Benign pilomatricoma of the breast
Images

CASE SUMMARY
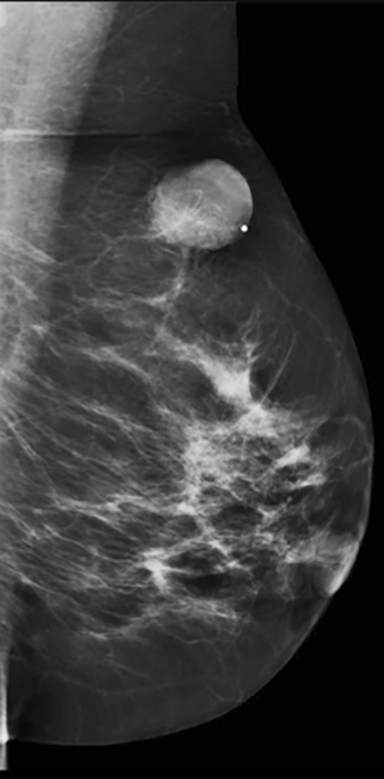
A 56-year-old woman presented to the breast imaging center with a several-month history of an enlarging, superficial, firm and non-tender palpable lump in the left breast at 12:00 (Figure 1). The patient was post-menopausal, had no personal history of any type of cancer, and had no family history of breast cancer. Diagnostic mammography and breast ultrasound were performed for further evaluation of the palpable lump.
IMAGING FINDINGS
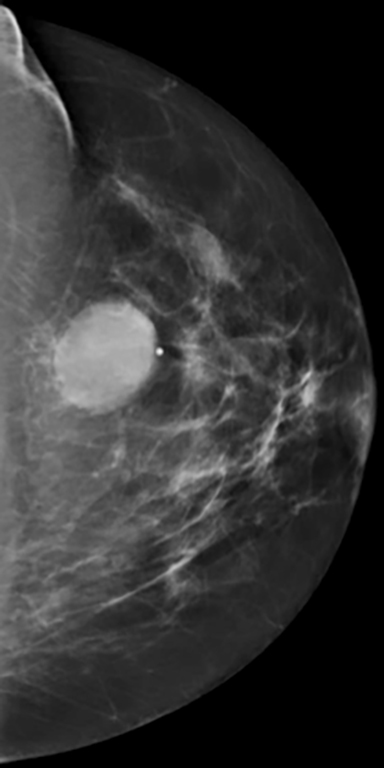
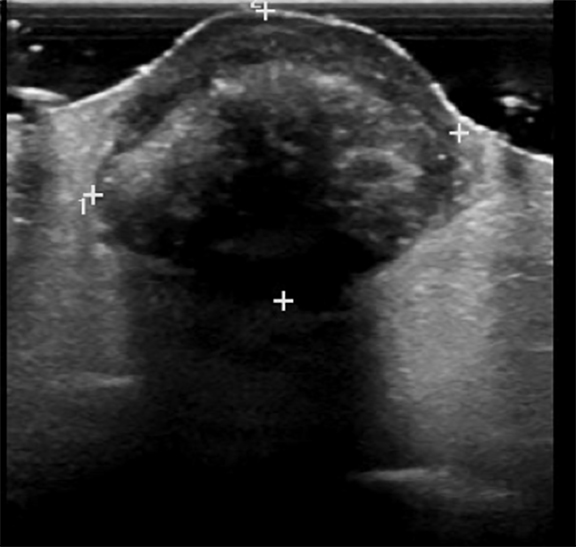
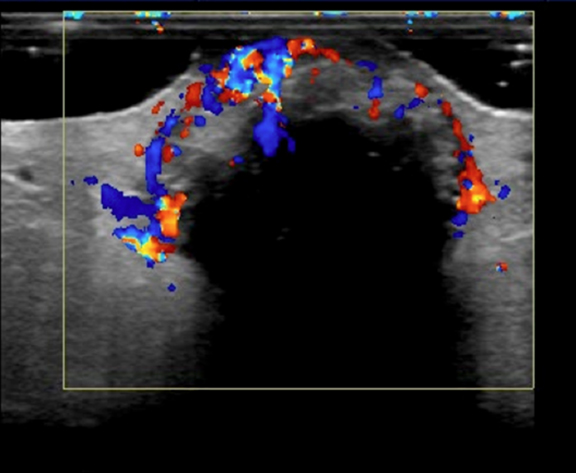
Mammography in the craniocaudad and mediolateral oblique planes demonstrated a well-circumscribed, equal-density oval mass measuring approximately 2.5 cm at 12:00 in the left breast at the site of the palpable lump indicated by a metallic BB marker (Figure 2). Ultrasound revealed a circumscribed heterogeneous dermal mass with posterior acoustic shadowing and marked peripheral color flow measuring 2.6 cm. There was an abrupt interface with the normal surrounding tissue, and there was no associated skin thickening or subcutaneous edema (Figure 3). An ultrasound-guided biopsy was not performed due to the marked vascularity associated with the lesion. Rather, surgical excisional biopsy was recommended and subsequently performed. Final pathology confirmed a pilomatricoma with no associated atypia or malignancy.
DIAGNOSIS
Benign pilomatricoma of the breast
DISCUSSION
Pilomatricoma (PM) is a rare but most-often benign skin appendage tumor of hair matrix origin. Malherbe and Chenatais first described the tumor in 1880 as a “calcified epithelioma of Malherbe” from sebaceous glands, but in 1961, Forbis and Helwig proved that the tumor originates from the hair matrix. It typically presents as a superficial, firm, solitary, slow-growing and painless mass in the deep dermis or subcutaneous tissues. The skin overlying a PM can have a normal appearance, or have a bluish-red discoloration, and it may have ulceration.1,2,3 Up to 75% of PMs possess active mutations of the beta-catenin gene, which is a signaling protein involved in the development of the pilous follicles.1,4
Pilomatricomas are the most common hair follicle tumor, typically measuring between 3-30 mm in diameter, and presenting on the head, neck or upper extremities.4 Location in the breast is considered rare, and due to clinical and imaging features, it can be misdiagnosed as a breast neoplasm. Lesions have never been reported on the palms or soles, presumably because these sites lack hair-bearing skin.5 They can occur at any age, but are most commonly seen in children and young adults, and again after age 60. Most studies demonstrate a female preponderance.1,2,3 Multiple lesions are reportedly present in 2-10% of cases, and are associated with Gardner Syndrome, Turner Syndrome, myotonic dystrophy and sarcoidosis.5
Clinical variants include extruding lesions, ulcerative lesions, multiple eruptive cases, familial cases, superficial PM presenting as a cutaneous horn, bullous PM, and giant PM. 4 Lesions larger than 5.0 cm are considered “giant” PMs, and pain and tenderness may be associated symptoms.1 PMs may be confused clinically with hemangiomas and neurofibromas. The differential diagnosis is broad, including epidermoid cyst, sarcoma, calcified giant hemangioma, giant dermatofibroma, atypical mycobacterial infection, ossifying hematoma, giant cell tumor, foreign body reaction, cutaneous lymphoma, cutaneous metastasis and basal cell carcinoma.1,2,5
Malignant pilomatricoma (MPM) is the rare malignant counterpart, and as of 2014, only 80 cases were reported in the literature.6 MPM may arise de novo, from a previously excised benign PM, or within a large benign PM that has been present for a long time.2,4 The MPM is a locally aggressive tumor seen in those over 40 years old.1, 6 It tends to recur, but has low potential for systemic metastases. It can be impossible to distinguish benign from malignant pilomatriomas clinically and through imaging, as the MPM normally has a very similar presentation.6
The role and importance of imaging is debatable, given the broad differential of the lesion. Plain film radiography may demonstrate calcifications. Ultrasound typically shows a well-defined hyperechoic or isoechoic mass with a hypoechoic rim and posterior acoustic shadowing. In other parts of the body other than the breast, CT and MRI may delineate the depth of a lesion. CT demonstrates a well-defined mass of soft tissue density with mild-to-moderate enhancement with contrast, and MRI shows a homogenous mass with intermediate signal intensity on T1, and inhomogeneous intermediate signal intensity on T2.5
If fine-needle aspiration is performed, the diagnosis of PM may be made only if all major components of PM are present in the aspirate, including calcium deposition, basaloid cells and keratinized ghost or shadow cells. Previous studies show that the diagnostic accuracy rate of preoperatively diagnosing PM ranges from 0-30%, and histopathologic analysis is therefore necessary for a final diagnosis.1,2,5 Histopathology generally demonstrates irregular islands of epithelial cells with biphasic architecture of central ghost cells and varying amounts of basaloid cells in the periphery. There is an increased ratio of ghost cells to basaloid cells with older PM because basaloid cells are keratinized to form ghost cells over time.5
Treatment of benign PM involves nonaggressive but complete excision of the lesion, as spontaneous regression has never been reported. Adherence to deep structures is also not reported in the setting of benign PM. The risk of recurrence is approximately 4%, but it is lowest when complete excision is successful. If a recurrence ensues, then a wider excision and more detailed histopathologic analysis are required.1, 5
CONCLUSION
Pilomatricoma is an uncommon, most-often benign hair matrix tumor rarely diagnosed in the breast. The malignant counterpart has a similar clinical and imaging presentation, and it is therefore difficult to distinguish between benign and malignant disease without complete histopathologic analysis. Treatment involves complete surgical excision of the lesion, and recurrence of benign PM is rare in this setting.
REFERENCES
- Souto MP, Medeiros Matsushita M, Medeiros Matsushita G, Souto LR. An unusual presentation of giant pilomatrixoma in an adult patient. J Derm Case Rep. 2013; 7:56-59.
- Sinhasan SP, Jadhav CR, Bhat RV, Amaranathan A. Pilomatrixoma – Presented as hypopigmented tender nodule: diagnosed by FNAC: A case report with review of literature. Indian J Derm. 2013; 58:405.
- Nori J, Abdulcadir D, Giannotti E, Calabrese M. Pilomatrixoma of the breast, a rare lesion simulating breast cancer: a case report. J Radiol Case Reports. 2013; 7:43-50.
- Belliappa P, Umashankar N, Raveendra L. Bullous pilomatricoma: A rare variant resembling bouncy ball. Int J Trichology. 2013; 5:32-34.
- Whittemore K, Cohen M. Imaging and review of a large pre-auricular pilomatrixoma in a child. World J of Rad. 2012; 4:228-230.
- Allaoui M, Hubert E, Michels JJ. Malignant Pilomatricoma: Two new observations and review of the relevant literature. Turkish J Path. 2014; 30:66-68.
Citation
. Benign pilomatricoma of the breast. Appl Radiol.
April 7, 2015