Telemammography: Interfacing between primary physicians and experts


Dr. Paredes is the Founder and Director, The Ellen Shaw de Paredes Institute for Women's Imaging, Glen Allen, VA. She is also a member of the editorial board of this journal. Mr. Lopez is President and Chief Information Officer and Mr. Strickland is Chief Executive Officer, Strategic Solutions of Virginia, Richmond, VA. Dr. Grizzard is a Partner and Dr. Roberts is a Partner, Riverview Physicians for Women, Colonial Heights, VA. Dr. Zedler is the Clinical Trials Division Leader, and Dr. Stout is a Partner, Virginia Women's Center, Richmond, VA.
Breast cancer is the most common cancer in American women and the second cause of cancer deaths after lung cancer. The difference in mortality rates between breast cancer and lung cancer is related to the higher cure rate of breast cancer because of early detection. Screening mammography has been proven to be effective in reducing the mortality rate from breast cancer as shown in both clinical trials 1-3 and in service screening. 4 With current technology, the reduction in breast cancer deaths because of screening mammography is estimated to be 50% for women aged 40 to 49 years. 5
Unfortunately, many women do not undergo annual mammography, as recommended by the current guidelines. Among the barriers to undergoing routine mammography are cost, access to mammography facilities, fear of cancer detection, fear of radiation, and procrastination. 6 Geographic barriers to mammography certainly exist worldwide, and barriers also exist throughout the United States. As more mammography facilities either close or are unable to handle the volume of patients who need mammography, this problem will most likely continue to worsen.
In a study of the utilization of mammography in Kansas, where mobile mammography is also available, Engelman et al 7 found that in adjusting for age, race, and education, the odds of receiving a mammogram were slightly lower for women residing longer distances from a permanent (nonmobile unit) facility. In a study of mammograms and healthcare access among U.S. Hispanic and non-Hispanic women who were ≥40 years, Aldridge et al 8 reported that the odds of ever having a mammogram were similar among both groups of women when adjusted for age, employment status, and other demographic variables. Having a personal physician and the type of healthcare facility were found to be associated with mammography use.
One of the methods to improve access to screening mammography is the use of mobile facilities that can visit rural areas or worksites. However, in a summary of 367 mobile facilities, Debruhl et al 9 found that only 47% of the facilities are either financially profitable or able to break even.
A direct correlation exists between mammography rates and the number of facilities per 1000 square miles, 10 indicating that the screening rate depends on access. Marchick and Henson 10 also found that the percent of in situ breast cancers in black and white women was correlated with the number of mammography facilities per 10,000 women. This illustrates the importance of access to screening for the detection of breast cancer at an earlier stage.
If high-quality screening mammography is offered in primary care or gynecology offices, women can undergo their screening during the same visit as an annual Pap test, and compliance with screening mammography may be higher. The combination of full-field digital mammography (FFDM) with expert interpretation offers a unique service at the local level. This is the concept behind our Telemammography Program in Central Virginia.
Analog mammography was the technique used in the various reported screening trials that assessed breast cancer mortality reduction. 1-3 Full-field digital mammography has been shown to be superior to film-screen mammography for cancer detection 11 in women with dense breasts, in perimenopausal and premenopausal women, and in women under age 50. Digital mammography has been shown to be equivalent in cancer detection to analog mammography for older women. In general, digital technology has several important advantages, including vastly improved image archiving over hard-copy storage. Images can be transmitted over high-speed lines, which offers remote access to this technology and concentrates the interpretive aspects by radiologists in a central area. In the field of digital mammography, algorithms can be applied to the images, allowing for computer-assisted detection (CAD) of abnormalities. Another important advantage of digital mammography is that the radiation exposure is often lower 12 than that of analog mammography, in part because of the use of a harder beam with tungsten or rhodium filtration.
With digital mammography, images can be transmitted, archived, and interpreted off-site, which allows for increased access to high-quality imaging. The implementation of telemammography is challenged by the very demanding spatial resolution requirements of mammography as compared with other forms of medical imaging, because of the need to detect microcalcifications and the fine details of lesion margination. The larger size of the image data sets places significant demands on the local and wide area networks to be able to transmit the studies. 13
Telemammography has been studied using digitized film images, data compression, and transmission over phone lines. 14 Leader et al 15 described a multisite telemammography system for remote patient management by transmitting digitized images across low-level communication systems to the central site. Lou et al 16 reported a full-field direct digital mammography (FFDDM) telemammography system that incorporated telediagnosis, teleconsultation, and telemanagement. In that project, a SenoScan FFDDM system (Fischer Medical Technologies, Inc., Denver, CO) with a 54 µm 2 pixel size was used, generating an image of approximately 46 MB (4 k × 5.6 k × 2 bytes) in size.
Early papers on telemammography network architecture described transferring images over asynchronous transfer mode (ATM) networks with transmission speeds of 155 MB/sec. 17 More recently, the Swedish Breast Care Centers in Seattle, WA, 18 described the implementation of a digital mobile telemammography service with transmission via satellite. Telemammography systems using FFDM are beginning to develop, and they can offer improved image quality and cancer detection rate to greater numbers of women.
Central Virginia Telemammography Program
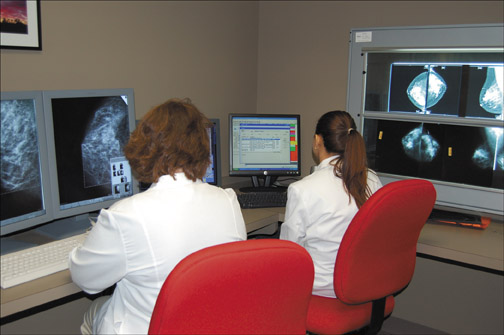
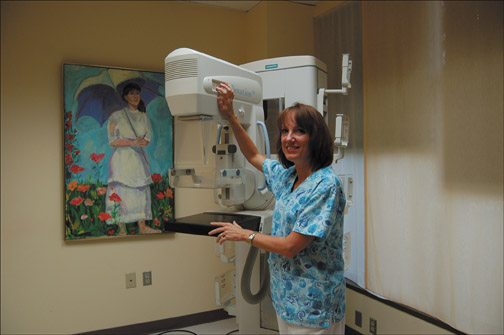
We have organized a partnership among groups of gynecologists (Riverview Physicians for Women and Virginia Women's Center), breast imagers (Paredes Institute for Women's Imaging), and a network technology group (Strategic Solutions of Virginia [SSV]) to provide expert-level telemammography services to patients in the office setting (Figure 1). High-quality FFDM is delivered to patients at the primary-care site-the gynecology office. The technologists were trained at the breast imaging practice, and their work and the overall quality control is supervised by the radiologists. At all of the sites, the FFDM units are MAMMOMAT Novation DR (Siemens Medical Solutions, Malvern, PA; Figure 2). The images are acquired on the digital units, checked for quality by the technologist on the acquisition workstation, and transmitted via high-speed encrypted data circuits through the archive at SSV to the breast imagers.
The studies are interpreted by experts in breast imaging. The interpretation is performed by soft copy on workstations, incorporating CAD (ImageChecker, R2 Technology, Inc., Santa Clara, CA) as well. Patients who need breast ultrasound, diagnostic mammography, and percutaneous biopsy are referred primarily to the breast imaging practice, so continuity of care is achieved. In addition, there is improved tracing for quality assurance within this network. In the more remote gynecology facility, online diagnostic mammograms are also occasionally directed by the radiologist from the central location and performed remotely.
Network and communications
In order for studies to be sent for remote interpretation, it is imperative that the network is secure, redundant, efficient, and resiliant. These qualities are required for a medical-grade network. SSV designed this network architecture to best meet these requirements.
For new patients, any prior outside mammograms are sent by courier to the breast imaging facility. For return patients, the prior study is already in the archive and is incorporated with the new study for interpretation. An average study size is 100 to 115 MB. Our minimum WAN (wide area network) transmission speed is 1.5 Mbps using a T1 line. Currently, a study takes approximately 10 minutes to transmit or receive from the remote sites to the centralized archive. The breast imaging practice is considered the host site and has redundant high-speed connectivity to the centralized archive (10 Mbps). This enables us to receive and transmit studies as well as other data very quickly.
High-speed connectivity is not all that is required to facilitate high-speed image transfer. By performing in-depth analysis using various network metric tools and protocol analyzers, SSV developed a formula to calculate the minimum bandwidth requirements for a practice participating in the telemammography project. The formula is based on variables such as study size, quantity of studies, and frequency of transmission. The transmission of 10 to 15 digital mammography examinations a day (with an average size of 115 MB) needs a minimum of a T1 (1.5 MB) line; 15 to 30 studies a day should use a minimum circuit with a bandwidth no less than 3 MB. In this network architecture, no image compression is employed in study transmission.
These circuits terminate in a Tier 1 carrier-class data center (Figure 3). The facility itself is fully redundant with many layers of redundancy. These layers surround the innermost layer known as the "core," where devices such as the DICOM archive and radiology information system (RIS) or mammography database reside. Studies are centrally archived at this data center with an off-site archive that is fully replicated. In addition, services such as secure remote access are provided to allow participating physicians access to the RIS.
Reporting
Reports are generated by the breast imagers using a computerized database and reporting system (MagView, Burtonsville, MD). The radiologist opens the database of the remote facility from the central location, keys in the findings, and signs the report; the letter for the patient and report are printed at the gynecology office. This process allows for interpretation on the same day or the next day, and the patient letter and radiology report are generated immediately (Figure 4). The referring physician has access to the printed report and is able to communicate the results to the patient and to discuss any further treatment planning.
The reporting system is also a database for patient tracking. Pathology information on biopsies performed at the radiology practice are entered remotely into the individual databases of the gynecology practices. This information is used for computing the quality assurance reports required by the Mammography Quality Standards Act (MQSA) for each of the facilities. The same database is also used to send recall letters to patients when they are due for follow-up studies.
Conclusion
Our telemammography system incorporates image acquisition, processing, transmission, display, and interpretation over a network that allows for near- real-time patient management remotely. While the majority of cases are screening mammograms, occasional diagnostic mammograms are performed remotely and directed by the radiologist from the breast imaging center. This program has extended the ability of experts in breast imaging to provide care to a greater number of patients. This also has improved the level of care to women in areas where both the technology and the expertise have not been available. It is hoped that the improved access to expert healthcare and the state-of-the-art technology for screening mammography that this program offers women will translate to fewer cancer deaths through the detection of more early breast cancers.
Full-field digital mammography offers numerous advantages, including improved cancer detectability, the incorporation of CAD, improved archiving, and the option of telemammography. Telemammography allows for access to expert radiologic interpretation at numerous remote sites. Improved access to mammography and utilization of screening can be achieved by partnerships between primary care physicians and radiologists via telemammography. Improved efficiencies in patient care, mammography interpretation, reporting and follow-up can be achieved through these partnerships. The breast imaging practice serves as a super-center, interpreting screenings off-site in a paperless, filmless manner, and serves as a referral center for the diagnostic mammograms, ultrasounds, and biopsies. With increased access to and utilization of high-quality digital screening mammography, we can reduce the mortality rate from breast cancer.
Acknowledgement
The authors gratefully acknowledge the assistance of Ms. Louise Logan in the manuscript preparation.
