Spontaneous left atrial intramural hematoma with cystic degeneration
By Kowalchuk RO, Kowalchuk RM, Kaplan-List K
CASE SUMMARY
A 62-year-old female patient with no prior cardiac history presented to the emergency department with chest pain radiating from the right breast to the left breast and back, accompanied by nausea, vomiting, and fatigue. Intermittent chest and back pain had started 3 days previously, associated with dysphagia and mild shortness of breath with exertion. The patient had recently travelled to Peru, Antarctica, Berlin, Prague, and Northern California.
On admission, the patient was tachycardic with mild hypotension. EKG demonstrated junctional tachycardia to 119, with ST segment depression in V4, V5 and V6. Laboratory workup showed leukocytosis of 19.3. Troponin (1.01), BNP (703), and CRP (176.2) were elevated. Coagulation parameters and liver function tests were normal. After developing atrial fibrillation on hospital day 4, the patient underwent open heart surgery which confirmed the mass filling almost the entire left atrium. After aspiration, the left atrium and atrial septum were relined with bovine pericardium. Differential diagnostic considerations included echinococcal cyst, fibrosarcoma, cystic myxoma, infected thrombus, or teratoma. Stains for bacteria and fungi were both negative. No histopathologic feature of hydatid cyst or myxoma was identified.
IMAGING FINDINGS
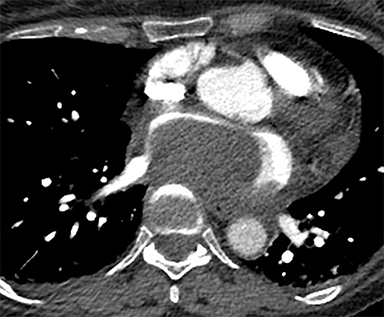
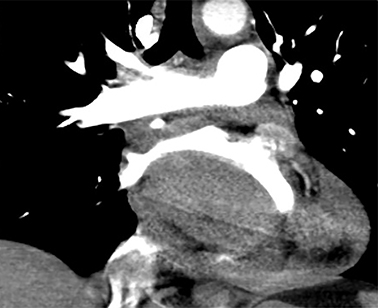
Chest CT evaluation for pulmonary embolism showed a 4.2 × 7.0 × 4.8 cm hyperdense (67 HU) mass along the posteroinferior left atrium (Figure 1). Mass effect was seen on the adjacent IVC, right atrium, and esophagus. There was a small pericardial effusion.
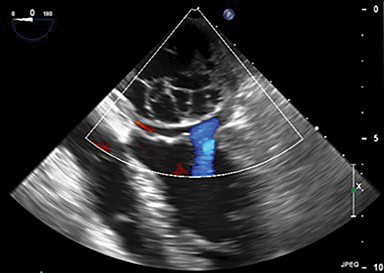
Transthoracic/ transesophageal echocardiograms demonstrated a 4.5 cm multiloculated, well-encapsulated cystic mass lesion in the left atrium attached to the interatrial septum and left atrial roof (Figure 2). There was normal appearance of the mitral valve leaflets and trivial mitral regurgitation. No flow was detected within the mass.
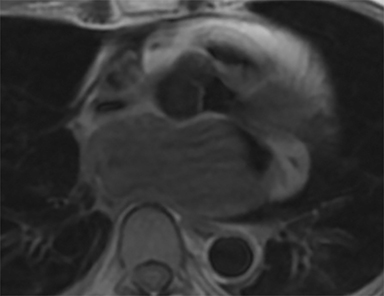
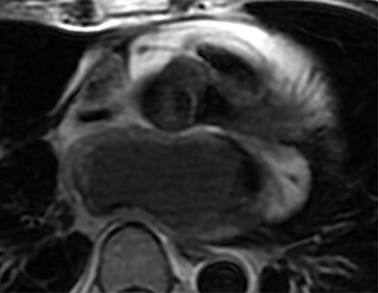
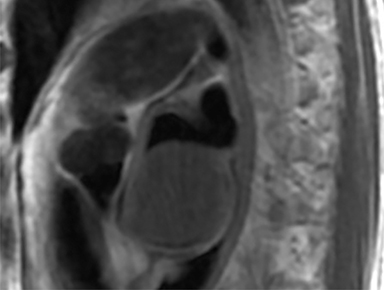
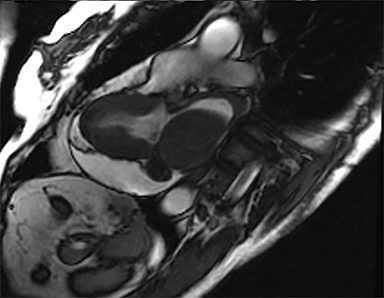
Cardiac MRI confirmed a large, smoothly marginated 4.2 × 7.0 × 4.8 cm left atrial mass related to the posteroinferior left atrial wall adjacent to the interatrial septum (Figure 3). The mass was not attached to the mitral valve. No extension of the mass was seen beyond the confines of the left atrium. The mass had slightly heterogeneous signal intensity, which was moderately hyperintense on T1-weighted imaging and moderately hypointense on T2-weighted imaging. The pulmonary veins were not obstructed. The left atrial lumen was severely narrowed with turbulent flow on cine images. The mass compressed the IVC/right atrial junction with resultant acute angulation and markedly turbulent flow within the IVC and the right atrium.
DIAGNOSIS
Spontaneous left atrial intramural hematoma with cystic degeneration
DISCUSSION
Spontaneous intramural left atrial hematomas are rare, with only 7 cases found in the literature. Reported causes of left atrial hematomas include trauma, coagulation disorders, infection, iatrogenic causes (eg, invasive intervention), mitral annular calcification, and systemic amyloidosis. In 2 of the 7 cases, the hematoma was associated with mitral valve calcification.1-2 Of the 5 remaining cases, one was associated with systemic immunocyte-derived (AL) amyloidosis in the setting of oral anticoagulation,3 another involved heparin administration,4 and a third was diagnosed after the use of CPR.5 Only 2 cases in addition to this report have no obvious cause and may be considered truly idiopathic.6-7
The workup of “spontaneous” left atrial hematoma includes echocardiography, which effectively identifies the lesion’s location and the hemodynamic status of the pulmonary vasculature; however, the appearance of a “cystic mass” may be misleading. Further characterization may be difficult due to lesion size and limited acoustic window. In our instance, workup continued with MRI, which provided excellent soft tissue characterization and three-dimensional visualization of the lesion. In 2 of the 7 previously discussed cases, MRI suggested the diagnosis of left atrial hematoma1,6 while in a third, it characterized the cystic mass as containing hematic content.7
In our patient, an echocardiogram performed 3 months after the surgery was normal.
CONCLUSION
While rare, spontaneous intramural atrial hematoma should be included in the differential diagnosis of “cystic atrial mass” on echocardiography. Echocardiography, CT, and MRI provide complementary information regarding cardiac masses, but the use of MRI may prove particularly beneficial in characterizing atrial hematomas.
REFERENCES
- Gual-Capllonch F, et al. Left atrial intramural haematoma associated with mitral annular calcification. European Journal of Echocardiography. 2009;11(5): E18-E18.
- Schecter, SO, et al. Intramural left atrial hematoma complicating mitral annular calcification. American heart journal. 1996; 132(2): 455-457.
- Watanabe, Ko, et al. Spontaneous intramural left atrial hematoma associated with systemic amyloidosis. The Annals of thoracic surgery. 2001; 72(6): 2132-2134.
- Shaikh N, et al. Spontaneous intramural atrial hematoma presenting as a left atrial mass. Journal of the American Society of Echocardiography.1999; 12(12): 1101-1103.
- BahnacyY, et al. Posterior left atrial wall hematoma mimicking cystic intracavitary atrial mass. Echocardiography.2010; 27(9).
- Álvarez J.et al. Diagnosis by magnetic resonance imaging of a case of intramural left atrial hematoma. Revista espanola de cardiologia. 2002; 55(8): 872-874.
- Jiménez JF, Delgado J, Rufilanchas J, and Pajuelo CG. Gómez. Spontaneous left atrial haematoma. International journal of cardiology. 1991; 31(3): 353-356.
Prepared by Roman O. Kowalchuk while a student at the University of Virginia School of Medicine, Charlottesville, VA; Dr. Roman M. Kowalchuk while at the Department of Imaging Sciences, University of Rochester School of Medicine, Rochester, NY; and Dr. Kaplan-List while at Rochester General Hospital, Rochester, NY.
