, The Saban Research Institute, Children’s Hospital Los Angeles, professor of Research Radiology, Department of Radiology, Keck School of Medicine at the University of Southern California, Los Angeles,Calif. “The radiology department wants to have the original image when calling up a prior. If there is an awkward compression or you cannot decompress the software from the CD-ROM, often you need the raw data of the medical image with full diagnostic quality.”
As for security concerns, the application ensures HIPAA compliance by creating a trust fabric that authenticates provider authorization to access the data. According Pernudi, a point-to-point encrypted email transfer is more secure than burning the images to CDs and giving them to patients. “The referring facility is sending the image directly to the hospitals. The data access will expire if the patient doesn’t pick itup within a set timeframe. This is a more secure way of communicating with hospitals in the community,” said Pernudi.
Another Internet-based image transfer solution is BEAM™ technology from OneMedNet. This solution makes it possible to send studies from Horizon Medical Imaging, McKesson’s PACS, instantaneously from hospital to hospital. In Hawaii, where many patients need to be airlifted to hospitals, clinicians at trauma centers can get a head start if they can review medical records in advance. The Queen’s MedicalCenter, Hawaii’s most advanced trauma hospital, implemented BEAM to overcome delays and today receives imaging studies well in advance of patient transfer.
Conclusion
As we envision the image-exchange of the future, radiologists, referring physicians, and patients will have access to health records for which they are authorized. Whether it’s achieved via the VNA track or the more familiar PACS enterprise-archive, image-data sharing across hospitals, private practices, and HIEs is critical from a patient-care perspective. Without it, providers will continue to merely treat one series of images at a time, and not the patient as a whole.6
REFERENCES
- 2014 Proposed Medicare Physician Fee Schedule Payment Cuts to Radiology and Radiation Oncology Services. ACR. http://www.acr.org/News-Publications/News/NewsArticles/2013/Economics/20130725-Medicare-Physician-Fee-Schedule-Payment-Cuts. Updated July 24, 2013. Accessed October 14, 2013.
- Benefits of image-enabling the EHR. MU2 implications for hospitals, imaging providers and EHR vendors. A Merge Healthcare Whitepaper. Accessed October 7, 2013.
- Enterprise imaging 2012: Provider’s strategies and insights. KLAS. 2012. Accessed October 14, 2013.
- Vendor neutral archive (VNA) & picture archiving and communication system (PACS) market worth $3.48 Billion by 2018. Markets and Markets. http://www.marketsandmarkets.com/PressReleases/vendor-neutral-archive-VNA-PACS.asp. Updated October 8, 2013. Accessed October 14, 2013.
- Ryan W. 5 Forces driving hospital consolidation. Stratasan. http://www.stratasan.com/5-forces-driving-hospital-consolidation/Updated July 10, 2013. Accessed October 14,
- Shrestha RB. Enterprise imaging: Enabling true image exchange. App Rad. 2013:5:20-21. 2013.