Cosmetic breast augmentation: A review of mammographic findings
Images



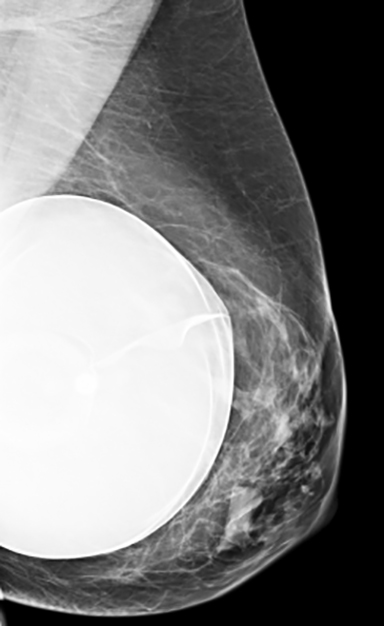
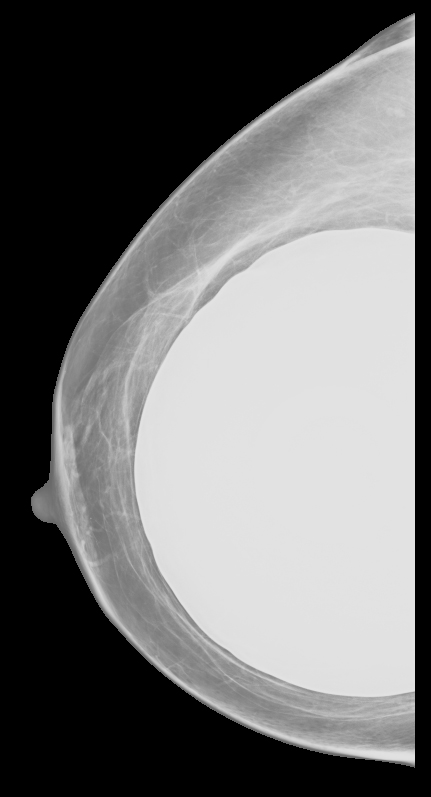
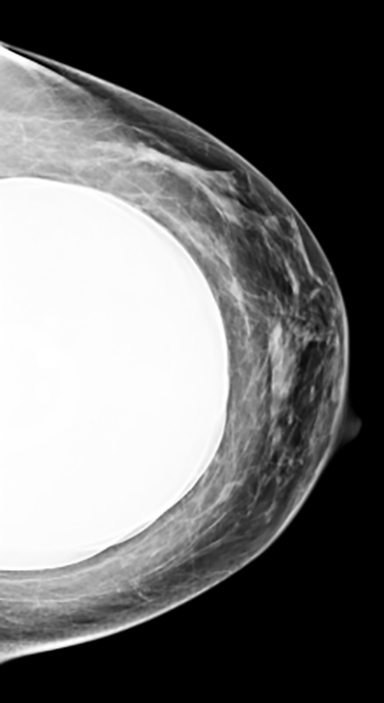
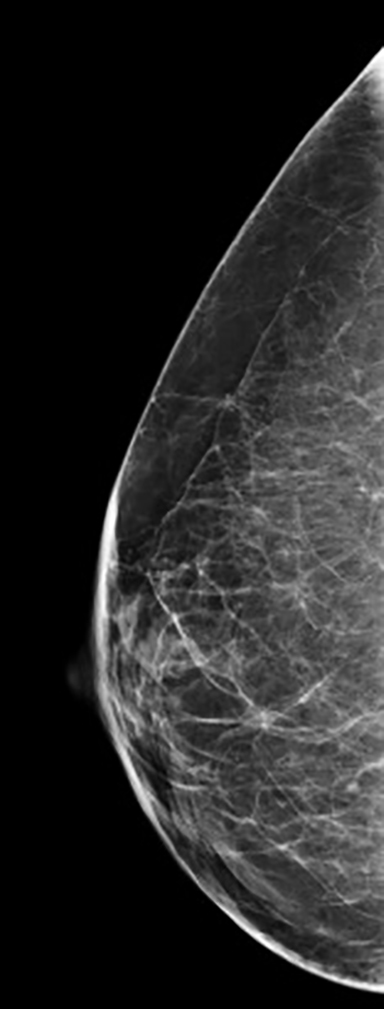
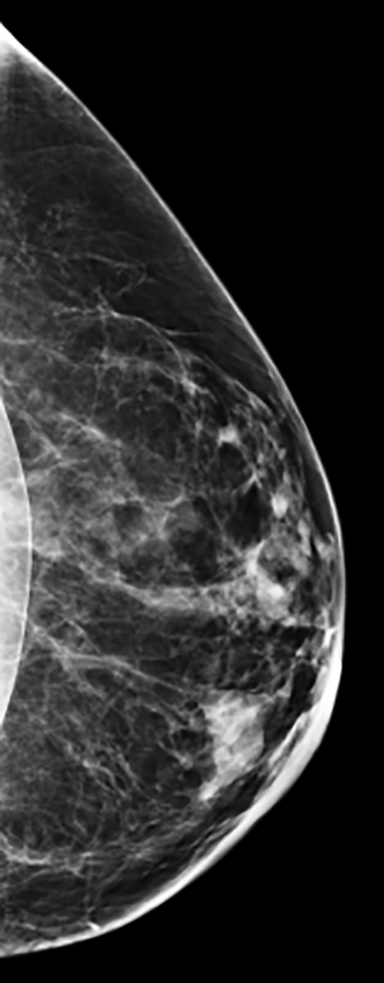



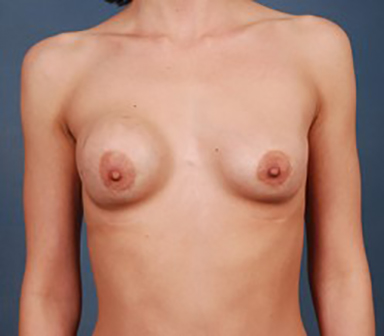

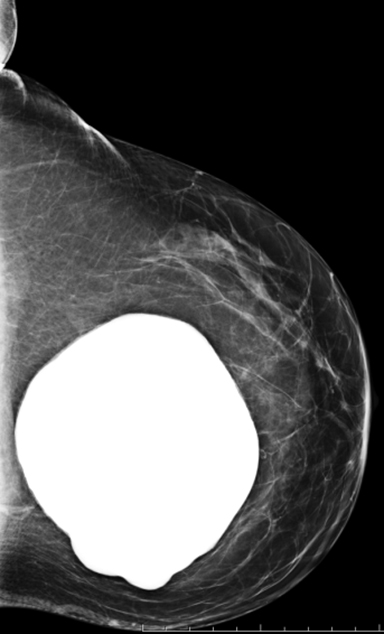
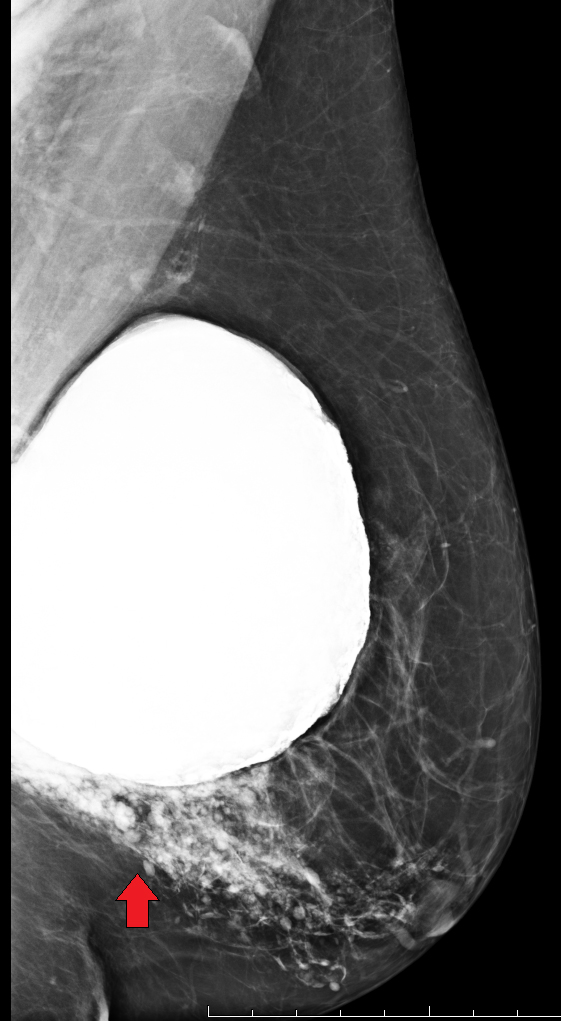
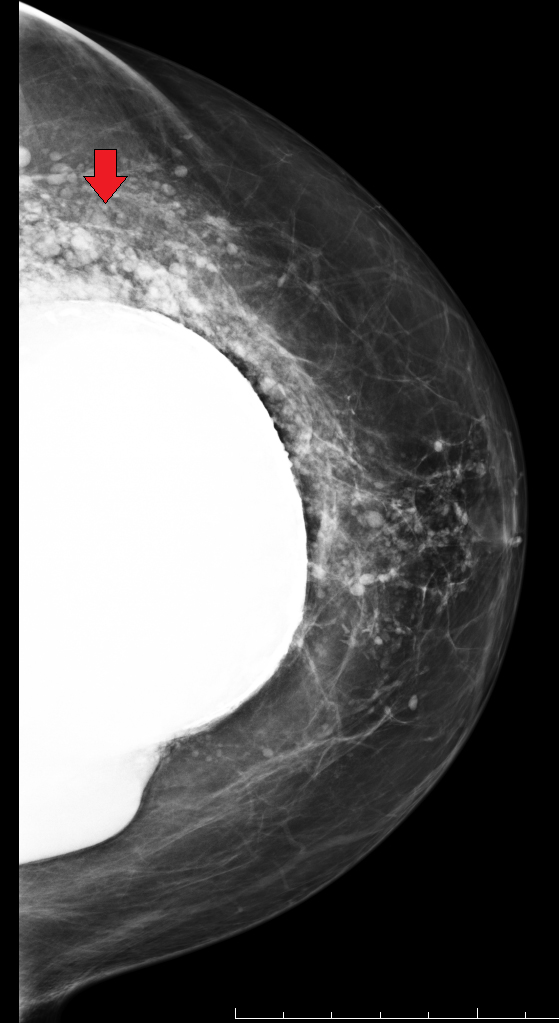
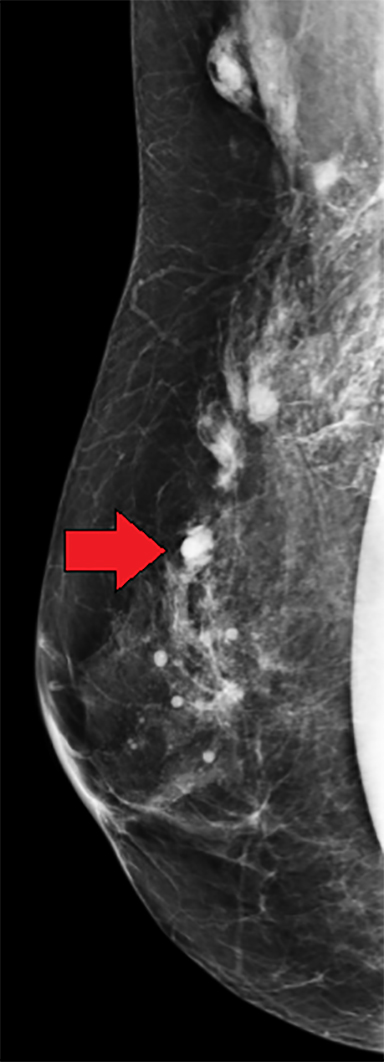
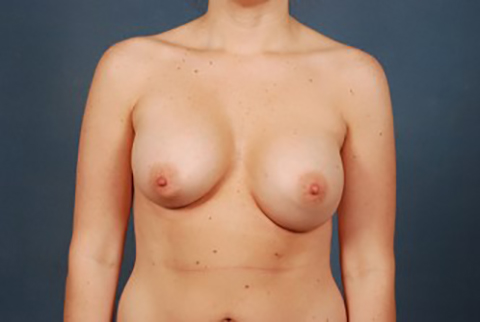


Elective cosmetic surgery, already popular in the United States, is on the rise. This includes cosmetic breast augmentation, with women electing to undergo this surgery for personal reasons such as a desire to increase or change breast shape or size, or to restore breast fullness due to weight changes and/or pregnancy (Figure 1). Breast augmentation is the most common cosmetic surgery performed in the United States, and it continues to increase.1 As more women undergo breast augmentation, the visualization of implants during mammography will also increase. For radiologists who interpret either screening or diagnostic mammograms, an understanding of the diverse mammographic manifestations of breast augmentation can help produce a precise, accurate and relevant report that can help to provide optimal patient care.
Implant-specific mammography
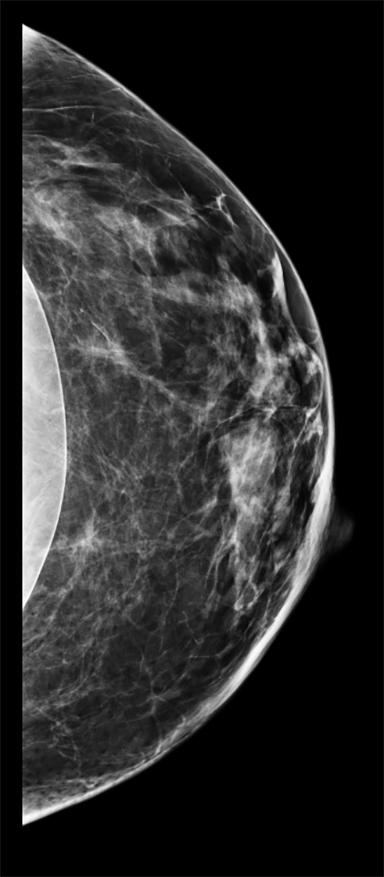
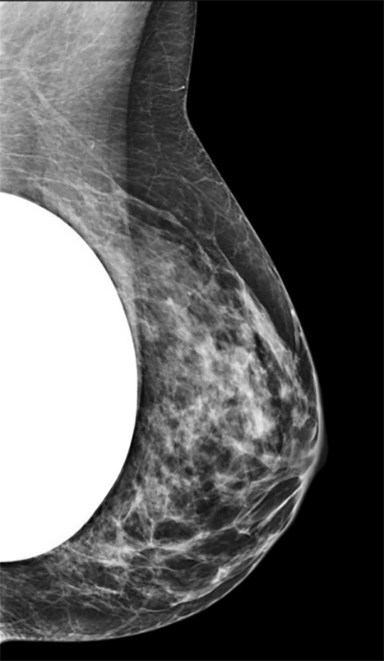
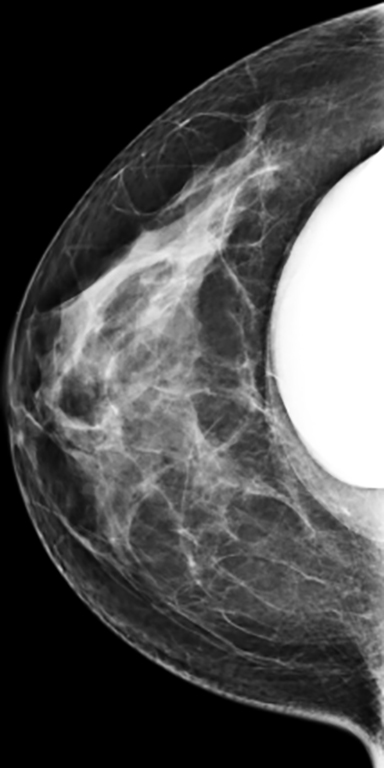
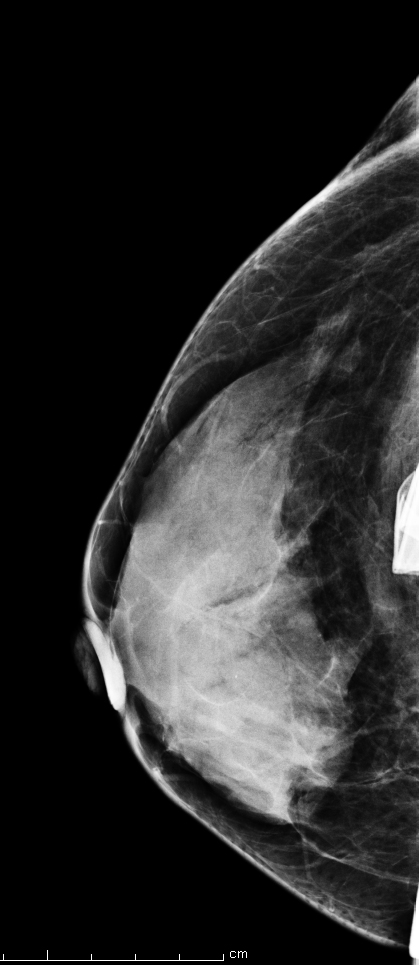
Implants are not a contraindication for mammography. Centers that routinely perform mammograms often provide these women with routine full field routine CC (cranio-caudal) and MLO (mediolateral oblique) views, as well as additional “implant displaced” CC and MLO views (Figure 2). These implant-displaced views are obtained for increased compression of glandular tissue and were first described by Dr. Eklund in 1988. The technique of “implant displaced” or “Eklund” views involves posterior and superior displacement of the implant to flatten it against the chest wall.2
Implant types and appearances
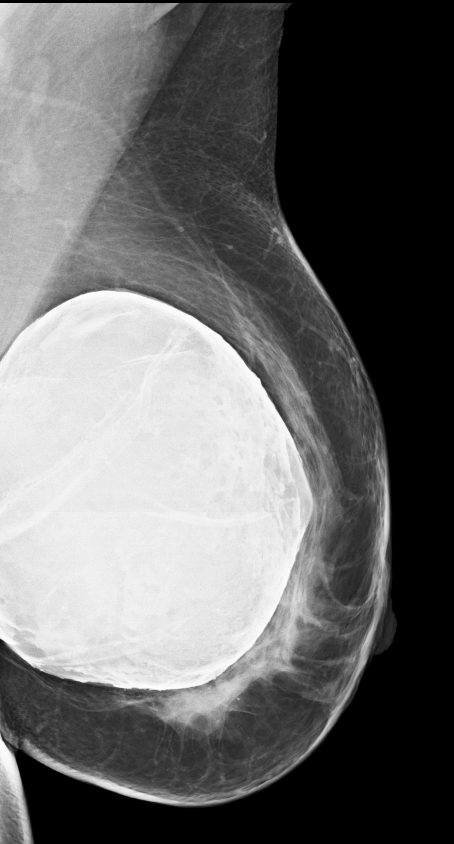
Implants are identified on a mammogram by visualizing a round or oval foreign body within the breast. Implants consist of an outer elastomer shell with an internal lumen that can be filled with different types of material. The most common types of implants are single-lumen silicone and single-lumen saline implants. There are other less common variations of dual-lumen implants containing an inner and outer shell, with either shell containing silicone or saline. In 2013 silicone was the most common type of implant placed, followed by saline.1
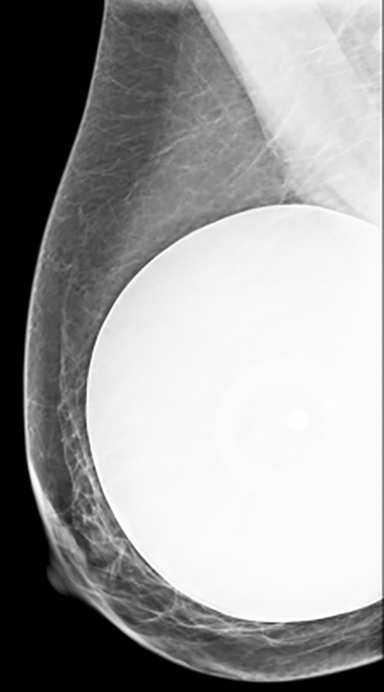
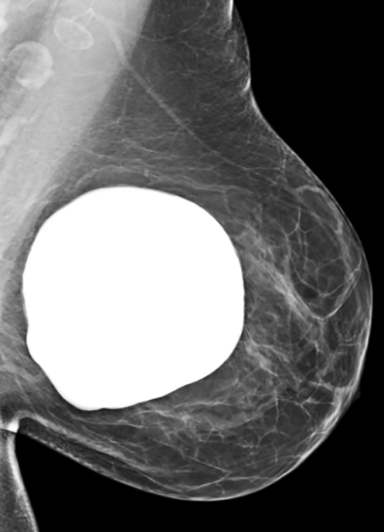
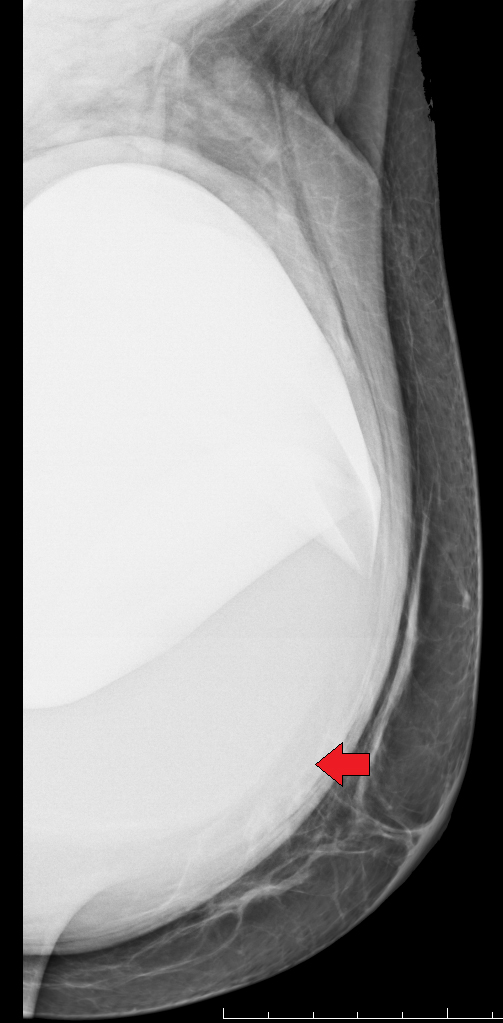
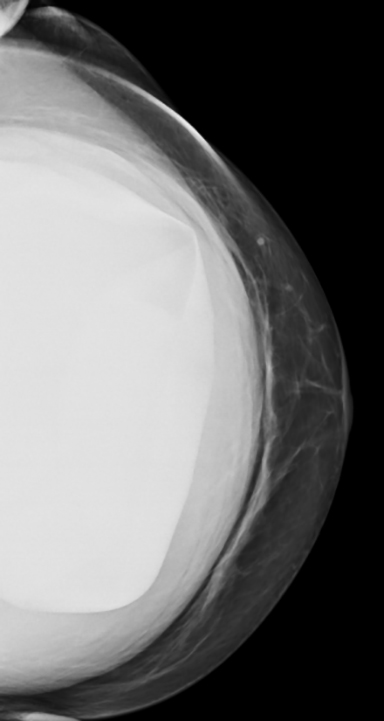
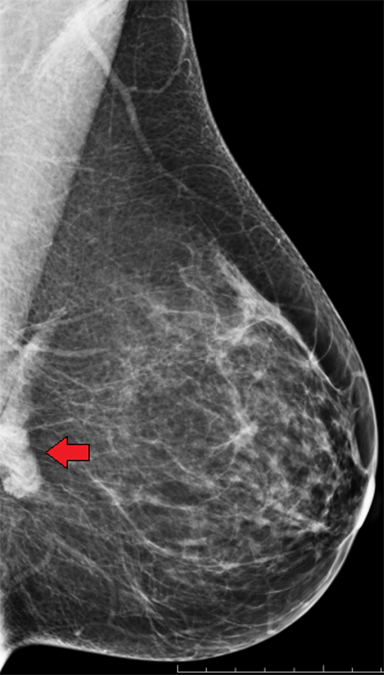
Distinguishing a saline implant from a silicone implant on a mammogram can be accomplished by two relatively typical characteristics. Saline implants contain a valve that is used to inflate the implant at surgical placement. This valve can be identified on a mammogram, as can the normal folds of the outer implant envelope.3 Silicone implants do not contain a valve, as they are placed in full expanded shape during surgery. The second characteristic to differentiate these two types of implants is their density. Saline implants are the same density as water. Silicone implants are composed of higher-density material that, despite window and leveling, do not readily change in appearance without discernment of folds (Figure 3). Dual-lumen implants may be seen as an inner lumen composed of the higher-density silicone surrounded by the outer lumen of saline.3
Implant placement
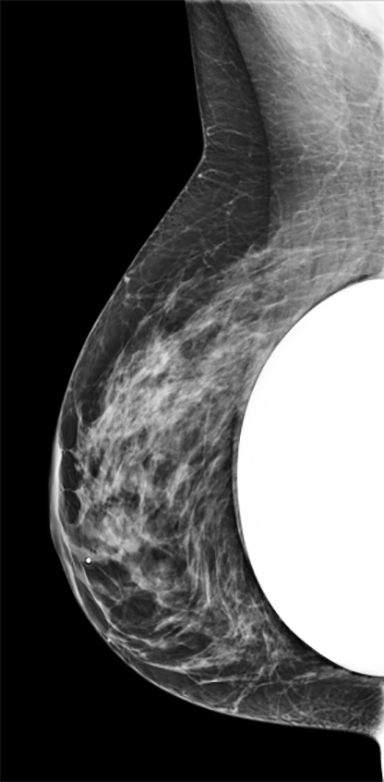
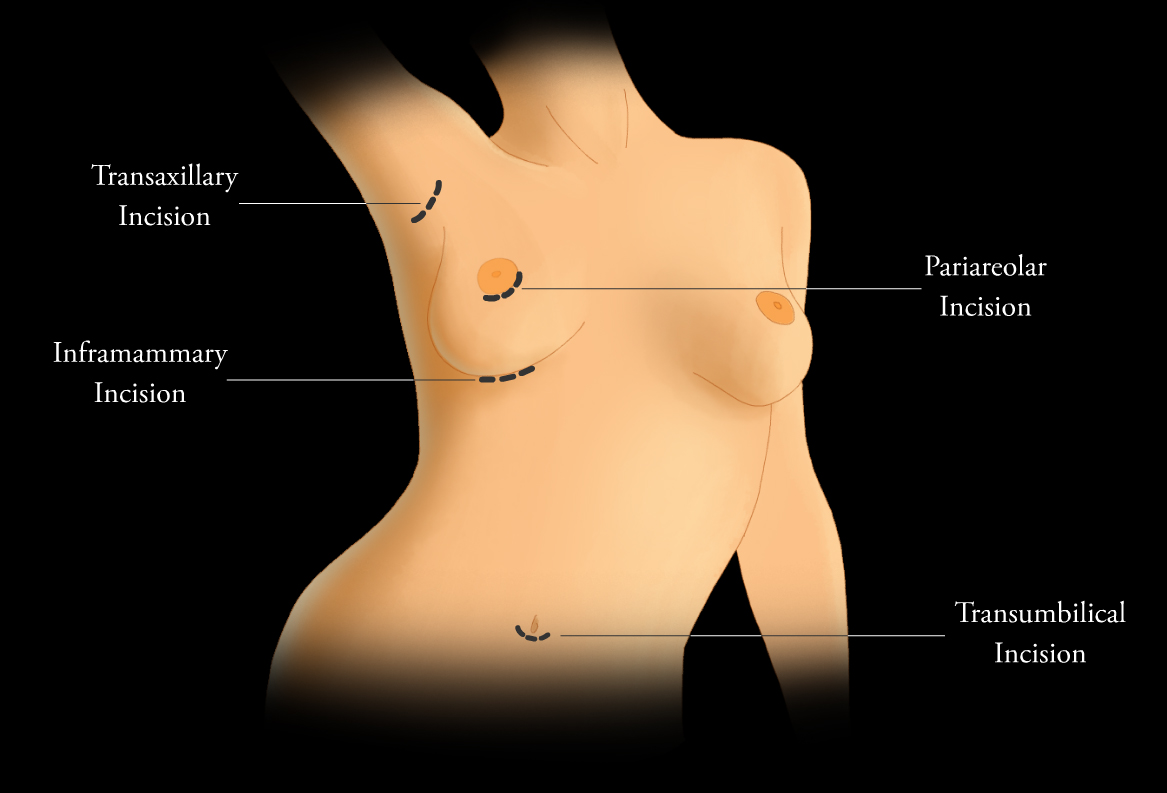
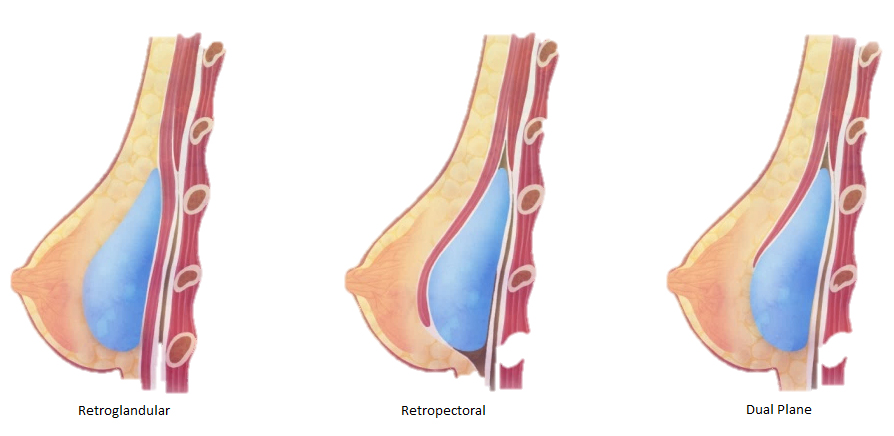
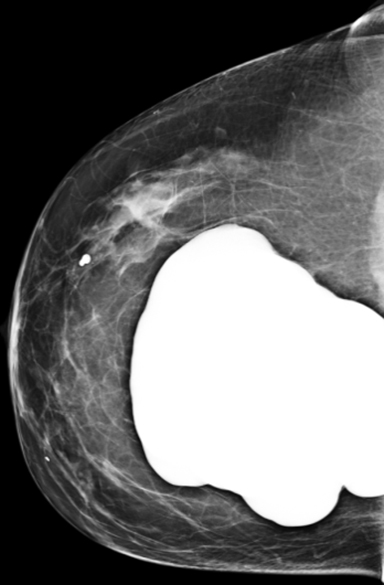
Surgeons may insert implants through several different incision sites (Figure 4). Where the implant is placed and positioned is called the “implant pocket.” Implant position is the location of the implant in relation to the pectoralis major muscle (Figure 5). The choice of incision site, implant type and position is driven by the size and type of implant, patient anatomy and patient-surgeon preference.4 Implants placed anterior to the pectoralis major are described as subglandular or retroglandular——behind most of the fibroglandular tissue in the breast but anterior to the pectoralis muscle. Implants placed posterior to the pectoralis major muscle are described as subpectoral or retropectoral.3 Discerning the implant position on mammography is often achieved on the non-implant displaced MLO view. On this view, both pectoralis major and the implant are seen, thereby most often discerning the location of the implant as related to the muscle. Implants placed in a retroglandular location demonstrate an acute angle to the inferior margin of pectoralis major. Implants placed in a retropectoral location demonstrate an obtuse angle to the inferior margin of the pectoralis major (Figure 3). Subpectoral implants are generally not entirely covered by the pectoralis major muscle, with only the superior portion of the implant covered by muscle. An additional implant positioning term is “dual plane,” a surgical term that describes how much muscle is released from the breast parenchyma, from the most inferior release at the inframammary fold to the most superior release, which is at the superior extent of the areola.
Post-placement assessment
Whether silicone or saline, an implant is considered normal when the outer elastomer shell is intact.5 The mammographic appearance of a normal saline or silicone implant is one with a round or oval shape, smooth regular borders and homogeneous radio-opacity. Saline implant rupture is classically a clinical diagnosis, as once the outer shell of the saline implant is breached, the saline leaks out of the lumen within hours. This quickly results in a loss of breast volume, which patients typically notice (Figure 6). Saline rupture can be diagnosed on mammography and is demonstrated by a deflated implant with multiple folds (Figure 7).3
Implants, regardless of lumen type, develop a fibrous capsule around the outer elastomer shell.6 This is normal; the body produces the capsule as it recognizes and walls off the implant as a foreign body. The surrounding fibrous capsule may or may not be discernible with mammography.3 However, being aware of the presence of this capsule is vital to understanding how silicone implants can rupture.
Implant rupture
There are 2 major types of silicone rup-ture, intracapsular and extracapsular.7 Intracapsular rupture occurs when the outer elastomer shell of the implant is breached, permitting the silicone to extrude from the shell but remain within the fibrous capsule. The elastomer shell in some way loses its integrity and leaks silicone, but since the surrounding fibrous capsule remains intact, the silicone remains contained. Since the surrounding fibrous capsule may or may not be discernible on mammography, combined with the high--density nature of silicone, intracapsular rupture is not a diagnosis that can reliably made with mammography. It has been reported that implants may be “suspicious” for intracapsular rupture based on a “distorted” appearance such as dis-homogeneous high/low density lumen and bulges, herniations or an irregular shape (Figure 8).5 However, these findings are not pathognomonic, sensitive or specific for intracapsular rupture. MRI is considered the gold standard for the diagnosis of intracapsular rupture, as it is the most sensitive exam for diagnosis of intracapsular rupture.5-7 Radiologists concerned about intracapsular rupture should consider a breast MRI implant protocol for further evaluation.
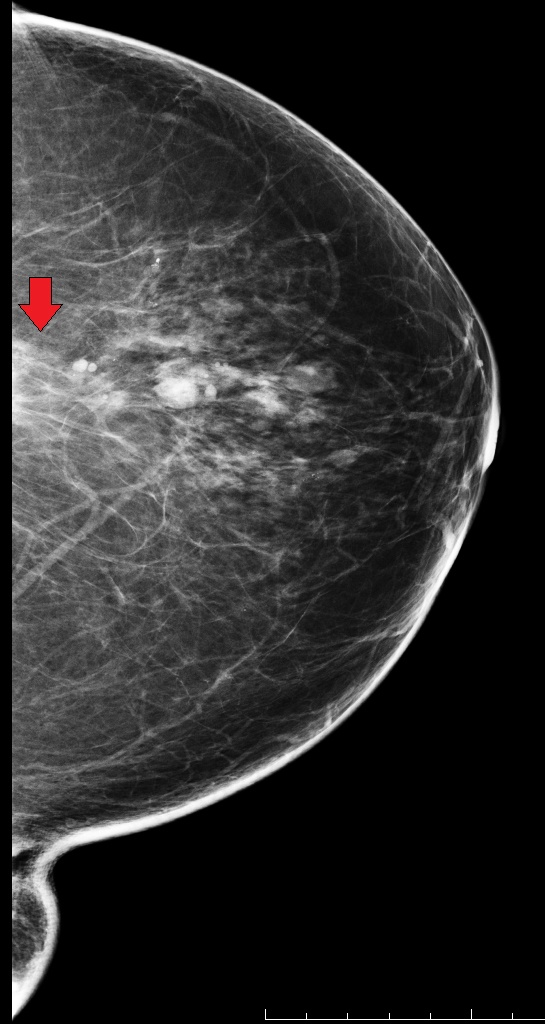
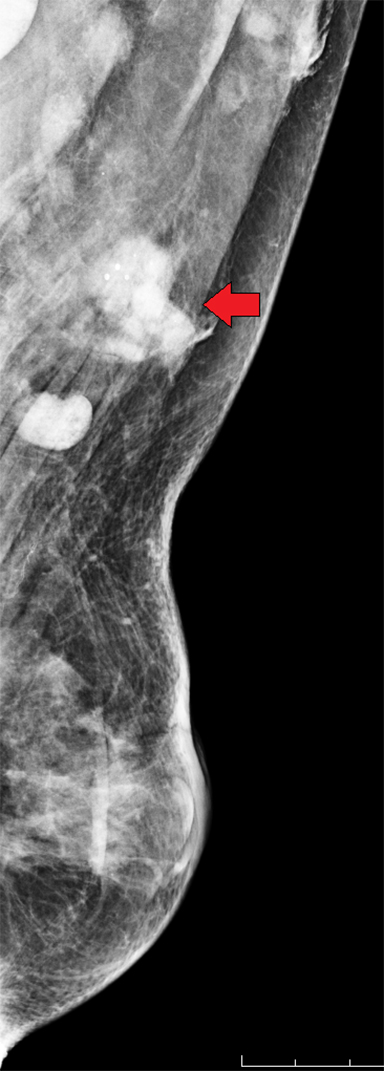
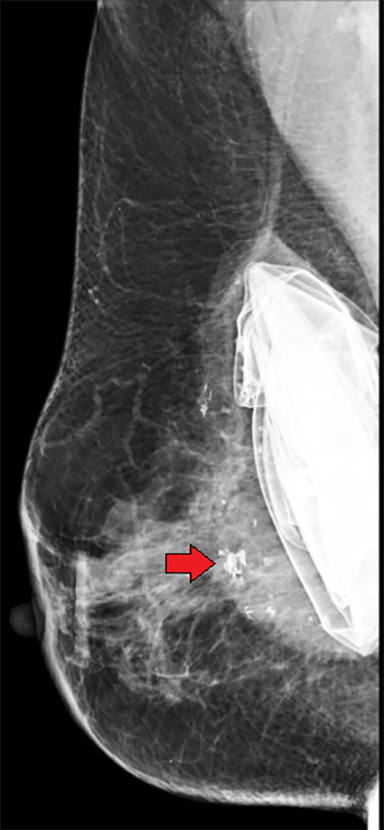
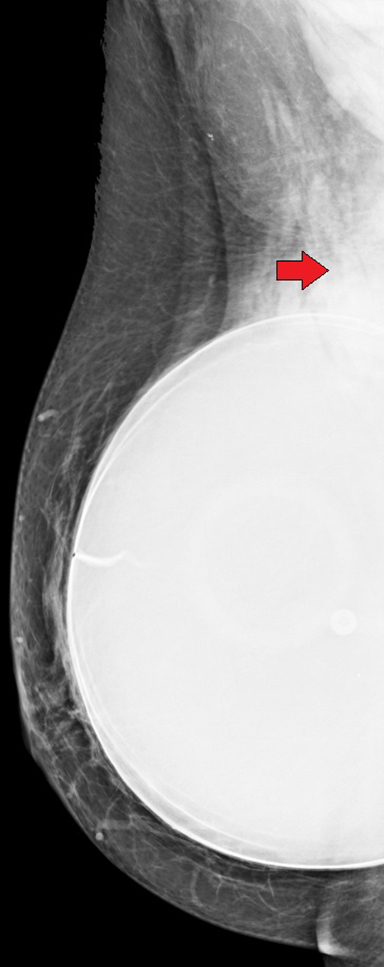
Extracapsular rupture occurs when the fibrous capsule is breached in addition to the elastomer shell.7 This results in the leakage of macroscopic silicone into the breast. Therefore, this type of rupture requires some degree of intracapsular rupture of the elastomer shell, as well as additional breach of the surrounding fibrous capsule. Mammographic signs of extracapsular rupture include extravasation of silicone outside of the implant, seen as hyperdense free silicone within the breast.5 This is often described as “peri-implant hyperdensity” (Figure 9). Free silicone may manifest as “silicone granulomas,” which are high-density masses due to the granulomatous response6 (Figure 10).. Another appearance of free silicone is “gel streaming,” in which the high-density free silicone manifests as a conic image projecting from the edge of the implant (Figure 11).8 Free silicone may be taken up by the lymphatics and result in silicone-laden lymph nodes, which materialize as abnormally high-density lymph nodes (Figure 12).9
After identifying free silicone on a mammogram, either within the breast or in a silicone-laden lymph node, in which there also an existing silicone implant, it is not always clear if the free silicone is secondary to current implant rupture. Free silicone could be present and related to a previous implant that sustained extracapsular rupture but was removed and replaced with a new, intact silicone implant. When an extracapsular ruptured silicone implant is surgically removed (explanted), the surgeon may not be able to remove all the free silicone present in the parenchymal breast tissue. Therefore, it is not always possible to determine from a mammogram if free silicone is related to the present implant or to prior implant rupture and explantation. Reviewing the patient’s surgical history can often offer explanation. Yet in the setting of reading screening mammograms in which the patient is not available for discussion and/or the history form may not have been thoroughly completed, a clear surgical history is not always known and a differential of prior versus current implant rupture may need to be considered (Figure 10).
Another phenomenon is known as a silicone “gel bleed.” This occurs in the setting of a silicone implant that is intact but there is transudation of microscopic silicone across the implant shell.3 This can occur as small quantities of low molecular weight silicone diffuse, or “bleed,” through the implant shell.10 In these cases, free silicone may bleed into the surrounding fibrous capsule, breast parenchyma and/or axillary lymph nodes.3,11
Other potential post-implant findings/complications
Apart from implant rupture, intact implants can produce other mammographic manifestations. This includes capsule calcifications and peri-implant fluid. The normal fibrous capsule surrounding the outer shell of the implant can calcify. This can occur with capsules surrounding all differing implants from saline, to silicone to dual lumen. The incidence of capsule calcifications has been reported around 16%.12 The degree of capsule calcification can vary from a focal area to a more diffuse process. The morphologic patterns of the calcifications can also vary from discrete plaques to subtle faint indistinct forms (Figure 13). Awareness of capsular calcifications is important, as they can produce mammographic false positives.10,12
Peri-implant fluid is not a common mammographic finding. Peri-implant fluid can be related to blood or more serous material. In the acute postoperative period, a collection of blood (hematoma) or fluid (seroma) around the implant produces symptoms that are most often diagnosed clinically by the plastic surgeon and treated without breast imaging. An implant may develop a seroma outside of the acute postoperative period as the implant capsule generates a foreign body reaction and inflammation, which generates a fluid collection.3 A late seroma (occurring 6 months or more after implant placement) is rare and not frequently reported in the literature.13 Peri-implant seroma can be seen as a waterdensity collection that may distort the implant shape (Figure 14). Identifying late peri-implant fluid after the acute postoperative time frame, however, has gained more attention from radiologists due to the possibility of anaplastic large cell lymphoma (ALCL), a very rare form of non-Hodgkin’s lymphoma with a reported incidence of 3 per 100 million.11,14 It is not a breast tissue cancer.11 The FDA believes that women with breast implants have a very low but increased risk of developing ALCL in the capsule surrounding the implant.15 Given the rarity of this diagnosis, however, there is a lack of clear facts regarding ALCL, including its cause, presentation or management.11,14, 16 However, ALCL should be considered in a woman presenting with a unilateral peri-implant late (at least 6 months after surgery) seroma.14-16 The FDA recommends any patient with suspicion of ALCL undergo specialty referral for additional evaluation, which may include collection of the seroma fluid for cytological evaluation.15
Capsular contraction is the most common complication of implant breast augmentation. The fibrous capsule around the implant contracts and hardens resulting in change of breast shape, breast hardening and distortion. Possible associated imaging findings may include: Inability to posterior displace the implant on Eklund view, altered implant shape such rounded, irregular, tented, and visible thick capsule.3,6, 17 Capsular contraction, however, is classically considered a clinical diagnosis. Baker grades (I-IV) are a clinical assessment of capsular contracture based on the degree of breast hardening and immobility (Figure 15).
Explantation
Women with breast implants may undergo implant removal. There are various reasons for implant removal, some of which include a desire to reduce breast size, capsular contracture, rupture, infection, and patient dissatisfaction. As many as 20% of women who undergo breast augmentation have their implant removed within 8 to 10 years.18 When an implant is explanted, the residual fibrous capsule may remain or it may be removed (capsulectomy). During explantation, it is considered oncologically safe to leave the capsule tissue behind.19 The decision to leave the capsule versus capsulectomy with explantation is surgeon preference, with consideration for capsulectomy also given to the initial implant and whether the capsule can be removed in its entirety. The mammographic sequelae of explantation are varied; in some degree they may depend on whether capsulectomy was performed. There may be no residual mammographic sequelae.20 A capsule that remains may be seen as a mass which can vary in size, shape and margins (Figure 16).21 The capsule may also contain calcifications. These findings are typically located in the mid-breast at posterior depth. If explantation was performed in the setting of extracapsular rupture, residual free silicone and/or silicone granulomas may remain (Figures 17 and 18).
Mammography certification/recommendations
As mammographic facilities must be certified by the U.S. Food and Drug Administration (FDA) and Mammography Quality Standards Act (MQSA), familiarity with their recommendations is also essential. Facilities that perform mammograms are required to ask a patient if she has breast implants, but they are not required to perform mammograms on these patients. Referrals of such patients to other facilities can be made, but they are not required. For facilities that perform mammography on patients with implants, displacement view techniques are not specified.22
For women with breast implants, the FDA recommends continued routine mammography, including implant-displaced views, as recommended by the patient’s healthcare provider based on age and risk factors. As previously described, intracapsular silicone rupture is not a mammographic diagnosis. It can also be difficult to make on clinical evaluation, which is why it has been called “silent rupture.” For this reason, the FDA recommends that women get a first breast MRI 3 years after receiving their implants and every 2 years thereafter to detect silent ruptures.23
Conclusion
Familiarity with breast implants is essential, as breast augmentation is a popular elective surgical option. An awareness and understanding of breast imaging positioning as related to the Eklund technique can help centers provide high-quality mammograms for women with breast implants. As women continue to choose this elective cosmetic option, radiologists must continue to improve their skills in mammographic interpretation. Patients with augmentation implants should be encouraged to participate in breast cancer screening programs according to the recommended guidelines.
REFERENCES
- Plastic surgery procedures continue steady growth in U.S. American Society of Plastic Surgeons. http://www.plasticsurgery.org/news/past-press-releases/2014-archives/plastic-surgery-procedures-continue-steady-growth-in-us.html. Published February 26, 2014. Accessed October 21, 2014.
- Eklund GW, Busby RC, Miller SH, et al. Improved imaging of the augmented breast. AJR Am J Roentgenol. 1988;151(3):469-473.
- Venkataraman S, Hines N, Slanetz P. Challenges in mammography: part 2, multimodality review of breast augmentation-imaging findings and complications. AJR Am J Roentgenol. 2011;197(6):W1031-W1045.
- Breast augmentation procedure steps. American Society of Plastic Surgeons Web site. http://www.plasticsurgery.org/cosmetic-procedures/breast-augmentation.html?sub=Breast+au gmentation+procedure+steps. Accessed October 21, 2014.
- Di Benedetto G, Cecchini S, Grassetti L, et al. Comparative study of breast implant rupture using mammography, sonography and magnetic resonance imaging: correlation with surgical findings. Breast J. 2008;14(6):532-537.
- Bassetti E, Pediconi F, Luciani ML, et al. Breast prosthesis: management of patients after plastic surgery. J of Ultrasound 2011;14(3):113-121.
- Juanpere S, Perez E, Huc O, et al. Imaging of breast implants — a pictorial review. Insights Imaging. 2011;2(6):653-670.
- Colombo G, Ruvolo V, Stifanese R, et al. Prosthetic breast implant rupture: imaging-pictorial essay. Aesthetic Plast Surg. 2011;35(5):891-900.
- Leibman AJ. Imaging of complications of augmentation mammoplasty. Plastic Reconstr Surg. 1994;93(6):1134-1140.
- Important Information for Augmentation Patients about Mentor Memory Gel Silicone Gel-Filled Breast Implants. Mentor Web site. http://www.mentorwwllc.com/pdf/approved/Augmentation.pdf. Accessed October 21, 2014.
- Brody GS, Deapen D, Taylor CR, et al. Anaplastic large cell lymphoma occurring in women with breast implants: analysis of 173 cases. Plastic Reconstr Surg. 2015;135(3):695-705.
- Peters W, Smith D. Calcification of breast implant capsules: incidence, diagnosis and contributing factors. Ann Plast Surg. 1995; 34(1):8-11.
- Oliveira VM, Roveda Junior D, Lucas FB, et al. Late seroma after breast augmentation with silicone prostheses: a case report. Breast J. 2007;13(4):421-423.
- Locke MB, Lofts J. Variable presentation of anaplastic large-cell lymphoma in patients with breast implants. ANZ J Surg. 2015;. Doi:10.1111/ans 13074. (Epub ahead of print).
- Center for Devices and Radiological Health USFaDA. Anaplastic Large Cell Lymphoma (ALCL) in Women with Breast Implants: Preliminary FDA Findings and Analysis. January 2011. http://www.fda.gov/downloads/MedicalDevices/Productsand%20MedicalProcedures/ImplantsandProsthetics/BreastImplants/UCM240003.pdf
- Hwang M, Brown H, Murrin R. Breast implant-associated anaplastic large cell lymphoma: a Case report and literature review. Aesthetic Plast Surg. 2015;39(3):391-395.
- Uematsu T. Screening and diagnosis of breast cancer in augmented women. Breast Cancer. 2008;15(2):159-164.
- Risks of breast implants. US Food and Drug Administration. http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/ImplantsandProsthetics/BreastImplants/ ucm064106.htm. Updated September 25, 2013. Accessed October 21, 2014.
- Lapid O, Noels EC, Meijer SL. Pathologic findings in primary capsulectomy specimens: analysis of 2351 patients. Aesthet Surg J. 2014;34(5):714-718.
- Hayes MK, Gold RH, Bassett LW. Mammographic findings after the removal of breast implants. AJR Am J Roentgenol. 1993;160(3):487-490.
- Stewart NR, Monsees BS, Destouet JM, et al. Mammographic appearance following implant removal. Radiology. 1992;185(1):83-85.
- Breast implants. US Food and Drug Administration. http://www.fda.gov/Radiation-EmittingProducts/MammographyQualityStandardsActandProgram/Guidance/PolicyGuidance-HelpSystem/ucm050244.htm. Updated June 25, 2014. Accessed October 6, 2014.
- FDA update on the safety of silicone gel filled breast implants. US Food and Drug Administration. http://www.fda.gov/downloads/MedicalDevices/ProductsandMedicalProcedures/ ImplantsandProsthetics/BreastImplants/UCM260090.pdf. Published June 2011. Accessed October 3, 2014.
Citation
MI Q, DR H, N M, B C, E R, LM R. Cosmetic breast augmentation: A review of mammographic findings. Appl Radiol. 2016;(2):26-33.
February 3, 2016